Knee Bursitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is knee bursitis?
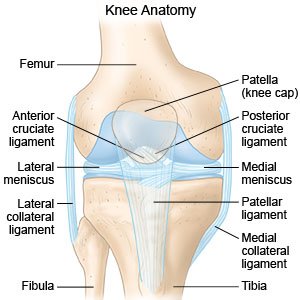
Knee bursitis is inflammation of the bursa in your knee. The bursa is a fluid-filled sac that acts as a cushion between a bone and a tendon. A tendon is a cord of strong tissue that connects muscles to bones.
 |
What increases my risk for knee bursitis?
- An injury, such as a fall
- Bacterial infection
- Overuse of your knees, such as when you run or jump
- Constant pressure on your knees, such as when you kneel to garden, clean the floor, or lay carpet
- Medical conditions, such as rheumatoid arthritis or gout
What are the signs and symptoms of knee bursitis?
- Pain, swelling, or tenderness in your knee
- Decreased movement or stiffness of your knee
- Red, warm, skin over your knee
- A grating or grinding sound or feeling when you move your knee
How is knee bursitis diagnosed?
Your healthcare provider will examine your knee and ask about your injury or activities. You may need any of the following:
- Blood tests may show signs of infection or a disease such as rheumatoid arthritis.
- X-ray or MRI pictures may show bone position problems, arthritis, or a fracture. You may be given contrast liquid to help your knee show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- A sample of fluid from your knee may tested for signs of infection. Removal of bursa fluid may also help relieve your symptoms.
How is knee bursitis treated?
- Medicines:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Aspirin helps relieve pain and swelling. Take aspirin exactly as directed by your healthcare provider.
- Antibiotics help fight an infection caused by bacteria.
- Steroids help relieve pain and swelling. Steroid injections are given directly into the painful area. Steroid pills may be given for a short time.
- Surgery may be used to remove your bursa. Surgery is only done when other treatments do not work.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Rest your knee as much as possible to decrease pain and swelling. Slowly start to do more each day. Return to your daily activities as directed.
- Apply ice to help decrease swelling and pain. Ice may also help prevent tissue damage. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel and place it on your knee for 15 to 20 minutes, 3 to 4 times each day, as directed.
- Apply heat to help decrease pain and stiffness. Apply heat on the area for 15 to 20 minutes, 3 to 4 times each day, as directed.
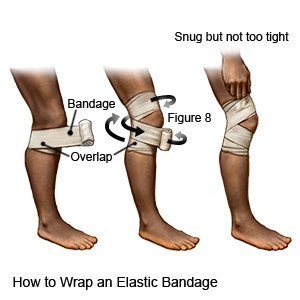
- Apply compression to decrease swelling. Healthcare providers may wrap your knee with tape or an elastic bandage to decrease swelling. Loosen the elastic bandage if you start to lose feeling in your toes.
- Elevate your knee above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your lower leg on pillows or blankets to keep it elevated comfortably. Do not put the pillow directly under your knee.

- Go to physical therapy, if directed. A physical therapist can teach you exercises to improve your range of motion and increase knee strength.
How can I prevent knee bursitis?
- Stretch, warm up, and cool down when you exercise. This will help loosen your muscles and decrease stress on your knees. Rest between workouts.
- Protect your knees. Use kneepads when you kneel on a hard surface and when you play sports. Stand and walk around every 20 minutes if you have to kneel for a long period of time.
When should I call my doctor?
- Your pain and swelling increase.
- Your symptoms do not improve with treatment.
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Knee Bursitis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
