Esophagitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
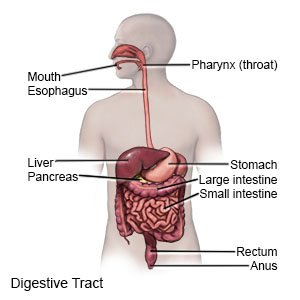
Esophagitis
is inflammation or irritation of the lining of the esophagus.
 |
Signs and symptoms of esophagitis
depend on the cause:
- Pain in the middle of your chest that may spread to your back
- Burning or pain in your esophagus, abdominal pain, or indigestion
- Trouble swallowing, or pain when you swallow
- A feeling that something is stuck in your esophagus
- Sore throat, a cough, or hoarseness
- Gagging, drooling, or wheezing
- Mouth sores (white patches), a bad taste in your mouth, or bad breath
- Nausea or vomiting
- Feeding problems or failure to thrive (young children)
Call your local emergency number (911 in the US) for any of the following:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
Seek care immediately if:
- You feel like you have food stuck in your throat and you cannot cough it out.
Call your doctor if:
- You have new or worsening symptoms, even after treatment.
- You have questions or concerns about your condition or care.
Treatment
may help the lining of your esophagus heal and prevent serious complications. Treatment will depend on what is causing your esophagitis. Symptoms caused by a toxic object such as a button battery need immediate treatment. Less severe causes may not need treatment. You may need any of the following if symptoms continue or get worse:
- Medicines may be given to fight infection or to control stomach acid. Your healthcare provider may make changes to your medicines, such as changing it to a liquid form.
- An elimination diet may help you find foods that are causing your symptoms. You will stop eating certain foods that can cause esophagitis. Your healthcare provider will tell you to start eating them again one at a time. Each time you do not have symptoms, you will start eating another food from the list. Any food that does cause symptoms may be causing your esophagitis.
- Surgery may be needed if other treatments do not work. Part of your stomach can be wrapped to cover the valve between your stomach and esophagus. This helps prevent acid from backing up into your esophagus.
Manage or prevent esophagitis:
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can irritate and damage your esophagus. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Do not drink alcohol. Alcohol can irritate your esophagus. Talk to your healthcare provider if you need help to stop drinking.
- Limit or do not eat foods that can lead to esophagitis. Foods such as oranges and salsa can irritate your esophagus. Caffeine and chocolate can cause acid reflux. High-fat and fried foods make your stomach digest food more slowly. This increases the amount of stomach acid your esophagus is exposed to. Eat small meals, and drink water with your meals. Soft foods such as yogurt and applesauce may help soothe your throat. Do not eat for at least 3 hours before you go to bed.
- Drink more liquid when you take pills. Drink a full glass of water when you take your pills. Ask your healthcare provider if you can take your pills at least an hour before you go to bed.
- Prevent acid reflux. Do not bend over unless it is necessary. Acid may back up into your esophagus when you bend over. If possible, keep the head of your bed elevated while you sleep. This will help keep acid from backing up. Manage stress. Stress can make your symptoms worse or cause stomach acid to back up.
- Keep batteries and similar objects out of the reach of children. Babies often put items in their mouths to explore them. Button batteries are easy to swallow and can cause serious damage. Keep the battery covers of electronic devices such as remote controls taped closed. Store all batteries and toxic materials where children cannot get to them. Use childproof locks to keep children away from dangerous materials.
Follow up with your doctor as directed:
Your doctor may refer you to a stomach specialist, allergist, or dietitian. You may need ongoing tests or treatment. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Esophagitis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
