Colorectal Cancer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
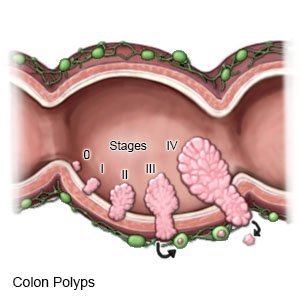
Colorectal cancer starts in the large intestine (colon) or rectum. The cancer may begin as a small polyp (lump of tissue) that grows inside your intestine.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You vomit multiple times and cannot keep any food or liquids down.
- You see blood in your bowel movements.
Call your doctor or oncologist if:
- You have a fever.
- You cannot control your diarrhea or constipation.
- Your pain is worse or does not go away after you take your pain medicine.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Antinausea medicine may be given to calm your stomach and prevent vomiting.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Get screened as directed:
Screening means you are checked for colorectal cancer, even if you do not have signs or symptoms. Screening is recommended starting at age 50 and continuing to age 75 if you are at average risk. Your healthcare provider may suggest screening starting at age 45. Screening may start before you are 45 or continue after you are 75 if your risk is high. Your provider will tell you how often to get screened. Timing depends on the type of screening and if polyps or other problems were found. Timing also depends on your age and if you are at increased risk for cancer. Screening may be recommended every 1, 2, 5, or 10 years.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Do not smoke:
Nicotine can damage blood vessels and make it hard to manage colorectal cancer. Smoking also increases your risk for new or returning cancer and delays healing after treatment. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your healthcare provider for information if you currently smoke and need help quitting.
Eat healthy foods:
Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. You may need to change what you eat during treatment. Do not eat foods or drink liquids that cause gas, such as cabbage, beans, onions, or soda. A dietitian may help to plan the best meals and snacks for you.
 |
Limit or do not drink alcohol as directed:
Men should limit alcohol to 2 drinks per day. Women should limit alcohol to 1 drink per day. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
Drink liquids as directed:
Ask how much liquid to drink each day and which liquids are best for you. If you have nausea or diarrhea from cancer treatment, extra liquids may help decrease your risk for dehydration.
Be physically active as directed:
Ask about the best exercise plan for you. Physical activity, such as exercise, may improve your energy levels and appetite.
 |
Follow up with your doctor or oncologist as directed:
You will need to see your oncologist for ongoing treatment and follow-up. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Colorectal Cancer
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
