Hypertension in the Older Adult
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
Hypertension is high blood pressure. Blood pressure often increases with age, but hypertension is not a normal part of aging. You may be able to control your blood pressure with lifestyle changes, medicines, or both. Hypertension that does not respond to medicines and lifestyle changes is called resistant hypertension. Hypertension is considered chronic when it continues for 3 months or longer.
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) or have someone call if:
- You have chest pain.
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You become confused or have trouble speaking.
- You suddenly feel lightheaded or have trouble breathing.
Seek care immediately if:
- You have a severe headache or vision loss.
- You have weakness in an arm or leg.
- You get dizzy and fall.
Call your doctor if:
- You feel faint, dizzy, confused, or drowsy.
- You have been taking your blood pressure medicine but your pressure is higher than your provider says it should be.
- Your blood pressure is lower than your healthcare provider said it should be.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Medicine may be used to help lower your blood pressure. You may need more than one type of medicine.
- Diuretics help decrease extra fluid that collects in your body. This will help lower your blood pressure. You may urinate more often while you take this medicine.
- Cholesterol medicine helps lower your cholesterol level. A low cholesterol level helps prevent heart disease and makes it easier to control your blood pressure.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
What you need to know about the stages of hypertension:
Your healthcare provider will give you a blood pressure goal based on your age, health, and risk for cardiovascular disease. The following are general guidelines on the stages of hypertension:
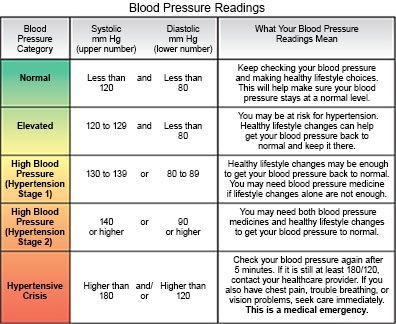 |
- Normal blood pressure is 119/79 or lower . Your healthcare provider may only check your blood pressure each year if it stays at a normal level.
- Elevated blood pressure is 120/79 to 129/79 . This is sometimes called prehypertension. Your healthcare provider may suggest lifestyle changes to help lower your blood pressure to a normal level. He or she may then check it again in 3 to 6 months.
- Stage 1 hypertension is 130/80 to 139/89 . Your provider may recommend lifestyle changes, medication, and checks every 3 to 6 months until your blood pressure is controlled.
- Stage 2 hypertension is 140/90 or higher . Treatment may include lifestyle changes and medicines to lower your blood pressure. You will also need to have your blood pressure checked monthly until it is controlled.
Manage hypertension:
- Check your blood pressure at home. Avoid smoking, caffeine, and exercise at least 30 minutes before checking your blood pressure. Sit and rest for 5 minutes before you take your blood pressure. Extend your arm and support it on a flat surface. Your arm should be at the same level as your heart. Follow the directions that came with your blood pressure monitor. Check your blood pressure 2 times, 1 minute apart, before you take your medicine in the morning. Also check your blood pressure before your evening meal. Keep a record of your readings and bring it to your follow-up visits. Ask your healthcare provider what your blood pressure should be.

- Manage any other health conditions you have. Health conditions such as diabetes can increase your risk for hypertension. Follow your healthcare provider's instructions and take all your medicines as directed.
- Ask about all medicines. Certain medicines can increase your blood pressure. Examples include decongestants, herbal supplements, and NSAIDs, such as ibuprofen. Your healthcare provider can tell you which medicines are safe for you to take. This includes prescription and over-the-counter medicines. You may also be taking several prescription medicines for other health conditions. It is important for your healthcare provider to know all your current medicines. Bring a list of your medicines or the pill bottles with you to follow-up visits. This will help your healthcare provider manage your current prescriptions and order new prescriptions.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
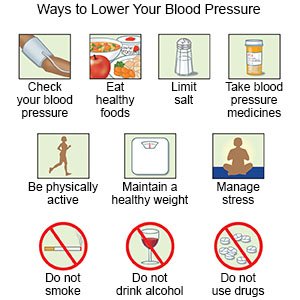
Lifestyle changes you can make to manage hypertension:
Your healthcare provider may recommend you work with a team to manage hypertension. The team may include medical experts such as a dietitian, an exercise or physical therapist, and a behavior therapist. Your family members may be included in helping you create lifestyle changes, such as the following:
 |
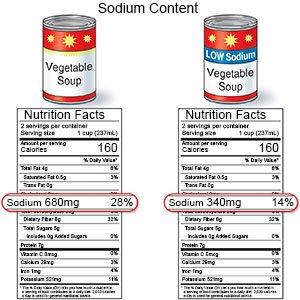
- Limit sodium (salt) as directed. Too much sodium can affect your fluid balance. Your heart works too hard if you have too much fluid in your body. Even if you lower your daily sodium intake by 1,000 mg, it can help. For example, if you cook with salt, do not add any to your food at the table. Check labels to find low-sodium or no-salt-added foods. Some low-sodium foods use potassium salts for flavor. Too much potassium can also cause health problems. Your healthcare provider will tell you how much sodium and potassium are safe for you to have in a day. He or she may recommend that you limit sodium to 2,000 to 2,300 mg a day.
- Follow the meal plan recommended by your healthcare provider. A dietitian or your provider can give you more information on low-sodium plans or the DASH (Dietary Approaches to Stop Hypertension) eating plan. The DASH plan is low in sodium, processed sugar, unhealthy fats, and total fat. It is high in potassium, calcium, and fiber. These can be found in vegetables, fruit, and whole-grain foods.

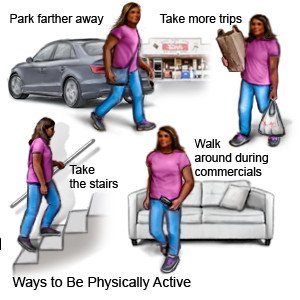
- Be physically active throughout the day. Physical activity, such as exercise, can help control your blood pressure and your weight. Be physically active for at least 30 minutes per day, on most days of the week. Examples of physical activity include walking, swimming, gardening, and riding a bicycle. Your healthcare providers can help you create a physical activity plan.

- Decrease stress. This may help lower your blood pressure. Learn ways to relax, such as deep breathing or listening to music. Talk to your provider if you have trouble sleeping. Sleep is important for blood pressure management.
- Limit alcohol as directed. Alcohol can increase your blood pressure. Ask your healthcare provider if it is okay for you to drink alcohol. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor. Your provider can tell you how many drinks are okay to have within 24 hours or within 1 week.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase your blood pressure and also cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Follow up with your doctor or cardiologist as directed:
You will need to return to have your blood pressure checked. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Hypertension
- Do blood pressure drugs interact with alcohol?
- FDA-Approved Weight Loss Drugs: Can They Help You?
- Which Drugs Cause Weight Gain?
Treatment options
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
