Iritis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is iritis?
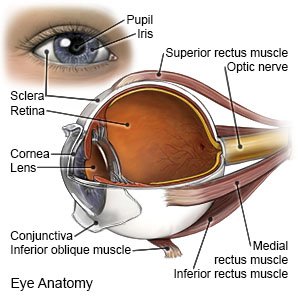
Iritis is inflammation of your iris. The iris is the colored part of your eye. Viruses, bacteria, and fungi are common causes of iritis. An eye injury or certain medicines may cause inflammation. You may develop iritis if you have an autoimmune disease, such as inflammatory bowel disease or psoriatic arthritis.
 |
What are the signs and symptoms of iritis?
- Pain that may be deep in your eye or on the surface
- Red or watery eye
- Blurred vision, or vision problems
- Sensitivity to light
How is iritis diagnosed?
Your healthcare provider will ask about your symptoms and when they started. You may also need any of the following tests:
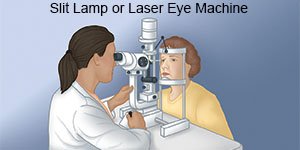
- A slit-lamp exam helps your healthcare provider have a better view of the inside of your eye. Your provider will shine a bright light in your eye to check for inflammation. You may need eyedrops to dilate your pupils.
- Tonometry is a test that measures your eye pressure. Your eyes will be numbed with eyedrops. Then your healthcare provider will touch your eyes with an instrument. A puff of air may be blown into your eyes. The pressure is measured with a light.
How is iritis treated?
Iritis may go away on its own. If it continues, you may need any of the following:
- Cycloplegic eyedrops dilate your pupil and relax your eye muscles. This helps decrease pain and light sensitivity.
- Steroid eyedrops help decrease pain and inflammation. These are only used for a short time to relieve the inflammation. You may be given steroid medicine as pills if the cause of your iritis is not an infection.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage iritis?
- Apply a warm compress to your eye. Wet a washcloth in warm water and wring it out. Place it gently over your eye for 20 minutes 3 to 4 times each day. This will help soothe your eye and decrease inflammation.
- Wear dark sunglasses. This will help prevent pain and light sensitivity. Make sure the sunglasses have UVA and UVB protection. This will protect your eyes when you go outside.
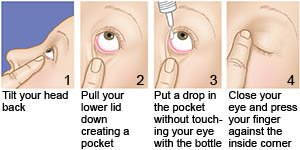
- Use eyedrops safely. If your treatment plan includes eyedrops, it is important to use them as directed. Your provider may give you detailed instructions to follow. The eyedrops may also come with safety instructions. Follow all instructions to help prevent an infection. Do not touch the tip of the bottle to your eye. Germs from your eye can spread to the medicine bottle.
When should I call my doctor or ophthalmologist?
- You have severe eye pain and a headache.
- Your vision suddenly gets worse.
- You have nausea or are vomiting.
- Your pain gets worse, even after treatment.
- You see halos or rainbows around lights.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Iritis
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
