A-Fib (Atrial Fibrillation)
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Atrial fibrillation (A-fib) is an irregular heartbeat. It reduces your heart's ability to pump blood through your body. A-fib may come and go, or it may be a long-term condition. A-fib can cause blood clots, stroke, or heart failure. These conditions may become life-threatening. It is important to treat and manage A-fib to help prevent a blood clot, stroke, or heart failure.
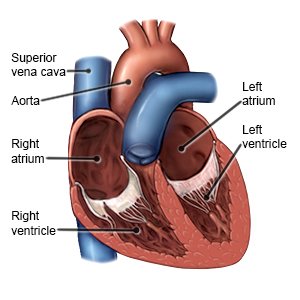 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
Seek immediate care if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Your heart rate is more than 110 beats per minute.
- You are short of breath, even at rest.
Call your doctor or cardiologist if:
- You have new or worsening swelling in your legs, feet, ankles, or abdomen.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Heart medicines help control your heart rate or rhythm. You may need more than 1 medicine to treat your symptoms.
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Antiplatelets , such as aspirin, help prevent blood clots. Take your antiplatelet medicine exactly as directed. These medicines make it more likely for you to bleed or bruise. If you are told to take aspirin, do not take acetaminophen or ibuprofen instead.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Manage or prevent A-fib:
- Get screening for A-fib, if recommended. Screening means you are checked for A-fib, even if you do not have signs or symptoms. Screening can find problems early so treatment can begin. Early treatment can save your life. Your healthcare provider will talk to you about the benefits and risks of screening. Screening may be recommended starting at age 50. Your provider may recommend regular screenings if you stay at high risk for A-fib.
- Know your target heart rate. Learn how to check your pulse and monitor your heart rate.
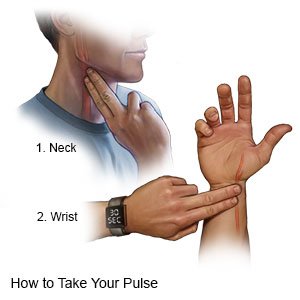
- Know the risks if you choose to drink alcohol. Alcohol can increase your risk for A-fib or make A-fib harder to manage. Ask your provider if it is okay for you to drink any alcohol. Your provider can help you set limits for the number of drinks you have in 24 hours and in a week. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Do not smoke. Nicotine can cause heart damage and make it more difficult to manage your A-fib. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your provider for information if you currently smoke and need help quitting.
- Eat heart-healthy foods. Heart healthy foods will help keep your cholesterol low. These include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Replace butter and margarine with heart-healthy oils such as olive oil and canola oil.

- Maintain a healthy weight. Ask your provider what a healthy weight is for you. Your provider can help you create a safe weight loss plan, if needed. Even a small goal of a 10% weight loss can improve your heart health.
- Get regular physical activity. Physical activity helps improve your heart health. Get at least 150 minutes of moderate aerobic physical activity each week. Your provider can help you create an activity plan.

- Manage other health conditions. This includes high blood pressure or cholesterol, sleep apnea, diabetes, and other heart conditions. Take medicine as directed and follow your treatment plan. Your provider may need to change a medicine you are taking if it is causing your A-fib. Do not stop taking any medicine unless directed by your provider.
Follow up with your doctor or cardiologist as directed:
You will need regular blood tests and monitoring. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about A-Fib
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
