Alpha-Gal Syndrome
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is alpha-gal syndrome (AGS)?
AGS is an allergic reaction to red meat or certain animal products. Alpha-gal is a type of sugar found in red meat, such as beef, pork, lamb, and venison. Animal products such as milk, or gelatin made from beef, also contain alpha-gal. Alpha-gal is not found in fish, birds, or other non-mammal animals. AGS develops after a tick bite, usually from a lone star tick. Allergic reactions range from mild to severe. The most severe reaction is anaphylaxis. Anaphylaxis is a sudden, life-threatening reaction that needs immediate treatment.
What are the signs and symptoms of AGS?
You may have an allergic reaction to some items that contain alpha-gal but not to others. You may not have a reaction every time you are exposed to alpha-gal. Any signs or symptoms that do develop usually begin 2 to 6 hours after exposure. You may be woken by an allergic reaction if you were exposed within 6 hours of going to sleep. The following are common reactions that may develop:
- Nausea, vomiting, or stomach pain
- Heartburn or diarrhea
- Itching, a rash, or swelling in your face, lips, throat, or tongue
- A cough or shortness of breath
How is AGS diagnosed?
Your healthcare provider will ask about your symptoms after you eat or are exposed to alpha-gal. Your provider will ask how long it takes for symptoms to appear and how long they last. Your provider will also ask about the amount that triggers symptoms. You may need to keep a diary to write down everything you are exposed to and any symptoms that develop. Your provider may recommend any of the following to confirm or rule out AGS:
- Blood tests may be used to find antibodies to something that contains alpha-gal. An antibody is a protein created by your immune system.
- A skin prick test is used to check for an allergy to red meat. Your provider will scratch tiny bits of different foods under your skin. If a bump appears within a few minutes, you likely have an allergy to that food.
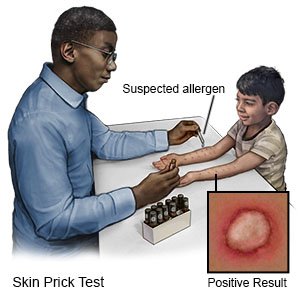
- An elimination diet is used to help you avoid anything you may be allergic to for several weeks. If you do not have an allergic reaction, you are exposed to potential allergens one at a time. A provider stays with you to watch for and treat any allergic reactions. When all potential allergens are tested, you will be given a list of any foods or products to avoid.
How is AGS treated?
AGS cannot be cured, but symptoms may get less severe or stop. This can take 8 months to 5 years. Until then, you will need to avoid being exposed to anything that triggers a reaction. You may need to see specialists, such as an allergist or dietitian, for ongoing care. The following medicines may be needed to manage allergic reactions:
- Antihistamines decrease mild symptoms such as itching or a rash.
- Steroids help reduce swelling.
- Epinephrine is used to treat severe allergic reactions such as anaphylaxis. Anaphylaxis symptoms include throat tightness, trouble breathing, tingling, dizziness, and wheezing. You will be taught how to use epinephrine if you are at risk for anaphylaxis.
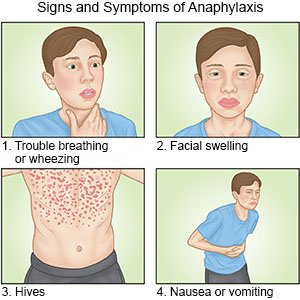
What can I do to manage or prevent AGS?
- Carry medical alert identification. Wear jewelry or carry a card that says you have a food allergy. Ask your provider where to get these items. Tell all healthcare providers you have AGS. Some medicines and vaccines contain or are coated with material that contains alpha-gal. Your provider can tell you what to do if the vaccine or medicine you need may cause a reaction.
- Know the ingredients of everything you eat and drink. Read food labels. Ask about ingredients when you go to restaurants. Ask if an ingredient that causes a reaction is used to prepare a dish you want to order. A dietitian can help you create meal plans to avoid allergens.
- Prevent or manage tick bites. A new tick bite can make AGS active again. If you go into areas that contain many trees, tall grasses, and underbrush, do the following:
- Prevent ticks from crawling through gaps in your clothing and onto your skin. Tuck your pant legs. Wear long sleeves that fit close to the skin at your wrists and neck. Wear a hat that fits close to your head.
- Apply insect repellant that contains DEET. Spray permethrin on your clothing. Apply repellant on exposed skin. Do not apply insect repellant on your child's face or hands.
- Check your and your child's clothing, hair, and skin for ticks. Shower within 2 hours of coming indoors. Carefully check the hairline, armpits, neck, and waist. Also check your pets after they are in tick-prone areas. Ask your pet's veterinarian about the best tick prevention products to use on your pet.
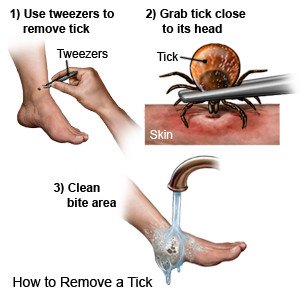
- Mange tick bites safely. Put on gloves. Use tweezers to grasp the tick as close to your skin as possible. Pull the tick straight up and out. Do not touch the tick with your bare hands. Check to make sure you removed the whole tick, including the head. Do not crush or squeeze the tick. Flush the tick down the toilet. Clean your skin with soap and water or rubbing alcohol. Then wash your hands with soap and water.
Have someone call your local emergency number (911 in the US) if:
- You have trouble breathing, wheezing or severe shortness of breath.
- Your heart is pounding or racing.
- You have swelling in your mouth or throat.
- You feel lighthearted or faint.
When should I seek immediate care?
- You have itching or hives that spread all over your body.
When should I call my doctor?
- You have new or worsening rashes, hives, or itching.
- You have an upset stomach or are vomiting.
- You have stomach cramps or diarrhea.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
