Compartment Syndrome in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is compartment syndrome?
Compartment syndrome is a condition that causes muscle and nerve damage. Swelling or bleeding increases pressure in and between muscles. This stops blood from flowing to the area. Compartment syndrome usually happens in an arm or leg. Symptoms start suddenly and get worse quickly. Without immediate treatment, damage may become severe and permanent.
What increases my child's risk for compartment syndrome?
- Direct pressure, such as from a bandage or cast that is too tight
- An injury that causes swelling or bleeding, such as broken bones, burns, allergic reactions, or insect bites
- Certain medicines that increase your child's risk for bleeding or pressure buildup
- Medicines or IV drugs that are injected into the veins
- Surgery that caused your child's leg to be placed above the level of his or her heart for a long period of time
What are the signs and symptoms of compartment syndrome?
- Severe pain that seems worse than you would expect for the injury, or that does not get better with pain medicine
- Pain that increases when your child rests the area or stretches or bends the area
- Swelling, tightness, or hardness of the skin in the area that was injured
- Pale or shiny skin near your child's injury
- Numb skin or weak muscles in the area, or trouble moving the injured arm or leg
How is compartment syndrome diagnosed and treated?
Your child's healthcare provider will examine the area where your child is having pain. The provider may also measure the pressure in this area. Your child may need to have a cast loosened or removed. This will help decrease pressure in the muscles. Your child may also need any of the following:
- Pain medicine may be given. You may need a doctor's order for this medicine. Do not wait until the pain is severe before you give your child the medicine.
- Surgery may be needed to decrease pain, pressure, and swelling.
- Hyperbaric oxygen therapy is used to get more oxygen into your child's body. It is done after surgery to decrease pressure. The oxygen is given under pressure to help it get into the tissues and blood. Your child may need to have this therapy more than 1 time.
What can I do to help my child prevent compartment syndrome?
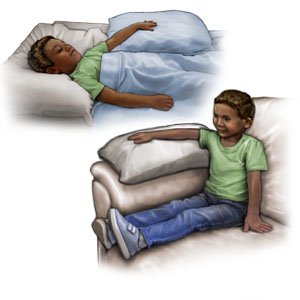
- Elevate your child's arm or leg after an injury. Raise your child's arm or leg at the level of his or her heart as long as directed. This will help decrease swelling and pain. Do not raise the arm or leg higher than your child's heart. Prop it on pillows or blankets to keep it elevated.

- Check for proper fit. Make sure a brace or bandage your child gets after an injury is not too tight. You should be able to fit 2 fingers between your child's skin and the brace or bandage.
When should I seek immediate care?
- Your child has increased pain that does not go away or gets worse, even after he or she takes medicine.
- Your child tells you that the injured arm or leg feels numb.
- Your child's injured arm or leg turns blue or white or feels cold.
- Blood soaks through your child's bandage or cast.
- Your child's wound drains pus or smells bad.
When should I call my child's doctor?
- Your child has a fever.
- Your child's skin is itchy, swollen, or has a rash.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
