Postpartum Thyroiditis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is postpartum thyroiditis?
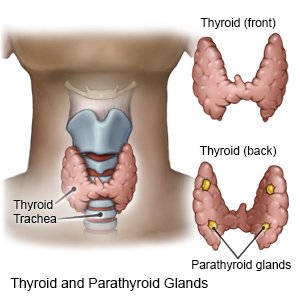
Postpartum thyroiditis is a disease that causes your thyroid gland to become inflamed after you give birth. The thyroid gland is located at the front of your neck. The thyroid produces hormones that help control your body functions, such as temperature and heart rate. Postpartum thyroiditis can develop right after or within a year after delivery.
 |
What causes postpartum thyroiditis?
Postpartum thyroiditis is an autoimmune disease. This means that your body's immune system attacks your thyroid gland. During pregnancy, the immune system slows down. After delivery, the immune system starts to work normally again. During this time, your immune system may attack and damage your thyroid gland.
What increases my risk for postpartum thyroiditis?
- Tobacco use
- Miscarriage or abortion
- Thyroid problems during past pregnancies
- Family history of thyroid disease
- High levels of thyroid antibodies during the first months of pregnancy
- Insulin-dependent diabetes mellitus
What are the signs and symptoms of postpartum thyroiditis?
- Early signs and symptoms:
- Being hot and sweaty
- Feeling nervous, tense, or restless
- A fast heartbeat
- An enlarged thyroid gland
- Tremors
- Weight loss without trying, and always feeling hungry
- Late signs and symptoms:
- Feeling cold
- A slow heartbeat
- Weakness and muscle pain
- Weight gain
- Constipation
- Dry or flaky skin, and thin and brittle fingernails or hair
- Swelling around the eyes
- A change in your voice or speech
How is postpartum thyroiditis diagnosed?
- Blood tests may show if your thyroid hormone level is too high or too low.
- A thyroid scan will show how well your thyroid gland is working. Dye is put into your IV or given as a liquid to drink. The part of your thyroid gland that works normally will soak up the dye. Healthcare providers put a machine over your neck 2 to 48 hours later. The machine takes pictures that show the areas of your thyroid that work properly. Tell the healthcare provider if you have ever had an allergic reaction to contrast dye.
How is postpartum thyroiditis treated?
Postpartum thyroiditis usually goes away on its own. Healthcare providers may watch you for changes over time. You may need any of the following:
- Medicines may be given to help raise or lower your thyroid hormone level. You may also need medicines to treat your signs and symptoms, such as fast heartbeat and nervousness.
- Radioactive iodine may be given to damage or kill some of your thyroid gland cells. This may decrease the amount of thyroid hormone produced. Tell the provider if you know or think you are pregnant. Radioactive iodine may be harmful to an unborn baby.
How can I manage my symptoms?
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. This will help you maintain a healthy weight. Ask if you need to be on a special diet.

- Drink liquids as directed. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you.
- Exercise as directed. Ask your healthcare provider about the best exercise plan for you. Start slowly and do more as you get stronger. Exercise can help give you energy and decrease your symptoms.

Call your local emergency number (911 in the US) or have someone call if:
- You have sudden chest pain or trouble breathing.
- You have a seizure.
When should I seek immediate care?
- Your heart is racing.
- You feel like you are going to faint.
When should I call my doctor?
- You have a fever.
- You run out of thyroid medicine before your next scheduled refill.
- You feel nervous and restless.
- You have pain or swelling in your muscles.
- Your voice becomes hoarse, or you have itchiness in your throat.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Postpartum Thyroiditis
Treatment options
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
