Premature Atrial Contractions
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What are premature atrial contractions (PACs)?
PACs are an interruption in your heart rhythm. PACs happen when your heart gets an early signal to pump. PACs are common and usually have no cause. Most people have skipped heartbeats from time to time. Follow up with your healthcare provider so the cause of your PAC can be diagnosed and treated.
What increases my risk for PACs?
- Stress or fatigue
- Caffeine, alcohol, or tobacco
- Medical conditions, such as high blood pressure, heart disease, or hyperthyroidism
- Pregnancy
What are the signs and symptoms of PACs?
- Palpitations (fast, forceful heartbeats in an irregular rhythm)
- A missed or skipped heartbeat
- Chest pain or shortness of breath
- Lightheadedness, dizziness, or feeling faint
- Tiredness with exercise or activity
How are PACs diagnosed?
Your healthcare provider will ask if you have a family history of heart problems. You may also need any of the following:
- An EKG records your heart rhythm and how fast your heart beats. It is used to check for PACs.
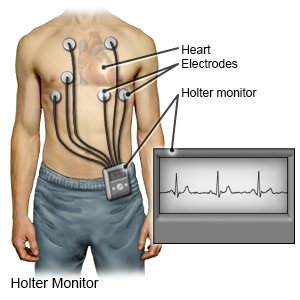
- A Holter monitor is a device that you wear for a period of time. It records how fast your heart beats, and if it beats in a regular pattern. You may need to wear it up to 72 hours. This will show how frequent your PACs are during your normal daily activities.
How are PACs treated?
PACs usually do not need treatment. You may be given medicine to strengthen or regulate your heartbeat.
How can I help prevent more PACs?
- Do not have alcohol or caffeine. These can increase your PACs.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase heart problems. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Exercise as directed. Exercise helps keep your heart healthy. Ask your healthcare provider about the best exercise plan for you.
Call 911 for any of the following:
You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
When should I contact my healthcare provider?
- Your symptoms do not go away, or they get worse.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Premature Atrial Contractions
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
