Male Condom Use
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about condoms?
A condom can help prevent pregnancy and sexually transmitted infections (STIs).
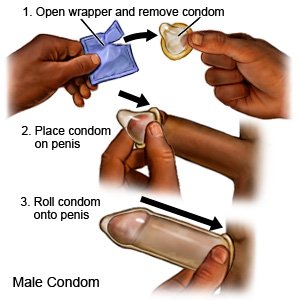
How do I put on a condom?
- Place the rolled condom over the tip of your erect penis. If you are not circumcised, pull back your foreskin before you put the condom on. You may choose to put 1 or 2 drops of water-based lubricant inside the rolled condom before you put it on.
- Leave ½ inch space at the tip to collect semen. Use your forefinger and thumb to pinch the tip of the condom to remove extra air. Trapped air may cause the condom to burst.
- Unroll the condom onto your penis.
- Roll it all the way down to the base of your penis. If the condom does not reach the base of your penis, remove it. The condom may be too small or inside out. Throw it away and use a new condom.
- Smooth out any air bubbles.
- Lubricate the outside of the condom, if needed. If you use lubricant, it must be water-based. Do not use petroleum jelly, cooking oil, mineral oil, lotion, or saliva. These may damage the condom. If it is used for anal sex, use extra lubricant to prevent the condom from breaking.
- Check the condom during sex. If your condom rolls up during sex, roll it back down. If it slips off, replace it with a new condom.
 |
How do I remove a used condom?
- Remove your condom before your penis softens. Hold the condom against the base of your penis while you slide it off so you do not spill the semen. Do not pull it from the tip or roll it off.
- Throw away your used condom in a trash container. Do not flush it down the toilet.
What else do I need to know about condoms?
- Latex condoms should be used, if possible. Lambskin (also called sheepskin or natural membrane) condoms do not protect against STIs. Use a polyurethane condom if you or your partner has a latex allergy.
- You or your partner may need medical care if the condom breaks, leaks, or slips. Your female partner can use emergency contraception to decrease the risk of a possible pregnancy. It should be taken as soon as possible after a condom accident. Ask your healthcare provider for more information about emergency contraception. Ask him or her to test you for STIs if you are concerned about an infection.
- Use a condom with a second form of protection. The best way to protect you and your partner is to use a condom with a sponge, cervical cap, or spermicide. Do not use a condom while your partner uses a female condom. The 2 condoms may stick together and slip out of place. Ask your healthcare provider for information about other methods of birth control.
- Use a new condom every time you have sex. Do not use condoms past the expiration date. Make sure the package is sealed and in good shape. Open the package carefully.
- Store condoms in a cool, dry place. Heat may damage the condom. Check the expiration date. Do not use the condom if it is past the expiration date.
When should I call my doctor?
- You have sudden itching, redness, or swelling on your penis.
- A condom breaks or slips off after ejaculation.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
