Contusion in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a contusion?
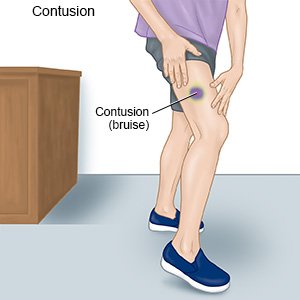
A contusion is a bruise that appears on your child's skin after an injury. A bruise happens when small blood vessels tear but skin does not. Blood leaks into nearby tissue, such as soft tissue or muscle.
 |
What increases my child's risk for a contusion?
- A disorder that makes him or her bleed more easily
- Kidney or liver disease, or an infection
- Medicines such as blood thinners or certain over-the-counter medicines and herbal medicines
- Weakened skin and muscles from nutrition problems
What are the signs and symptoms of a contusion?
- An area that may be black, blue, red, or darker than the skin around it
- Pain that increases when your child touches the bruise, walks, or uses the area around the bruise
- Swelling or a lump at the site of the bruise, or near it
- Stiffness or problems moving the bruised area
How is a contusion diagnosed?
Your child's healthcare provider may ask about any injuries, infections, or bleeding problems your child had. The provider will check the skin over the injured area. The provider may touch it to see where it hurts. The provider may also check for problems your child may have when he or she moves the bruised area. Your child may need any of the following:
- Blood tests may be used to check for blood disorders or to see how long it takes for your child's blood to clot.
- Ultrasound pictures may show how deep the bruise is and if any of your child's organs are injured.
- MRI pictures may show if a hematoma (pooling of blood) has started to form. Your child may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if your child has ever had an allergic reaction to contrast liquid. Do not let your child enter the MRI room with anything metal. The MRI machine uses a powerful magnet. Metal can cause serious injury from the magnet. Tell the healthcare provider if your child has any metal in or on his or her body.
How is a contusion treated?
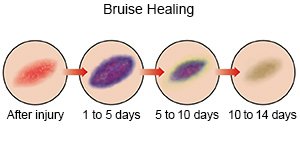
Treatment may not be needed. The bruise may become lighter or change to green or yellow as it heals. Treatment for a more severe injury may include any of the following:
- Medicine may be needed to treat or prevent pain or swelling.
- Aspiration is a procedure to drain pooled blood in your child's muscle. This helps prevent increased pressure in the muscle.
- Surgery may be done to repair a tear in your child's muscle or relieve pressure in the muscle caused by swelling.
 |
What may help my child's contusion heal?
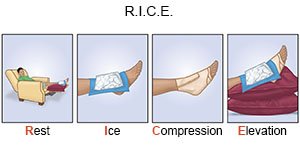
- Have your child rest the injured area or use it less than usual. If your child bruised a leg or foot, crutches may be needed. This will help your child keep weight off the injured body part.
- Apply ice to decrease swelling and pain. Ice may also help prevent tissue damage. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel and place it on your child's bruise for 15 to 20 minutes every hour or as directed.
- Use compression to support the area and decrease swelling. Wrap an elastic bandage around the area over the bruised muscle. Make sure the bandage is not too tight. You should be able to fit 1 finger between the bandage and your child's skin.
- Elevate (raise) the area above the level of your child's heart to help decrease pain and swelling. Use pillows, blankets, or rolled towels to elevate the area as often as you can.
- Do not let your child stretch injured muscles right after the injury. Ask your child's healthcare provider when and how your child may safely stretch after the injury. Gentle stretches can help increase your child's flexibility.
- Do not massage the area or put heating pads on the bruise right after the injury. Heat and massage may slow healing. Your child's healthcare provider may tell you to apply heat after several days. At that time, heat will start to help the injury heal.
 |
How can a contusion be prevented?
- Do not leave your baby alone on the bed or couch. Watch him or her closely as he or she starts to crawl, learns to walk, and plays.
- Make sure your child wears proper protective gear. These include padding and protective gear such as shin guards. He or she should wear these when he or she plays sports. Teach your child about safe equipment and places to play, and teach him or her to follow safety rules.
- Remove or cover sharp objects in your home. As a very young child learns to walk, he or she is more likely to get injured on corners of furniture. Remove these items, or place soft pads over sharp edges and hard items in your home.
When should I seek immediate care?
- Your child cannot feel or move his or her injured arm or leg.
- Your child begins to complain of pressure or a tight feeling in his or her injured muscle.
- Your child suddenly has more pain when he or she moves the injured area.
- Your child has severe pain in the area of the bruise.
- Your child's hand or foot below the bruise gets cold or turns pale.
When should I call my child's doctor?
- The injured area is red and warm to the touch.
- Your child's symptoms do not improve after 4 to 5 days of treatment.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Contusion
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
