Anal Fissure
Medically reviewed by Drugs.com. Last updated on May 4, 2025.
What is an anal fissure?
An anal fissure is a cut or tear in the tissue inside your anus. An anal fissure may be acute or chronic. An acute anal fissure is usually small and shallow and often heals without treatment. A chronic fissure may last longer than a month and will usually need treatment. A chronic anal fissure comes back after treatment.
What increases my risk for an anal fissure?
Anal fissures may occur when your anal muscle becomes too tight. Your anal muscle forms a ring around your anus and helps control your bowel movements. When this muscle becomes too tight, blood flow to your anus is decreased. You may also have too much pressure around your anus. Any of the following may increase your risk for an anal fissure:
- Constipation that causes you to strain while having a bowel movement, or diarrhea
- A condition such as Crohn disease or inflammatory bowel disease (IBS)
- Anal cancer, leukemia, or treatment for cancer, such as chemotherapy
- An infection such as HIV, syphilis, or tuberculosis (TB)
- Vaginal childbirth that tears the area between your vagina and anus, an anal injury or surgery, or anal intercourse
- Pressure from obesity or long periods of sitting
What are the signs and symptoms of an anal fissure?
- Pain that lasts several hours around your anus after you have a bowel movement
- Bleeding from your anus
- Bright red blood in your bowel movement or spots of blood on your toilet paper
- Pain while you urinate or have sex
- Spasms in your anus
- Itching around your anus
How is an anal fissure diagnosed?
Your healthcare provider will ask about your symptoms and when they started. Tell your provider about your bowel movements, foods you eat, and medicines you take. Your provider may also ask if you have other medical conditions, or had anal procedures or surgeries. Your provider will look at and feel your anus to check for cuts or tears. If you are in severe pain, you may get local anesthesia. Your provider may also remove a piece of anal tissue and send it to a lab for testing.
How is an anal fissure treated?
You may need to have the cause of your anal fissure treated. You may need any of the following to treat your anal fissure:
- Medicine:
- Stool softeners help make your bowel movements softer. This helps prevent constipation. You will be less likely to strain and cause an anal fissure if you are not constipated.
- Topical medicines may be given to help your anal muscle relax or to increase blood flow to your anus. Your provider will teach you the right way to use topical medicine.
- Botulinum toxin is given as a shot into the skin around your anus. It helps your anal muscle relax.
- Surgery may be needed if other treatments do not work. You may also need surgery if your anal fissure is very painful. The most common surgery is called a lateral internal sphincterotomy. A small part of your anal muscle is cut to help relax your anal muscle and decrease your pain. A fissurectomy may be used to remove all or some of your anal fissure.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage or prevent an anal fissure?
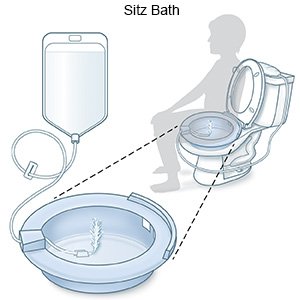
- Soak in a warm tub or take a sitz bath. A sitz bath may decrease your pain and relax your anal muscle. You may need to do this more than 1 time each day. Ask your healthcare provider for information on how to use a sitz bath.
- Eat foods that are high in fiber. This will help keep your bowel movements soft. High-fiber foods include fruits, vegetables, and whole grains.

- Drink more liquids. Liquids may help soften your bowel movements. This will help prevent you from straining. Ask your provider how much liquid you should drink each day and which liquids are best for you.
- Do not ignore the urge to have a bowel movement. Do not strain. Clean the area gently after every bowel movement.
- Avoid anal intercourse for as long as directed by your provider. Anal intercourse may make it harder for your anal fissure to heal.
When should I seek immediate care?
- You have severe pain in or around your anus.
- You have bleeding from your anus that does not stop.
When should I call my doctor?
- You have a fever.
- You still have pain after you take pain medicine.
- You are not able to have a bowel movement.
- You have spasms in your anus that do not stop.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
