Covid-19 and Chronic Health Conditions
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about coronavirus disease 2019 (COVID-19) and chronic health conditions?
Your chronic condition may increase your risk for COVID-19 or serious problems it can cause. You can take steps to manage your condition. The steps will also lower your risk for COVID-19 or the serious problems it causes. If you do develop COVID-19, healthcare providers will tell you when it is okay to be around others after you recover. This depends on your chronic condition, any symptoms of COVID-19 that developed, and how severe the symptoms were.
What do I need to know about serious problems from the virus?
You may develop long-term health problems caused by the virus. Your risk is higher if you are 65 or older. A weak immune system, obesity, diabetes, chronic kidney disease, or a heart or lung condition can also increase your risk. Your risk is also higher if you currently use cigarettes or used them in the past. Your healthcare provider may give you medicine to prevent serious problems from the virus. COVID-19 can lead to any of the following:
- Multisymptom inflammatory syndrome in adults (MIS-A) or in children (MIS-C), causing inflammation in the heart, digestive system, skin, or brain
- Shortness of breath, serious lower respiratory conditions, such as pneumonia or acute respiratory distress syndrome (ARDS)
- Blood clots or blood vessel damage
- Organ damage from a lack of oxygen or from blood clots
- Sleep problems
- Problems thinking clearly, remembering information, or concentrating
- Mood changes, depression, or anxiety
- Long-term problems tasting or smelling
- Loss of appetite and weight loss
- Nerve pain
- Fatigue (feeling mentally and physically tired)
How does the virus spread?
The virus can be spread starting 2 to 3 days before symptoms begin. Close personal contact with an infected person increases your risk for infection. This means being within 6 feet (2 meters) of the person for at least 15 minutes over 24 hours.
- The virus travels in droplets that form when a person talks, sings, coughs, or sneezes. The droplets can also float in the air for minutes or hours. Infection happens when you breathe in the droplets or get them in your eyes or nose.
- Person-to-person contact can spread the virus. For example, a person with the virus on his or her hands can spread it by shaking hands with someone.
- The virus can stay on objects and surfaces for hours to days. You may become infected by touching the object or surface and then touching your eyes or mouth.
What do I need to know about the signs and symptoms of COVID-19?
Signs and symptoms usually start about 5 days after infection but can take 2 to 14 days. Signs and symptoms range from mild to severe. You may feel like you have the flu or a bad cold. Your chronic health condition may cause some of the same symptoms COVID-19 causes. This can make it hard to know if a symptom is from COVID-19 or your chronic condition. Tell your healthcare provider if you have any new or worsening symptoms. This is especially important if you have a condition that often causes shortness of breath. Your provider can tell you if you should be tested for COVID-19. Tell your provider if you think you were infected but develop signs or symptoms not listed below:
- A cough
- Shortness of breath or trouble breathing that may become severe
- A fever of at least 100.4°F, or 38°C (may be lower in adults 65 or older)
- Chills that might include shaking
- Muscle pain, body aches, or a headache
- A sore throat
- Suddenly not being able to taste or smell anything
- Feeling very tired (fatigue)
- Congestion (stuffy head and nose), or a runny nose
- Diarrhea, nausea, or vomiting
What can I do to manage my chronic health condition?
If you do not have a regular healthcare provider, experts recommend you contact a local community health center or health department. The following can help you manage your condition and prevent COVID-19 during an active outbreak in your area:
- Get emergency care for your condition if needed. Talk to your healthcare providers about symptoms of your chronic condition that need immediate care. Your providers can help you create a plan or add exacerbation management to your plan. The plan will include when to go to an emergency department and when to call your local emergency number. This will depend on where you live and the services that are available.
- Go to dialysis appointments as scheduled. It is important to stay on schedule. You will need to have enough food to be able to follow the emergency diet plan if you must miss a session. The emergency diet needs to be part of the management plan for your condition.
- Ask your healthcare provider for other ways to have appointments. Some providers offer phone, video, or other types of appointments.
- Follow any regular management plan you use. Your healthcare provider will tell you if you need to make any changes to your regular management plan. For example, if you have asthma, continue to follow your asthma action plan. If you have diabetes, you may need to check your blood sugar level more often. Stress and illness can make blood sugar levels go up. You may need to adjust medicine such as insulin. If you have a heart condition or high blood pressure, you may need to check your blood pressure more often. Stress and illness can also raise your blood pressure.
- Talk to your healthcare providers about your medicines. You may be able to get more than 1 month of medicine at a time. This will lower the number of times you need to go to a pharmacy to get your medicines. Make sure you have enough medicine if you have a condition that can lead to an emergency. Examples include asthma medicines, insulin, or an epinephrine pen. Check the expiration dates on the medicines you currently have. Ask for refills as soon as possible, if needed. If it is not time to refill prescriptions, you may be able to get an emergency supply of some medicines. Medicine plans vary, so ask your healthcare provider or pharmacist for options.
- Have supplies available in your home or delivered as needed. If possible, get extra supplies you use regularly. Examples include absorbent pads, syringes, and wound cleaning solutions. This will limit the number of trips out of your home to get supplies. Have food, medicines, and other supplies delivered. You can instead ask someone who does not have COVID-19 to get items you need.
What do I need to know about COVID-19 vaccines?
Your healthcare provider can give you more information about what to expect, depending on your chronic condition.
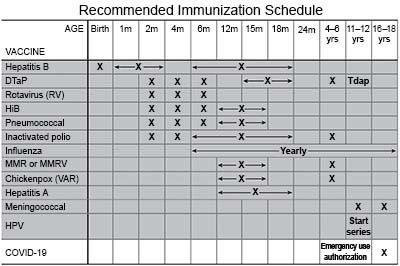
- Get a COVID-19 vaccine as directed. At least 1 dose of an updated vaccine is recommended for everyone 6 months or older. COVID-19 vaccines are given as a shot in 1 to 3 doses, depending on the age of the person who receives it. COVID-19 vaccines are updated throughout the year. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
- Continue to protect yourself and others. You can become infected even after you get the vaccine. You may also be able to pass the virus to others without knowing you are infected.
- After you get the vaccine, check local, national, and international travel rules. You may need to be tested before you travel. Some countries require proof of a negative test before you travel. You may also need to quarantine after you return.
- Medicine may be given to prevent infection. The medicine can be given if you are at high risk for infection and cannot get the vaccine. It can also be given if your immune system does not respond well to the vaccine.
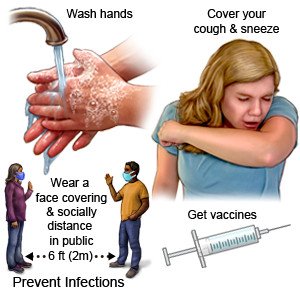
What can I do to lower my risk for COVID-19?
- Stay home if you are sick or think you may have COVID-19. It is important to stay home if you are waiting for a testing appointment or for test results.
- Wash your hands often throughout the day. Use soap and water. Rub your soapy hands together, lacing your fingers, for at least 20 seconds. Rinse with warm, running water. Dry your hands with a clean towel or paper towel. Use hand sanitizer that contains alcohol if soap and water are not available. Teach children how to wash their hands and use hand sanitizer.

- Cover sneezes and coughs. Turn your face away and cover your mouth and nose with a tissue. Throw the tissue away. Use the bend of your arm if a tissue is not available. Then wash your hands with soap and water or use hand sanitizer. Teach children how to cover a cough or sneeze.
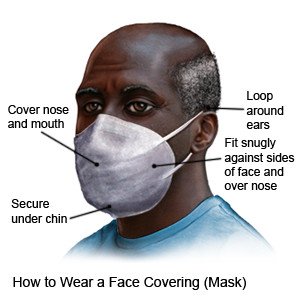
- Wear a face covering (mask) when needed. Use a cloth covering with at least 2 layers. You can also create layers by putting a cloth covering over a disposable non-medical mask. Cover your mouth and your nose.
- Try to keep space between you and others when you are out of the house. Avoid crowds as much as possible. Wear a face covering when you must be around a large group and cannot keep space between you and others.
- Clean and disinfect high-touch surfaces and objects in your home often. Use disinfecting wipes, or make a solution by mixing 4 teaspoons of bleach with 1 quart (4 cups) of water. Do not use any cleaning or disinfecting products that can trigger an asthma attack or other breathing problems. Open windows or have circulating air as you clean. Do not mix ammonia with bleach. This will create toxic fumes.
 |
What can I do to help strengthen my immune system?
- Ask about other vaccines you may need. Get the influenza (flu) vaccine as soon as recommended each year, usually starting in September or October. Get the pneumonia and respiratory syncytial virus (RSV) vaccines, if recommended. Your healthcare provider can tell you if you should also get other vaccines, and when to get them.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase your risk for infection and for serious COVID-19 effects. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Eat a variety of healthy foods. Examples include vegetables, fruits, whole-grain breads and cereals, lean meats and poultry, fish, low-fat dairy products, and cooked beans. Healthy foods contain nutrients that help keep your immune system strong.

- Find ways to manage stress. Talk to your healthcare providers about ways to manage stress. Stress can lead to breathing problems or trigger an attack or exacerbation of many health conditions. Do things you enjoy to help you relax. For example, talk to a friend, read a book or magazine, or listen to soothing music.
Where can I find more information?
- Centers for Disease Control and Prevention
1600 Clifton Road
Atlanta , GA 30333
Phone: 1- 404 - 6393311
Phone: 1- 800 - 3113435
Web Address: http://www.cdc.gov
Call your local emergency number (911 in the US) if:
- You have trouble breathing or shortness of breath.
- You have chest pain or pressure that lasts longer than 5 minutes.
- You become confused or hard to wake.
When should I seek immediate care?
- You have trouble staying awake during the day.
- Your nail beds, face, fingers, or toes look blue or darker than usual.
When should I call my doctor or specialist?
- You have a fever.
- You have symptoms of COVID-19.
- You have questions or concerns about COVID-19 or your chronic condition.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
