Acute Low Back Pain
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is acute low back pain?
Acute low back pain is sudden discomfort that lasts up to 6 weeks and makes activity difficult.
What causes or increases my risk for acute low back pain?
Conditions that affect the spine, joints, or muscles can cause back pain. These may include arthritis, spinal stenosis (narrowing of the spinal column), muscle tension, or breakdown of the spinal discs. The following increase your risk for back pain:
- Repeated bending, lifting, or twisting, or lifting heavy items
- Injury from a fall or accident
- Lack of regular physical activity
- Obesity or pregnancy
- Smoking
- Aging
- Driving, sitting, or standing for long periods
- Bad posture while sitting or standing
How is the cause of acute low back pain diagnosed?
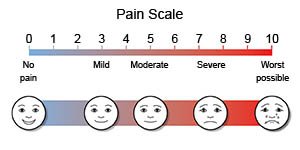
Your healthcare provider will ask about your medical history and examine you. He or she may ask when you last had low back pain and how it started. Show him or her where you feel the pain and what makes it better or worse. Tell your provider about the type of pain you have, how bad it is, and how long it lasts. Tell him or her if your pain worsens at night or when you lie on your back.
 |
How is acute low back pain treated?
The goal of treatment is to relieve your pain and help you be able to do your regular activities. Most people with acute low back pain get better within 4 to 6 weeks. You may need any of the following:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Muscle relaxers decrease pain by relaxing the muscles in your lower spine.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
What can I do to prevent low back pain?
- Use proper body mechanics.
- Bend at the hips and knees when you pick up objects. Do not bend from the waist. Use your leg muscles as you lift the load. Do not use your back. Keep the object close to your chest as you lift it. Try not to twist or lift anything above your waist.

- Change your position often when you stand for long periods of time. Rest one foot on a small box or footrest, and then switch to the other foot often.
- Try not to sit for long periods of time. When you do, sit in a straight-backed chair with your feet flat on the floor. Never reach, pull, or push while you are sitting.
- Bend at the hips and knees when you pick up objects. Do not bend from the waist. Use your leg muscles as you lift the load. Do not use your back. Keep the object close to your chest as you lift it. Try not to twist or lift anything above your waist.
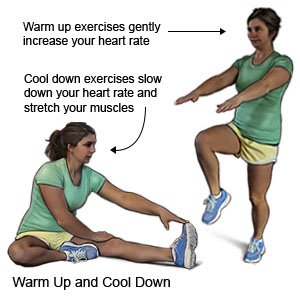
- Do exercises that strengthen your back muscles. Warm up before you exercise. Ask your healthcare provider for the best exercises for you.
- Maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Ask him or her to help you create a weight loss plan if you are overweight.
How can I take care of myself if I have acute low back pain?
- Stay active as much as you can without causing more pain. Bed rest could make your back pain worse. Start with some light exercises, such as walking. Avoid heavy lifting until your pain is gone. Ask for more information about the activities or exercises that are right for you.

- Apply heat on your back for 20 to 30 minutes every 2 hours for as many days as directed. Heat helps decrease pain and muscle spasms. Alternate heat and ice.
- Apply ice on your back for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it to your skin. Ice helps prevent tissue damage and decreases swelling and pain.
When should I seek immediate care?
- You have severe pain.
- You have sudden stiffness and heaviness down both legs.
- You have numbness or weakness in one leg, or pain in both legs.
- You have numbness in your genital area or across your lower back.
- You cannot control your urine or bowel movements.
When should I call my doctor?
- You have a fever.
- You have pain at night or when you rest.
- Your pain does not get better with treatment.
- You have pain that worsens when you cough or sneeze.
- You suddenly feel something pop or snap in your back.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Acute Low Back Pain
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
