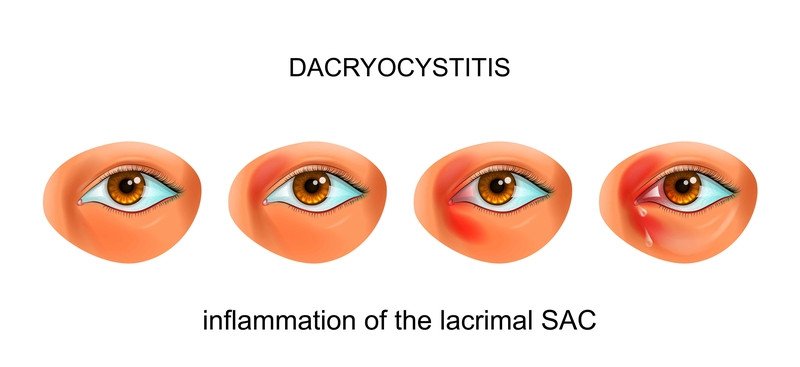
Tear duct infection (dacryocystitis)
Medically reviewed by Drugs.com. Last updated on May 15, 2024.
What is dacryocystitis?

Dacryocystitis is an infection in the tear drainage system. Tears drain from each eye through small canals, a tear sac (lacrimal sac) and a tear duct (nasolacrimal duct).
Tears are made by a small organ above the eye under the upper lid. At the inner corner of each upper and lower eyelid is an opening to a small tube (drainage canal). The drainage canals carry away tears that have rinsed the front surface of the eye away so fresh tears can come in.
The drainage canals empty into tear sacs, one for each eye. The tear sacs sit at the top of the tear duct. Tears move through the sac into the duct and then are dumped into your nose.
Tears spill out of the eyes and into the back of your nose when you cry, although the tears entering the nose are not visible. That's why you get a runny nose when you cry.
The tear drainage system can get infected if it becomes blocked and bacteria collect in the ducts or the lacrimal sac. A blockage near the nose also can cause excessive tearing from the eye.
|
|
Although tear duct infections can occur at any age, they are most common in infants, who commonly have a congenital (inborn) obstruction of the nasolacrimal duct. Infants with this problem have a narrower drainage passageway that will widen with time as they grow. Most children with the disorder outgrow it by the time they are 1 year old.
If adults get a tear duct infections, it usually is because their tear ducts have become abnormally narrowed by continued growth of surrounding bone. The ducts are more rigid and less able to flush out the debris that can cause blockages.
Tear ducts also can become blocked after trauma to the nose or eyes, such as a broken nose, or by nasal polyps.
When a tear duct infection first occurs, it is called acute dacryocystitis. If a tear duct infection is not treated quickly or if it causes minor symptoms that build up over a long period, it can be more difficult to cure. The infection is then called chronic dacryocystitis.
Symptoms of dacryocystitis
Typical symptoms of acute tear duct infection include:
- pain, redness, and swelling of the lower eyelid at the inner corner of the eye
- excessive tearing
- pus or discharge from the eye
- fever.
Symptoms of chronic (long-lasting) tear duct blockage are less severe. Although there may be tearing and perhaps some pus or discharge, usually there is little or no pain, redness or swelling.
Diagnosing dacryocystitis
Your doctor will examine you for signs of swelling and redness at the corner of the eye, fever, excessive tearing and discharge of pus. Pressing on the lacrimal sac may cause mucus or pus to come out of the ducts near the eye. If pus is present, a sample of the discharge can be collected and tested to determine the type of bacteria causing the infection.
If the physical signs do not obviously show dacryocystitis, or if the doctor wants to confirm the diagnosis, he or she may do a dye disappearance test. With this test, a yellow fluorescent dye is placed in the corner of the eye and allowed to mix with the eye's film of tears. If the tear drainage system is functioning well, the dye should disappear from the eye's surface after several minutes. A cotton swab can be inserted into the nose to see if any dye has passed through the tear duct. This test can help your doctor tell whether your tear duct is blocked completely or partially.
Expected duration of dacryocystitis
In infants or adults, tear duct infections need to be treated when there is redness or fever and cloudy tear drainage. Acute tear duct infections usually will go away quickly with antibiotic therapy. Between episodes of acute infection, there may still be excessive tearing or cloudy drainage from block tear ducts. In infants, the obstruction that causes an infection is commonly outgrown by the age of 9 to 12 months. Chronic infections, especially in adults, can be difficult to cure without surgery to expand the tear duct's drainage channel.
Preventing dacryocystitis
If a child is prone to tear duct infections, here's a routine that helps decrease the frequency of infections. First, wash your hands thoroughly. Apply a warm compress (a warm, wet clean washcloth) over the area of the tear sac. Then, place your index finger sideways along the bony ridge beneath the child's eye, with your finger pointing toward the top of the nose. Firmly, but gently, apply pressure with your finger tip between the eye and nose. This pressure will compress and empty the tear sac, flushing the duct below. After this, rinse and re-warm the compress. Apply it again to the same area for one or two minutes.
Treating dacryocystitis
Antibiotics that can be taken by mouth are the standard treatment for tear duct infection. However, a severe infection requires initial intravenous antibiotics and observation in the hospital.
In general, antibiotics clear up acute infections quickly. Antibiotics are also used to treat chronic infections. In some cases, antibiotic ointment or eye drops may be prescribed. Do not attempt to apply an over-the-counter antibiotic ointment to the eye or the area around the eye, since over-the-counter ointments are not made for use in the eye and could have irritating ingredients.
If the infection does not respond to antibiotics, or if infections keep returning, minor surgery may be needed. There are several types of surgical treatments for tear duct infections:
- Surgical probing of the tear duct, in which a thin wire is guided through the tear duct to clear out any blockage. This is the most common treatment for recurring infections in infants.
- A procedure called dacryocystorhinostomy, in which the narrowed or blocked duct is expanded. This usually requires removal of bone that has caused the duct's narrowing. This surgery commonly is done with the aid of a laser.
- Removing all or part of the lacrimal sac.
When to call a professional
Call a health care professional if you or your child experiences any of the eye symptoms of an infection, including pain, excessive tearing, redness, swelling or pus.
Prognosis
There are treatments for just about any cause or severity of tear duct infection, so the outlook for this problem is good.
Most children outgrow a problem with blocked tear ducts by the time they are 1 year old.
Additional info
American Academy of Ophthalmology
https://www.aao.org
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.