Opioid Use Disorder
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
What is opioid use disorder (OUD)?
OUD is a medical condition that develops from long-term use or misuse of an opioid. You are not able to stop taking the opioid even though it causes physical or social problems. OUD may be use of an opioid such as heroin or misuse of a prescription opioid such as fentanyl.
What are the signs and symptoms of OUD?
Signs and symptoms of OUD include at least 2 of the following in a 12-month period:
- You take an opioid in a way it was not intended. This is also called misuse. Examples of misuse include taking more than prescribed or taking it longer than recommended. Another example is taking it for a different reason than prescribed. Your prescription may be for pain relief, but you take it because it makes you feel good. Misuse can also mean you take the opioid even though you do not have a prescription for it.
- You have a strong urge or craving for the opioid. This is also called addiction. You spend large amounts of time trying to get, take, or recover from the opioid. You also spend time thinking about when you can take the opioid again.
- You become dependent on the opioid. Dependence means your body becomes used to the opioid. You have withdrawal symptoms when you do not take the opioid for a short amount of time. You have to take it to stop or prevent withdrawal symptoms, such as shaky hands.
- You become tolerant to the opioid. Tolerance means you continue to need higher amounts to feel the effects you want.
- You are not able to stop, or to take less. You start it again when you try to quit. You try to lower the amount or increase time without it, but you are not able.
- You continue the opioid even though it causes problems or is dangerous. For example, you drive even though the opioid makes you drowsy. You try to make the effect stronger by mixing the opioid with alcohol, medicines, or drugs. You have problems at school, work, or home. You spend less time doing important or enjoyable activities.
How is OUD diagnosed and treated?
Your healthcare provider will ask about the amount and type of opioids you had over the last 12 months. Your blood or urine may be used to check the level of opioid in your system. Your provider can help you make decisions about treatment. Treatment may be offered in a hospital, outpatient facility, or treatment center.
- Detoxification (detox) means healthcare providers will slowly decrease the amount of the opioid. Another opioid medicine, such as methadone, may be given to help decrease symptoms of withdrawal.
- Therapy may include work with a psychiatrist, psychologist, or therapist. Therapy can happen in group or individual sessions. Some therapy may include family members. Your healthcare provider or therapist may be able to help you find a support group in your area. A support group is a way to get help from others who have OUD.
What do I need to know about opioid safety?
- Do not suddenly stop the opioid. A sudden stop may cause dangerous side effects. Work with your healthcare provider to decrease the amount slowly.
- Do not take prescription opioids that belong to someone else. The kind or amount may not be right for you.
- Do not mix opioids with other medicines, drugs, or alcohol. The combination can cause poisoning, or cause you to stop breathing. Alcohol, sleeping pills, and medicines such as antihistamines can make you sleepy. A combination with opioids can lead to a coma.
- Learn about the signs of poisoning. Examples include slow breathing, pale or cold skin, and small pupils. Tell others about these signs so they will get help for you if needed. Talk to your healthcare provider about naloxone. You may be able to keep naloxone at home in case of poisoning. Your family and friends can also be trained on how to give it to you if needed.
- Take prescribed opioids exactly as directed. Do not take more than the recommended amount. Do not take it more often than recommended or for a different reason. Be sure to remove an old patch before you place a new one. Make sure the patch is not exposed to sunlight. Sunlight speeds up the opioid release from the patch.
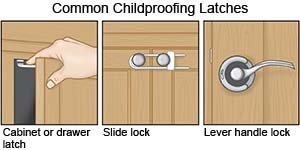
- Keep opioids out of the reach of children. Store opioids in a locked cabinet or in a location that children cannot get to.
- Follow instructions for what to do with leftover prescription opioids. Your healthcare provider will give you instructions for how to dispose of it safely. This helps make sure no one else gets to it.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Where can I get support and more information?
The following organizations provide information on opioid treatment programs near you:
- Substance Abuse and Mental Health Services Administration (SAMHSA)
PO Box 2345
Rockville , MD 20847-2345
Web Address: http://www.samhsa.gov or https://dpt2.samhsa.gov/treatment/
- National Institute on Drug Abuse
6001 Executive Boulevard, Room 5213
Bethesda , MD 20892-9561
Phone: 1- 301 - 443-1124
Web Address: www.nida.nih.gov
Call your local emergency number (911 in the US) or have someone call if:
- You have chest pain or trouble breathing.
- You have a seizure.
- You cannot be woken.
When should I seek immediate care?
- You have trouble staying awake and your breathing is slow or shallow.
- You have a fast, slow, or irregular heartbeat.
- You have pale or cold skin.
- You feel lightheaded or faint.
- Your speech is slurred, or you are confused.
When should I call my doctor?
- You have nausea and are vomiting, or you cannot stop vomiting.
- You have balance problems.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Opioid Use Disorder
- The Meaning of Drug Toxicology Reports and Tests
- Tramadol - Top 8 Things You Need to Know
- What is a Boxed Warning?
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
