Colposcopy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about a colposcopy:
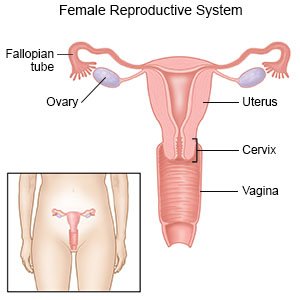
A colposcopy is a procedure to look at your cervix and inside your vagina. You may need a colposcopy if abnormal cells are found on a Pap smear or you were treated for cervical or vaginal problems. Abnormal bleeding, pelvic pain, or genital warts are also reasons for a colposcopy.
 |
How to prepare for a colposcopy:
- Your healthcare provider will talk to you about how to prepare for your procedure. You may need to arrange to have someone drive you home after the procedure.
- Do not douche, use tampons, or have sex for 24 hours before the procedure. Do not put medicines in your vagina for 24 hours before the procedure.
- Call your healthcare provider if you have your menstrual period on the day of the procedure. You may need to wait until your period ends to have the procedure.
- Your healthcare provider may tell you take ibuprofen before your procedure to decrease cramping.
What will happen during a colposcopy:
- Your healthcare provider will insert a speculum in your vagina. A speculum is an instrument that holds the vagina open so your provider can see your cervix. The provider will place a colposcope near the opening to your vagina. A colposcope has a magnifying lens that helps your provider see your cervix better. The provider will apply a liquid to your cervix. The liquid helps your provider see abnormal areas more clearly. You may feel burning or tingling when the liquid is applied.
- If abnormal areas are seen, your healthcare provider may place a numbing medicine on your cervix. He or she will take a biopsy (samples) of tissue from your cervix. The samples can be sent to a lab and tested for cancer or infection. You may feel pain or cramping when the sample is taken. Your healthcare provider may place medicine on your cervix to control bleeding.
What to expect after a colposcopy:
- You may have cramps and light bleeding or spotting after the procedure. These usually only last a few hours.
- You may have cramps and bleeding for several days if samples were taken. You may have brown or black discharge if medicine was used to control bleeding.
- Your healthcare provider will tell you when to come in for a follow-up visit. This is usually 1 to 3 weeks after the procedure. You may also get results of a biopsy during that visit.
Risks of a colposcopy:
You may bleed more than expected or get an infection. A biopsy of your cervix may cause problems with future pregnancies, such as preterm labor or miscarriage.
Seek care immediately if:
- You have severe pain in your lower abdomen.
- You soak through 1 sanitary pad in 1 hour or less.
- You feel weak, dizzy, or faint.
Call your doctor or gynecologist if:
- You have a fever, chills, or foul-smelling discharge.
- You have bleeding with clots.
- Your pain gets worse or does not get better after you take pain medicine.
- You have questions or concerns about your condition or care.
Medicines:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
If tissue samples were not taken, you can go back to your usual activities. Your healthcare provider will give you specific directions if samples were taken. The following are general guidelines:
- Rest for 24 hours, or as directed. Do not exercise, play sports, or lift anything heavier than 5 pounds. Ask your provider when you can return to your usual activities.
- Do not put anything in your vagina for 2 weeks, or as directed. Do not douche, use medicines in your vagina, or have sex. Do not use tampons. Wear sanitary pads for bleeding. Your provider will tell you when it is okay to do these again.
- Do not smoke. Smoking increases your risk for cervical cancer. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Follow up with your doctor or gynecologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
