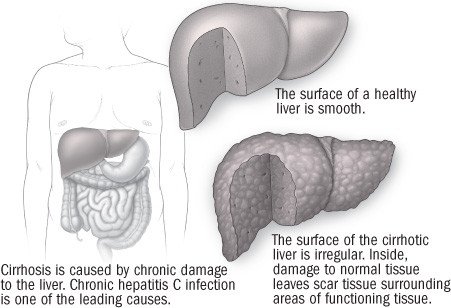
Cirrhosis
Medically reviewed by Drugs.com. Last updated on Jul 15, 2025.
What is cirrhosis?

No body organ performs a wider variety of essential jobs than the liver. It:
- Produces essential proteins that help blood to clot
- Removes or neutralizes poisons, drugs and alcohol
- Manufactures bile that helps the body to absorb fats and cholesterol
- Helps to maintain normal blood sugar levels
- Regulates several hormones.
Cirrhosis is a disease in which normal liver cells are replaced by scar tissue, which interferes with all of these important functions. In extreme cases, the damage is so severe that the only solution is a liver transplant.
|
|
Cirrhosis has many causes. In the United States and Europe, the most common causes are excessive alcohol use and chronic infection with the hepatitis C virus.
Alcohol has a toxic effect on liver cells. Alcoholic cirrhosis tends to develop after a decade or more of heavy drinking, although it is possible for "social drinkers" to have cirrhosis. It is not known why some people are more prone to adverse reactions than others, but women are at greater risk of cirrhosis, even when they drink less alcohol than men.
Chronic hepatitis B, which causes damage in a similar way, is another common cause of cirrhosis in the world. But it is less common in industrialized countries because of routine vaccination against hepatitis B.Chronic hepatitis C causes inflammation of the liver that eventually can lead to cirrhosis. Without treatment, about one out of every five people with chronic hepatitis C develops cirrhosis after 20 years.
More recently, non-alcoholic fatty liver disease has become a more common cause of cirrhosis. Doctors call it nonalcoholic steatohepatitis (NASH). Fat deposition in the liver leads to inflammation, which can progress to scarring.
Rarer causes of cirrhosis include:
- Autoimmune diseases that attack the bile ducts or liver cells
- Severe reactions to prescription drugs
- Prolonged exposure to environmental toxins
- Infections from bacteria and parasites usually found in the tropics or Asia
- Repeated episodes of heart failure with liver congestion
- Certain inherited diseases, including:
- Hemochromatosis, in which too much iron builds up in the liver and other organs
- Wilson's disease, which produces abnormal concentrations of copper
- Alpha-1-antitrypsin deficiency, which is the absence of a particular enzyme in the liver.
Symptoms of cirrhosis
In its early stages, cirrhosis often has no symptoms. But as liver cells die, the organ makes less of the proteins that regulate fluid retention and blood clotting and loses its ability to metabolize the pigment bilirubin. This causes symptoms and complications that include:
- Fatigue
- Loss of appetite
- Nausea
- Weakness
- Weight loss
- Fluid accumulation in the legs (edema) and abdomen (ascites)
- Increased bleeding and bruising
- Jaundice, a yellowing of the skin and eyes
- Itching
- Confusion.
As damage increases, the liver fails to detoxify the blood and becomes less able to metabolize many medications, which magnifies their effects. Eventually, toxins build up in the brain. These changes can produce:
- Increased sensitivity to drugs
- Personality and behavioral changes, including confusion, neglect of appearance, forgetfulness, trouble concentrating and changes in sleep habits
- Loss of consciousness
- Coma.
Scarring also impedes blood flow and increases pressure in the portal vein, which moves blood from the stomach to the liver. This condition is called portal hypertension. Blood vessels in the stomach and esophagus swell, and the body creates new ones in an attempt to bypass the liver. These vessels, called varices, have thin walls. If one bursts, the resulting hemorrhage (major bleeding) can cause death within hours if not treated.
Diagnosing cirrhosis
Your doctor will ask about your medical history, family history of liver disease, diet, alcohol consumption, medications you are taking, and risk factors for hepatitis B and C, such as intravenous drug use. During a physical examination, the doctor determines whether the liver feels harder or larger than normal, looks for skin changes such as bruising and jaundice, and looks for evidence of fluid swelling in the legs or abdomen.
Blood tests may be ordered to look for evidence of liver inflammation, an elevated bilirubin level, a buildup of toxins (such as ammonia) and reduced levels of essential substances made by the liver.
Two of the blood tests that indicate a poor prognosis in people with cirrhosis are a low albumin level and a high INR (adjusted Pro-Time). The high INR indicates the person's liver cannot make the normal amount of clotting proteins.
The liver may be viewed using ultrasound or a computerized tomography (CT) scan, or other imaging technique.
Cirrhosis can usually be diagnosed based on the history, physical exam, blood test results and imaging. Sometimes a liver biopsy is needed. A tiny sample of liver tissue is removed through a needle and then examined for scarring and damage to cells.
Expected duration of cirrhosis
Cirrhosis is usually a progressive disease. Although it usually cannot be reversed, the liver damage can be halted or slowed down with treatment or changes in behavior in many cases.
Preventing cirrhosis
The most important step you can take to prevent cirrhosis is to avoid excessive drinking. It is best to consume an average of no more than two alcoholic drinks a day for men or one drink a day for women. If you have chronic hepatitis or other liver problems, avoid alcohol completely.
Some other causes of cirrhosis can be prevented. To avoid infection with hepatitis B and C, do not inject illegal drugs, snort cocaine, or have unprotected sex, especially with multiple partners. If you are considering body piercing or tattooing, make sure that the equipment is cleaned properly. Health care and emergency workers should follow infection control precautions carefully whenever they are exposed to blood.
Hepatitis B also can be prevented with a vaccine, a series of three shots that is 90% effective.
By preventing nonalcoholic fatty liver disease, you prevent the small risk of developing cirrhosis. This means maintaining a healthy weight and getting plenty of exercise.
Treating cirrhosis
Treatment for cirrhosis varies depending on the cause and stage of the disease. Because liver damage usually cannot be reversed, the aim of all treatment is to keep the disease from getting worse and to reduce complications.
Regardless of the cause, anyone with cirrhosis should abstain from alcohol and use caution in taking medications that can make liver disease worse, including over-the-counter acetaminophen (Tylenol and generic types). You also will be treated for underlying diseases -- for example, antiviral medications for chronic hepatitis B or C, corticosteroids or other immunosuppressant medications for autoimmune hepatitis, and phlebotomy, which is the periodic removal of a pint of blood -- to reduce iron levels in hemochromatosis.
Much of the treatment is directed at complications.
- Your doctor may recommend a low-sodium diet and diuretics if you are retaining excess fluid in your body.
- Lactulose or other medication will be prescribed if you have confusion caused by hepatic encephalopathy. Lactulose is a laxative that decreases the absorption of certain substances toxic to the brain.
- Medications can be prescribed for itching and infections.
- Blood pressure medicines may help to lower pressure in the portal veins to decrease the risk of internal bleeding.
Bleeding varices pose an immediate, life threatening hazard. To prevent them from bleeding, doctors called gastroenterologists do endoscopy to find the varices and treat them. The varices can be injected with a solution to shrink them or they can be sealed with bands. The same procedure is done when varices are actively bleeding. Intravenous and oral drugs are also given to reduce bleeding.
The person may also need a procedure called transjugular intrahepatic portosystemic shunt (TIPS). This involves creating a new blood channel in the liver that relieves some of the high portal pressure. With less portal pressure, there is less bulging of the varices. And new varices are less likely to form.
If liver function becomes too impaired from cirrhosis, a transplant is the only treatment. Approximately 80% to 90% of patients survive liver transplantation, and long-term survival rates have improved because of drugs such as cyclosporine (Neoral, Sandimmune) that suppress the immune system to keep it from attacking the new liver.
When to call a professional
If you have any risk factors for liver disease, make an appointment with your doctor. Cirrhosis can often be prevented if action is taken early enough.
If you have cirrhosis, get immediate medical attention for:
- Vomiting blood
- Black, tarry stools
- High fever
- Abdominal pain
- Confusion.
Prognosis
Treatment leads to improvement in most cases when the disease is discovered in its earlier stages. Most patients are able to live a normal life for many years. The outlook is less favorable if liver damage is extensive or if someone with cirrhosis does not stop drinking. People with cirrhosis usually die of bleeding that can't be stopped, serious infections or kidney failure. They often enter irreversible coma in their last days.
Additional info
National Institute of Diabetes & Digestive & Kidney Disorders
https://www.niddk.nih.gov/
American Liver Foundation
https://www.liverfoundation.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.