Dyspnea
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Dyspnea is breathing difficulty or discomfort. You may have labored, painful, or shallow breathing. You may feel breathless or short of breath. Dyspnea can occur during rest or with activity. You may have dyspnea for a short time, or it might become chronic. Dyspnea is often a symptom of a disease or condition.
DISCHARGE INSTRUCTIONS:
Return to the emergency department if:
- Your signs and symptoms are the same or worse within 24 hours of treatment.
- You have shaking chills or a fever over 102°F.
- You have new pain, pressure, or tightness in your chest.
- You have a new or worse cough or wheezing, or you cough up blood.
- You feel like you cannot get enough air.
- The skin over your ribs or on your neck sinks in when you breathe.
- You have a severe headache with vomiting and abdominal pain.
- You feel confused or dizzy.
Call your doctor or specialist if:
- You have questions or concerns about your condition or care.
Medicines:
- Medicines may be used to treat the cause of your dyspnea. Medicines may reduce swelling in your airway or decrease extra fluid from around your heart or lungs. Other medicines may be used to decrease anxiety and help you feel calm and relaxed.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Manage long-term dyspnea:
- Create an action plan. You and your healthcare provider can work together to create a plan for how to handle episodes of dyspnea. The plan can include daily activities, treatment changes, and what to do if you have severe breathing problems.
- Lean forward on your elbows when you sit. This helps your lungs expand and may make it easier to breathe.
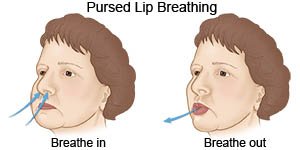
- Use pursed-lip breathing any time you feel short of breath. Breathe in through your nose and then slowly breathe out through your mouth with your lips slightly puckered. It should take you twice as long to breathe out as it did to breathe in.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage and make it harder to breathe. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Reach or maintain a healthy weight. Your healthcare provider can help you create a safe weight loss plan if you are overweight.
- Exercise as directed. Exercise can help your lungs work more easily. Exercise can also help you lose weight if needed. Try to get at least 30 minutes of exercise most days of the week. Your healthcare provider can help you create an exercise plan that is safe for you.
Follow up with your doctor or specialist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Dyspnea
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
