Hyperosmolar Hyperglycemic State
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is hyperosmolar hyperglycemic state?
Hyperosmolar hyperglycemic state (HHS) is a serious medical condition that develops if your blood sugar levels get very high. Your body gets rid of the extra sugar through your urine. This leads to severe dehydration. HHS can occur in people with type 1 or type 2 diabetes, but is more common in people with type 2 diabetes.
What causes HHS?
HHS usually develops because of other illnesses or conditions that cause blood sugar levels to rise, such as the following:
- Not taking insulin or diabetes medication as directed
- Infections such as pneumonia and urinary tract infections
- Stroke or heart attack
- Appendicitis (inflammation of your appendix) and pancreatitis (inflammation of the pancreas)
- Certain medicines such as diuretics, steroids, or beta blockers
- Alcohol abuse and cocaine use
What are the signs and symptoms of HHS?
Signs and symptoms of HHS usually develop over days or weeks. You may have any of the following:
- Blood sugar level above 600 mg/dL
- Frequent urination
- More thirst than usual or a dry mouth
- Blurred vision or vision loss
- Fatigue and weakness
- Fever
- Dizziness, drowsiness, or confusion
- Weight loss
- Seizures
How is HHS diagnosed?
Your healthcare provider will ask about your symptoms and when they started. He or she may also ask about other health conditions you have and about medicines that you take. Your blood and urine will be tested to check your blood sugar level and ketones. Your healthcare provider will also check for signs of dehydration, infection, or other conditions that may have led to HHS.
How is HHS treated?
HHS can be treated and controlled most of the time, but early treatment is very important. You may need to stay in the hospital for treatment. Healthcare providers will first treat dehydration by giving you fluids and electrolytes, such as potassium, through an IV. Healthcare providers will also give you insulin to help lower your blood sugar level. Healthcare providers may also need to treat other conditions that led to HHS.
How can I prevent HHS?
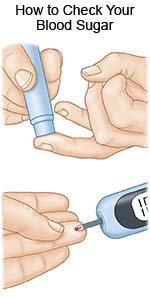
- Check your blood sugar level regularly. Ask your healthcare provider for information about how to check your blood sugar and how often to check it. He or she will tell you what your blood glucose level should be.
- Take your insulin or diabetes medicine as directed. This will help you to control your blood sugar levels. Tell your healthcare provider if the medicines are causing side effects or are not working well. Do not stop taking your insulin or medicines before you talk to your healthcare provider.
- Prepare for sick days. Your blood sugar levels increase when you are sick. Planning for sick days can keep your blood sugar levels from getting too high. Talk to your healthcare provider about a sick day plan that works best for you. Your healthcare provider may suggest any of the following:
- Check your blood sugar more often than usual. You may need to check your blood sugar level at least 4 times each day if you have type 2 diabetes. You may need to check even more often if you have type 1 diabetes.
- Check for ketones. You can check for ketones in your urine or blood at home. Ketone test kits are sold in pharmacies and some stores. Ask your healthcare provider which type of ketone testing is best for you. Your healthcare provider will tell you when and how often to check ketones.
- Take your insulin or diabetes medicine as directed. Take your medicine, even if you do not feel well and are eating less than usual. They help to keep your blood sugar under control. Talk to your healthcare provider before you make any changes to your dose of insulin or diabetes medicine.
- Continue your normal meal plan if you can. Eat your regular meals and drink plenty of liquids, such as water and caffeine-free diet drinks. If you cannot continue your meal plan, eat other foods that are easier for your body to digest. These foods include apple sauce, gelatin, crackers, soup, pudding, and yogurt. If you cannot eat these foods, drink liquids with calories in them instead. Some liquids that have calories include juice, broth, and regular soft drinks.
- Get help from others if you are older and live alone. Older adults are at increased risk of HHS. Have someone visit you regularly if you live alone. The visitor should watch for signs and symptoms of high blood sugar. The visitor should also remind you to drink enough liquids. It may be helpful to write down the amount of liquids you drink each day.
Call 911 for any of the following:
- You have a seizure.
- You begin to breathe fast, or are short of breath.
- You become weak and confused.
When should I seek immediate care?
- You are urinating more often than usual.
- You are more thirsty than usual.
- You are more drowsy than usual.
When should I contact my healthcare provider?
- Your blood sugar levels are higher than your healthcare provider says they should be.
- You have blurred vision.
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Hyperosmolar Hyperglycemic State
Treatment options
- Medications for Diabetic Coma
- Medications for Diabetic Coma, in DM Type I
- Medications for Diabetic Coma, in DM Type II
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
