Failure to Thrive in Older Adults
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Failure to thrive (FTT) happens when an older adult has a loss of appetite, eats and drinks less than usual, loses weight, and is less active than normal. He or she may not be interested in other people or social activities. He or she may also have memory loss, trouble thinking, and trouble with daily activities. Examples of daily activities include preparing meals, getting in and out of bed, walking, bathing, dressing, and using the bathroom.
DISCHARGE INSTRUCTIONS:
Return to the emergency department if:
- The person is not aware of his or her environment, is confused, or has hallucinations.
Call the person's doctor or specialist if:
- The person's symptoms get worse.
- The person has a fever.
- The person has signs of dehydration. Examples include dark yellow urine, dry mouth and lips, dry skin, fast heartbeat, and urinating less than usual.
- The person does not have an appetite or is losing weight.
- The person frequently complains of pain.
- The person has a change in behavior.
- The person has new difficulty swallowing.
- The person falls frequently.
- You or the person has questions or concerns about his or her condition or care.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Medicines:
- Medicines may be given to improve appetite and mood.
- Give the person's medicine as directed. Call the person's healthcare provider if you think the medicine is not helping or if the person has side effects. Tell the healthcare provider if the person is allergic to any medicine. Keep a list of the medicines, vitamins, and herbs the person takes. Include the amounts, and when and why he or she takes them. Bring the list or the pill bottles to follow-up visits.
Follow up with the person's doctor or specialist as directed:
The person may be referred to another healthcare provider such as a social worker or mental health specialist. Write down your questions so you remember to ask them during visits.
How to help a person with FTT:
- Offer foods that the person likes and are easy to eat. Offer healthy snacks and nutritional supplements between meals. These can provide extra calories and protein to increase energy and strength. Ask a dietitian for more information.

- Use herbs, spices, and flavor enhancers to add flavor to foods. Ask the healthcare provider or dietitian about flavor enhancers. Flavor enhancers with ham, natural bacon, and roast beef flavors can also be sprinkled on food to add flavor.
- Have the person drink liquids as directed to avoid dehydration. The person may be offered liquids between meals if they cause him or her to get full too quickly during meals. Ask how much liquid the person should drink each day and which liquids are best for him or her.
- Encourage social activities. Encourage the person to share meals with others as often as possible. Support from family and friends can give the person a sense of community and decrease feelings of loneliness.
- Talk with the healthcare provider about safe physical activities the person can do. Physical activity may help to increase the person's appetite. It may also help increase strength and improve balance.

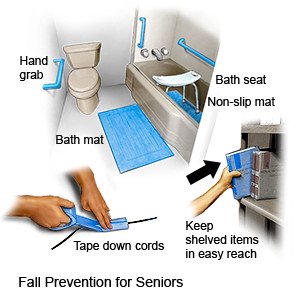
- Help prevent falls. Keep paths clear so the person will not trip on objects such as shoes, books, or electrical cords. Remove small rugs or secure them with double-sided tape. Install bright lights in the person's home and place items that are regularly used within reach.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Failure to Thrive
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
