Hydrocephalus
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is hydrocephalus?
Hydrocephalus is a condition caused by too much cerebrospinal fluid (CSF) inside the ventricles of your brain. Ventricles are spaces inside the brain where cerebrospinal fluid (CSF) is made and held. CSF surrounds and helps cushion your brain and spinal cord. CSF also provides nutrients to your nervous system. CSF is constantly being made and absorbed by your body. CSF moves through ventricles before it drains out and gets absorbed into your bloodstream. When CSF cannot drain properly, the fluid pressure may cause the ventricles to swell.
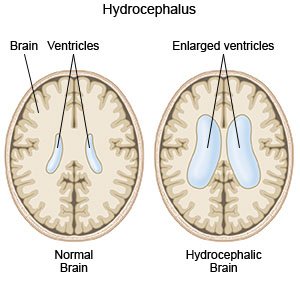 |
What increases my risk for hydrocephalus?
You may have been born with hydrocephalus. The following can also increase your risk:
- A brain injury or bleeding in the ventricles
- Infections, such as meningitis (infected covering of the brain or spinal cord) or ventriculitis (infected ventricles)
- Tumors or cysts that block the flow of CSF
- Aqueductal stenosis (narrowed passage between 2 ventricles), a condition you are born with that increases your risk as an adult
What are the signs and symptoms of hydrocephalus?
Signs and symptoms may be mild at first and get worse over time:
- Headache or dizziness
- Problems walking
- Nausea or vomiting
- Double vision
- Urinary problems, such as needing to urinate often or urgently, or leaking urine
- Sleepiness or fatigue
- Seizures or loss of consciousness
- Thinking or memory problems
How is hydrocephalus diagnosed?
- Neuro signs , or neuro checks show healthcare providers your brain function. They will check your eye movements and how your pupils react to light. They may check your memory and how easily you wake up. Your strength, balance, vision, and other brain functions may also be tested.
- Blood tests may show infection and inflammation.
- A CT or MRI may show bleeding, extra fluid, or blockage. You may be given contrast liquid to help your brain show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- A lumbar puncture , or spinal tap, is a procedure to collect a sample of CSF fluid to check for infection or test CSF pressure.
- Lumbar drainage is a procedure used to drain CSF fluid to see if your symptoms get better. Healthcare providers use a needle to insert a catheter (tube) to drain CSF from around your spine for up to 5 days. You must stay in the hospital during this test.
- Intracranial pressure (ICP) monitoring measures the pressure inside your skull. A small tube is put through your skull. The other end is connected to a monitor.
- Cisternography is a test to watch how CSF moves through your brain and spinal canal. The test takes 1 to 3 days.
How is hydrocephalus treated?
- Surgery:
- Tumor or cyst removal may help relieve a blockage and improve your symptoms.
- Shunt placement helps drain extra CSF fluid through a tube from your brain into your abdomen where it is absorbed.
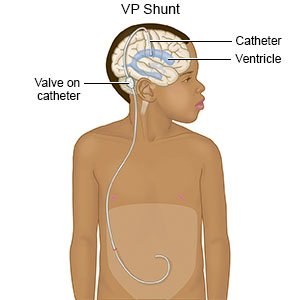
- Ventriculostomy helps drain the extra CSF fluid through a small hole in your brain.
- Medicines can help decrease inflammation or treat a bacterial infection. Medicines may also lower the amount of CSF your body makes.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How do I manage hydrocephalus?
- Keep your follow-up visits. Ask your healthcare provider when to return for follow-up visits. You may need CT scans every 2 to 3 weeks at first. Write down your questions so you remember to ask them during your visits.
- Keep a record of your headaches. Rate your headache, such as from mild to severe. Write down what you were doing when the headache started. Also note when you have been sitting or standing for a long time. Healthcare providers may use the headache record to change your treatment if needed.
- Report weight changes. Tell your healthcare providers if you gain or lose weight. Your shunt valve may need adjustment.
Call your local emergency number (911 in the US), or have someone call if:
- You had a seizure.
- You feel sleepy, or have problems waking.
When should I seek immediate care?
- You have nausea or are vomiting, even after treatment.
- You feel dizzy or your vision changes.
- You have headaches do not get better, even after you take medicine.
- You have a fever and a stiff neck, or you feel confused.
When should I call my doctor?
- You have a fever.
- Your neck and shoulders feel sore.
- The skin around your shunt looks red and feels tender.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Hydrocephalus
Treatment options
- Medications for Brain Anomalies incl Congenital
- Medications for Central Nervous System Disorders
- Medications for Hydrocephalus
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
