Guillain-Barre Syndrome
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Guillain-Barré syndrome (GBS) is a rare condition that causes damage to nerves that control movement and your sense of touch. You may have mild symptoms, such as muscle weakness. You may have more serious symptoms, such as paralysis.
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
Intake and output
may be measured. Healthcare providers will keep track of the amount of liquid you are getting. They also may need to know how much you are urinating. Ask healthcare providers if they need to measure or collect your urine.
A Foley catheter
is a tube put into your bladder to drain urine into a bag. Keep the bag below your waist. This will prevent urine from flowing back into your bladder and causing an infection or other problems. Also, keep the tube free of kinks so the urine will drain properly. Do not pull on the catheter. This can cause pain and bleeding, and may cause the catheter to come out.
Take deep breaths and cough 10 times each hour.
This will decrease your risk for a lung infection. Take a deep breath and hold it for as long as you can. Let the air out and then cough strongly. Deep breaths help open your airway. You may be given an incentive spirometer to help you take deep breaths. Put the plastic piece in your mouth and take a slow, deep breath, then let the air out and cough. Repeat these steps 10 times every hour.
Activity:
Your healthcare provider will tell you when it is okay to get out of bed. Have a healthcare provider help you the first time you get out of bed. If you feel weak or dizzy, sit or lie down right away. When you are strong enough, you may begin leg exercises in bed. Move your legs, ankles, and feet as directed while you are in bed. This may help prevent blood clots.
Medicines:
- Immune globulins decrease damage to your nerves.
- Antibiotics treat or prevent an infection caused by bacteria.
- Blood thinners help prevent blood clots. Blood thinners may be given before, during, and after a surgery or procedure. Blood thinners make it more likely for you to bleed or bruise.
- Heart medicine may be given to help your heart beat more regularly.
- Pain medicine may be given. Do not wait until the pain is severe before you ask for more medicine.
- Stool softeners help soften your bowel movements, decrease straining, and prevent constipation.
Tests:
- Blood and urine samples are sent to a lab to help find the cause of your symptoms. They may also be used to make sure organs, such as your liver and kidneys, are working correctly.
- An x-ray may be used to check your heart and lungs.
- A lumbar puncture (spinal tap) is a procedure to take a sample of fluid from around your spinal cord. The fluid will be sent to a lab to be tested for cause of your symptoms.
- An electromyography (EMG) test measures the electrical activity of your muscles at rest and with movement.
- Nerve conduction studies measure how your nerves respond to stimulation. Electrodes (wires) are placed on affected areas of your body. They send electrical currents into the nerve to see how quickly it responds.
- A neurologic exam tests how well your brain is working during your illness. Healthcare providers will check how your pupils react to light. They may check your memory and how easily you wake up. Your hand grasp and balance may also be tested.
- Pulmonary function tests (PFTs) show how well your body uses oxygen. You breathe into a mouthpiece connected to a machine. The machine measures how much air you breathe in and out over a certain amount of time.
Treatment:
Treatment depends on the type and severity of your symptoms:
- Plasmapheresis is a procedure to remove antibodies from your blood. Antibodies attack your nerve cells. Some of your blood will be removed through an IV. The blood is then put in a machine that spins and separates the red blood cells from the antibodies. The cleaned blood is then put back in your body through the IV.
- A plasma exchange is a procedure that removes part of the blood, called plasma. The plasma is then replaced with other fluids.
- You may need extra oxygen if your blood oxygen level is lower than it should be. You may get oxygen through a mask placed over your nose and mouth or through small tubes placed in your nostrils. Ask your healthcare provider before you take off the mask or oxygen tubing.
- Breathing treatments may be needed to help open your airways so you can breathe easier. A machine is used to change liquid medicine into a mist. You will breathe the mist into your lungs through tubing and a mouthpiece. Inhaled mist medicines act quickly on your airways and lungs to relieve your symptoms.
- Postural drainage (PD) uses body position and gravity to help bring up sputum (mucus) from your lungs. Your healthcare provider will place you in different positions to help the sputum drain to larger air passages. Then you can cough it out more easily. Your healthcare provider may also lightly clap on your back and chest with his or her hands. The provider may also use a small machine that vibrates on your skin. This breaks up the sputum in your lungs, making it easier to cough up.
- A ventilator is a machine that breathes for you if you cannot breathe on your own.

- Thickened liquids may be given to help you swallow. You may also be fed by an IV or nasogastric (NG) tube. An NG tube is placed through your nose and goes down to your stomach. The tube may also go directly from the outside of your body into your stomach, called a gastrostomy tube.
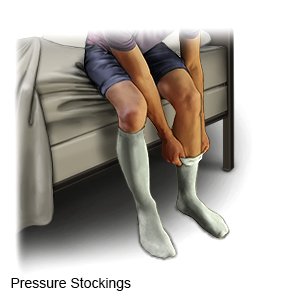
- Pressure stockings are long, tight stockings that put pressure on your legs to promote blood flow and prevent clots.
- Physical, occupational, or speech therapy may be needed. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain. An occupational therapist teaches you skills to use at home to help with your daily activities. You and home care providers may also be shown how to change your position often to prevent bedsores. A speech therapist may be able to help if you have problems with eating or swallowing. The therapist can teach you about which foods and liquids are safe to eat and drink.
RISKS:
GBS may lead to breathing problems and choking. You may develop blood clots. Blood clots may lead to other health problems. Even after treatment, you may have mild weakness. Without treatment, GBS may be life-threatening.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Guillain-Barre Syndrome
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
