Arthroscopic ACL Reconstruction
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about arthroscopic anterior cruciate ligament (ACL) reconstruction:
ACL reconstruction is surgery to replace your torn ACL. The ACL is a ligament in your knee that connects the tibia (shin bone) to the femur (thigh bone). Ligaments are strong tissues that connect bones.
How to prepare for surgery:
- Your surgeon will tell you how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight before your surgery. Arrange to have someone drive you home after surgery.
- Tell your surgeon about all your current medicines. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon if you have any allergies, including to anesthesia or medicines.
What will happen during surgery:
- You may get regional anesthesia that will make you lose feeling in your leg. You may get general anesthesia to keep you asleep and free from pain during surgery. A small incision will be made in your knee.
- Your surgeon will use an arthroscope to look inside your knee joint by inserting it through the incision. More small incisions will be made in several places around your knee. Tools will be put into these incisions to reconstruct your injured ACL. Another incision will be made if the graft (piece of tendon or muscle) will be taken from another part of your body. The graft will be pulled through a tunnel drilled in your tibia and femur. Screws will be used to hold it in place.
- The incisions will be closed with stitches, staples, or medical tape. A drain may be placed temporarily to remove fluid from the surgery area.
What to expect after surgery:
You will be taken to a room to rest until you are fully awake. Healthcare providers will watch you closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You will then be taken to your room or allowed to go home.
- You may need to walk around the same day of surgery , or the day after. Movement will help prevent blood clots. You may also be given exercises to do in bed. Talk to healthcare providers before you get up the first time. They may need to help you stand up safely. When you are able to get up on your own, sit or lie down right away if you feel weak or dizzy. Then press the call light button to ask for help.
- An electrical muscle stimulator (EMS) may be used to decrease your pain after surgery. Sticky pads are put on the skin around your knee. Electrical impulses go into one pad and energy comes out the other. This treatment may last 15 to 20 minutes one or more times a day. EMS makes your muscles contract. This helps your muscles heal and get stronger.
- Medicines may be given to prevent or fight a bacterial infection. You may also get medicine to prevent nausea or to reduce pain, swelling, or fever.
- Physical therapy (PT) is used to help you improve movement and strength, and to decrease pain. You may begin PT while you are in the hospital and continue for several weeks after you get home.
Risks of ACL reconstruction:
You may develop an infection or bleed more than expected. You could have trouble breathing or develop blood clots. Even after surgery, the knee may not go back to the way it was before.
Call your local emergency number (911 in the US) if:
- You have sudden shortness of breath or chest pain.
Seek care immediately if:
- Blood soaks through your bandage.
- Your stitches come apart.
- You fall on your knee.
- You have pain in your lower leg and swelling or a red area near the pain.
- Your leg or toes feel numb, tingly, cool to the touch, or look blue or pale.
Call your doctor or surgeon if:
- You have a fever.
- You have severe pain in your knee or trouble moving around, even after you take your pain medicines.
- Your wound is swollen, red, or draining pus.
- Your skin is itchy, swollen, or has a rash.
- You have questions or concerns about your condition or care.
Medicines:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Self-care:
- Elevate your knee. Keep your knee raised above the level of your heart as often as you can. This will help decrease or limit swelling. Elevate your knee by resting it on pillows.

- Apply ice. Ice helps decrease swelling and pain. Ice may also help prevent tissue damage. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel and place it on your wound for 15 to 20 minutes every hour. Use the ice for as long as directed.
- Rest your knee as directed. Your healthcare provider will tell you when you can return to your normal activities.
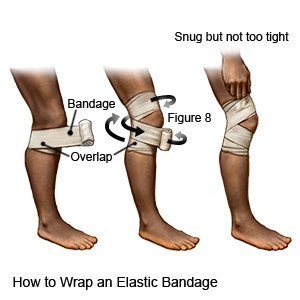
- Apply compression. Ask your healthcare provider if you should wrap an elastic bandage around your injured ligament. Compression provides support and helps decrease swelling and movement so your joint can heal. Do not wrap the bandage tightly. It should be snug, but you should be able to slip a finger between the bandage and your skin.
- Physical therapy is used to help you improve movement and strength, and to decrease pain.
- A continuous passive motion (CPM) machine is a device that slowly and gently moves your joint while you are in bed. The machine can increase your range of motion, strengthen your muscles, and decrease pain. Your healthcare provider may tell you use a CPM machine with other treatments, such as physical therapy.
Use support devices as directed:
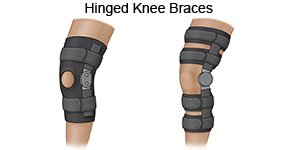
- A knee brace may be used to limit your movement and protect your knee. Your healthcare provider will tell you when you can unlock the brace. Keep it locked at all other times. Ask your healthcare provider for more information about your knee brace.
- Crutches may help decrease your pain as you move around. Crutches help decrease strain on your knee. Use crutches as directed.
Wound care:
- Keep your bandage and stitches clean and dry. Do not remove the bandage over the surgery area or get it wet unless your healthcare provider says it is okay. Ask when you can bathe. Do not trim or shorten the ends of your stitches. If the stitches rub against your clothing, you can put a soft gauze bandage between the stitches and your clothes. Strips of medical tape that were placed over the incision will start to peel off on their own. If they have not fallen off within 14 days, you can carefully peel them off.
- Wash your hands. Always wash your hands before and after you care for your wound to prevent infection.

- Change your bandage and clean the surgery area as directed. Ask for help if you cannot reach the area. Do not put powders or lotions on the area. Check the area every day for signs of infection such as redness, swelling, or pus.
Follow up with your doctor or surgeon as directed:
You may need to return to have your stitches removed. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
