ORIF of Hip Fracture
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about open reduction and internal fixation (ORIF) of a hip fracture?
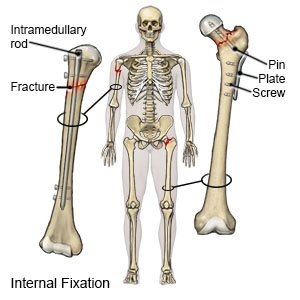
ORIF is surgery to fix a broken bone in your hip. A hip fracture is a break in the top of the femur or in the hip socket. The femur is the long bone in your thigh that attaches to your pelvis at the hip joint. Open reduction means that the bone is moved back into the right place with surgery. Internal fixation means that hardware (such as screws, rods, or pins) is used to hold the broken bones together. You may also need an implant to replace your hip socket. ORIF of a hip fracture is also called percutaneous hip pinning.
 |
How do I prepare for surgery?
- Your surgeon will tell you how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight on the day of surgery. Arrange to have someone drive you home when you are discharged.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine before surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- You may need blood or urine tests before your surgery. You may also need x-rays or an MRI of your hip. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the provider if you have any metal in or on your body.
What will happen during surgery?
- You may be given medicine to keep you asleep and free from pain during surgery. You may instead be given the medicine into your spine to numb the surgery area. You may also be given antibiotics to prevent infection. Your healthcare provider will make an incision on your hip to see the damaged femur. He or she will straighten your femur and put the broken pieces of bone together. He or she will use metal screws, bars, plates, or rods to hold the broken bones tightly together.
- Your surgeon will use an artificial implant to replace the head of your femur, if needed. It will be tightly fitted to the top of your femur. It may be secured with screws or cement. If your hip socket is badly damaged, it may also be replaced with an implant. X-rays may be taken during surgery to help your surgeon put your hip joint back together. X-rays can also show if the devices and implants are in the right places. A drain may be placed to carry blood and other fluids away from your hip joint. Your incision will be closed with stitches or staples and covered with a bandage.
What should I expect after surgery?
- You will stay in the hospital for several days. You will need to wear pressure stockings to help prevent blood clots. It will be important for you to get up and move after your surgery. Movement also helps prevent blood clots and pneumonia.
- A physical therapist will come and help you move the day after surgery. He or she will teach you how to use a walker or crutches. He or she will also give you exercises to do when you go home. After you go home, you will need to continue physical therapy.
What are the risks of ORIF of a hip fracture?
You may develop a life-threatening blood clot. You may have trouble walking without a walker or cane even after surgery. You may develop arthritis (joint inflammation) in your hip. Nerves may be injured. Your bone may not heal well or heal fully. You may have a limp if one leg becomes shorter than the other.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
