Optic Neuritis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is optic neuritis?
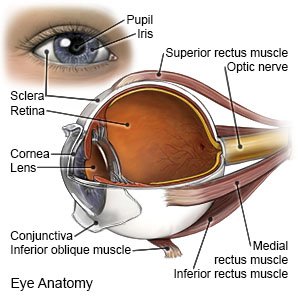
Optic neuritis is inflammation of the optic nerve. The optic nerve helps you see by sending an image from the eye to the brain. Inflammation of the nerve leads to vision loss. Usually only one eye is affected, but you may have optic neuritis in both eyes.
 |
What causes or increases my risk for optic neuritis?
- Demyelination (loss of protective covering) of the optic nerve
- An infection, such as hepatitis or tuberculosis (TB)
- An autoimmune disease such as multiple sclerosis (MS)
- An inflammatory disease such as lupus or certain eye infections
- Exposure to a chemical such as lead
- A tumor, or damage in an artery or vein that affects the optic nerve
- Certain medicines, such as some antibiotics and medicines used to treat malaria or TB
- A lack of vitamin B12
What are the signs and symptoms of optic neuritis?
Vision loss can start within hours or days. The loss will be worst at 1 week. You may also have any of the following:
- Loss of vision, or trouble with depth perception (seeing how far away an object is)
- Seeing lights as dim or less bright than usual, or trouble seeing in direct sunlight
- Tenderness around your eye that is worse when you move your eye
- A blurry spot or quick flashes of light
- Trouble seeing color, especially red
- Blurred or foggy vision
- A headache (more common in children)
- Signs and symptoms that happen only when you exercise or are hot
How is optic neuritis diagnosed?
Your healthcare provider will ask about your symptoms and when they began. Your provider will check how your nervous system is working, and examine your overall health. You may also need any of the following:
- Blood tests may be used to check for certain antibodies. Antibodies are part of your immune system. These antibodies may be attacking your optic nerve.
- An eye exam will show how well you see shapes and colors. Your provider will use an instrument such as an ophthalmoscope to see into the back of your eye. Your provider may also shine a flashlight to see how your pupils react to light.
- MRI pictures may show problems with your optic nerve or other parts of your eye and brain. You may be given contrast liquid to help your eye show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious damage. Tell the healthcare provider if you have any metal in or on your body.
- A visual evoked response test is used to show your brain's reaction to what you see. You will look at a screen that shows different patterns. Your brainwaves are measured through wires attached to patches that are placed on your head.
How is optic neuritis treated?
Optic neuritis may go away on its own without treatment within a few months. It may take a year before your vision returns to normal or near normal. Even with treatment, your vision may not return completely to normal. If you have severe vision loss, steroid medicine may be used to reduce inflammation. The medicine may be given through an IV to help your vision clear more quickly. This may be done if you only have vision in 1 eye or you need to see clearly for work.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When should I seek immediate care?
- You have vision loss in both eyes along with a headache or double vision.
When should I contact my healthcare provider?
- You have new or worsening symptoms.
- Your symptoms do not improve within 1 to 2 weeks.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Optic Neuritis
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
