Laparoscopic Myotomy and Fundoplication for Achalasia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about laparoscopic myotomy and fundoplication:
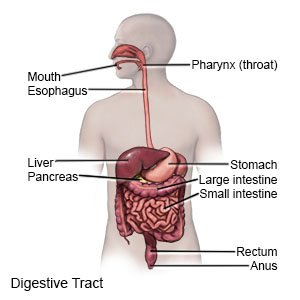
A laparoscopic myotomy is a procedure to open the valve between your esophagus and stomach. A fundoplication is a procedure to wrap part of your stomach around part of your esophagus. This prevents acid reflux. A laparoscope (tube with a camera on the end) is used to do the surgery, along with other tools.
 |
How to prepare for this procedure:
- Your healthcare provider will tell you how to prepare. Arrange to have someone drive you home after the procedure.
- You may need to be on a liquid diet for at least 24 hours before the procedure. Your provider will give you instructions for your liquid diet if it is recommended.
- Your provider will use a test called a manometry to measure muscle strength in your esophagus. He or she will tell you when to have the manometry and how to prepare.
- Tell your provider about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop.
- Tell your provider about all your allergies, including allergic reactions to anesthesia.
What will happen during this procedure:
- General anesthesia will be given to keep you asleep and free from pain during the procedure. Your healthcare provider will make 5 small incisions in your abdomen. He or she will do the procedure with a laparoscope put through the incisions.
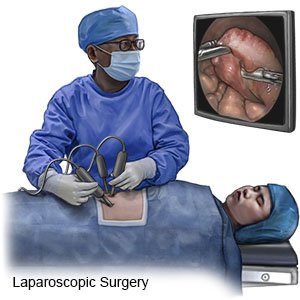
- Your provider will open the area between your esophagus and stomach. This will make it easier for food to get to your stomach when you to swallow. Then your provider will wrap part of your stomach around your esophagus. This prevents stomach acid from going up into your esophagus. Your provider will fix the part of your stomach in place with stitches.
- A drain may be placed to remove extra fluid from the surgery area. The incisions will be closed and covered with bandages to prevent an infection.
What to expect after this procedure:
- The procedure area may be swollen. You may also have pain. These should get better in a few days.
- You may have bloating for about a month.
- You may be able to have liquids or some foods the day after the procedure.
- Your healthcare provider will tell you if you should stay on a liquid diet after surgery. You may need to work up to solid foods.
- You will be given a list of foods to avoid for 2 weeks. These include meat, liquid that contains carbonation (such as soft drinks), and bread.
Risks of laparoscopic myotomy and fundoplication:
You may bleed more than expected. You may develop an infection in the procedure area, or in an organ. The inner lining of your esophagus may be perforated. This means holes are made in the lining. You may need antibiotics or another surgery to fix this problem. A hernia may develop where you had an incision. You may develop a bowel obstruction (blockage). Your intestines or a blood vessel may be injured. Your healthcare provider may change your procedure to open surgery if this happens. You may still have problems swallowing, or the problems may come back later. Some stomach acid may still go into your esophagus. You may develop dumping syndrome. This means food goes too fast from your stomach to your intestines. This can cause bloating, nausea, or diarrhea after you eat.
Seek care immediately if:
- You have a fever of 101°F (38.3°C) or higher or a fever with chills.
- You have severe pain in the procedure area.
- You see signs of an infection, such as swelling, red streaks, or pus.
- You have trouble swallowing.
- You have severe nausea and are vomiting.
Call your doctor if:
- You have a fever of 99°F (37.2°C) to 100.9°F (38.2°C).
- You have new or worsening pain, even after you take pain medicine.
- You have diarrhea or constipation.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Antacids may be needed if you continue to have acid reflux. Your healthcare provider will tell you when to take these and for how long to take them.
- Gas relief medicine may be recommended to relieve bloating. Your provider will tell you how many times each day to take these, and for how long to take them.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
- Eat foods and drink liquids as directed. Do not have meat, liquid that contains carbonation (such as soft drinks), or bread for 2 weeks, or as directed. Your healthcare provider may want you to stay on a liquid diet for a few days or weeks. He or she will give you specific instructions for a liquid diet.
- Care for the incision areas as directed. Your provider will tell you when you can remove any bandages covering the areas. He or she will tell you when it is okay to take a shower. You may need to keep the incision areas covered to prevent them from getting wet. Do not take a bath, swim, or soak in a hot tub until your provider says it is okay. Check the incision areas every day for signs of infection, such as swelling, red streaks, or pus.
- Follow your provider's directions for activity. He or she will tell you when you can drive, return to work, and do your regular activities. This should be within 2 weeks of your procedure. You may be able to drive sooner, if you are no longer taking opioid pain medicine. Do not lift anything heavy for 6 weeks, or as directed. Your provider may give you a weight limit for lifting. For example, he or she may say do not lift anything heavier than 5 pounds.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
