Endotracheal Tube
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about an endotracheal tube?
An endotracheal (ET) tube is a hollow plastic tube that is placed in your trachea through your mouth. The trachea is also called the windpipe or airway. The ET tube is attached to a machine called a respirator. A respirator gives you oxygen and breathes for you when you cannot breathe on your own.
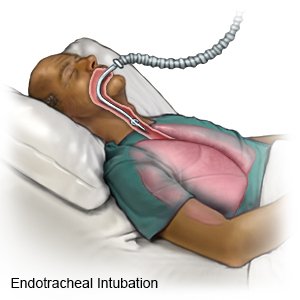 |
Why might I need an ET tube?
You may need an ET tube if you are not able to breathe enough oxygen on your own. This can occur if you have an injury, serious illness, or a heart attack. An ET tube may also be used during surgery.
How is an ET tube inserted?
- You will be asleep before your provider inserts the ET tube. He or she will take measurements of your mouth, neck, and chest to see how deep the ET tube should be placed. You will get extra oxygen before the ET tube is inserted. A device may be used to help guide the ET tube into place. Your provider will put the ET tube in your mouth, past your vocal cords, and into your trachea. The tube may have a balloon at the end that is filled with air to hold the tube in place. The tube will be secured to your mouth with medical tape. The ET tube will be attached to a respirator that will breathe for you.
- After the ET tube is put in, your provider will make sure the tube is in the right place. He or she will listen for breathing sounds in your lungs and watch for chest movement. He or she may measure the level of carbon dioxide you are breathing out. A small camera may be put down into the ET tube to check placement. An ultrasound or x-ray may also be used to check if the ET tube is in the right place.
When is the ET tube removed?
The ET tube will be removed when you are able to breathe on your own. You may be awake or waking up as the tube is removed.
What are the risks of an ET tube?
You may have abnormal heartbeats. The tube may cause damage to your mouth, teeth, vocal cords, or trachea. The tube may be placed into your esophagus (the passage from your mouth to your stomach). If this happens, you may vomit, and fluid may enter your lungs and cause an infection. The tube may be placed too far into your trachea or be dislodged. You may not get the oxygen you need. Decreased levels of oxygen can lead to permanent organ or brain damage and be life-threatening.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
