COPD: Prevent Exacerbations
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
AMBULATORY CARE:
An exacerbation of COPD
means your symptoms get much worse very quickly and can become life-threatening. Exacerbations can be triggered by infections such as a cold or the flu. Lung irritants such as air pollution, dust, fumes, or smoke can also be triggers.
Go to pulmonary rehabilitation (rehab) if directed:
Rehab is a program run by specialists who help you learn to manage COPD. Examples include a pulmonologist (lung specialist), dietitian, or exercise therapist. The specialists will help you make a plan to avoid triggers that cause an exacerbation.
Protect yourself from germs:
Germs can get into your lungs and cause an infection. An infection in your lungs can create more mucus and make it harder to breathe. An infection can also create swelling in your airway and prevent air from getting in. You can decrease your risk for infection by doing the following:
- Wash your hands often. Wash your hands several times each day. Wash after you use the bathroom, change a child's diaper, and before you prepare or eat food. Wash your hands for at least 20 seconds. Rinse with warm, running water. Then dry your hands with a clean towel or paper towel. Use hand sanitizer that contains alcohol if soap and water are not available.

- Always cover your mouth when you cough. Cough into a tissue or your shirtsleeve so you do not spread germs from your hands.
- Try to avoid people who have a cold or the flu. If you are sick, stay away from others as much as possible.
- Ask about vaccines you may need. Your healthcare provider may recommend these and other vaccines:
- Ask your healthcare provider about the flu and pneumonia vaccines. All adults should get the flu (influenza) vaccine as soon as recommended each year, usually in September or October. The pneumonia vaccine is recommended for all adults aged 50 or older to prevent pneumococcal disease, such as pneumonia. Adults aged 19 to 49 years who are at high risk for pneumococcal disease should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors.
- COVID-19 vaccines are given to adults as a shot. At least 1 dose of an updated vaccine is recommended for all adults. COVID-19 vaccines are updated throughout the year. Adults 65 or older need a second dose of updated vaccine at least 4 months after the first dose. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
Do not smoke:
Nicotine and other chemicals in cigarettes and cigars can cause lung damage and make your COPD worse. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Avoid secondhand smoke:
This is smoke another person exhales. Even if you have never smoked or have quit, it is important to avoid secondhand smoke. This smoke can also cause lung damage or trigger an exacerbation.
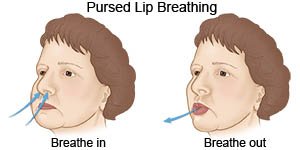
Use pursed-lip breathing any time you feel short of breath:
- Breathe in through your nose. Use the muscles in your abdomen to help fill your lungs with air.
- Slowly breathe out through your mouth with your lips slightly puckered. You should make a quiet hissing sound as you breathe out.
- Try to take 2 times as long to breathe out as to breathe in. This helps you get rid of as much air from your lungs as possible.
- Repeat this exercise several times. When you are used to doing pursed-lip breathing, you can do it any time you need more air.
Take your medicines as directed:
Your healthcare provider may prescribe medicine to help you breathe easier. It is important that you take your medicines as directed to prevent or stop an exacerbation. Refill your medicines before you are out so that you do not miss a dose. Talk to your healthcare provider or pharmacist if you have any questions about how to take your medicines.
- Short-acting bronchodilators may be called rescue inhalers or relievers. They relieve sudden, severe symptoms and start to work right away.
- Long-acting bronchodilators may be called controllers or maintenance medicine. This medicine helps open your airway over time. It is used to prevent breathing problems. Long-acting bronchodilators should not be used to treat sudden, severe symptoms, such as trouble breathing.
Avoid anything that makes your symptoms worse:
Stay out of high altitudes and places with high humidity. Stay inside, or cover your mouth and nose with a scarf when you are outside in cold weather. Stay inside on days when air pollution or pollen counts are high. Do not use aerosol sprays, such as deodorant, bug spray, and hairspray.
Exercise daily:
Exercise for at least 20 minutes each day to help increase your energy and decrease shortness of breath. Talk to your healthcare provider about the best exercise plan for you.
 |
Drink liquids as directed:
You may need to drink more liquid than usual. Liquid will help to keep your air passages moist and help you cough up mucus. Ask how much liquid to drink each day and which liquids are best for you.
Follow up with your doctor as directed:
You may need more tests. Your doctor may refer you to a specialist, depending on your needs. Some specialist services may be available through your pulmonary rehab program. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
