Kawasaki Disease
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is Kawasaki disease?
Kawasaki disease (KD) is an illness in children that causes fever and inflammation of blood vessels. It usually occurs in children younger than 5 years old. KD can damage blood vessels in your child's heart. It can become life-threatening. KD can also cause heart problems as your child gets older, even into adulthood. The exact cause of KD is unknown. Healthcare providers believe it may be caused by an infection.
What are the signs and symptoms of KD?
There are 3 phases of KD. Most symptoms appear in the first phase. The first phase can last up to 2 weeks. Heart damage can happen during this phase. During the second phase, your child may not have any symptoms except peeling of your child's hands and feet. The second phase may last up to 4 weeks. In the third phase, your child will recover. You may notice ridges in his or her nails. This phase may last for years. The following are common symptoms of the first phase:
- Fever stays above 101.3°F (38.5°C) even with treatment
- Red, dry, cracked lips
- A red tongue with small raised bumps
- Red eyes
- Skin rash, usually on the torso
- Swollen lymph nodes, usually on one side of your child's neck
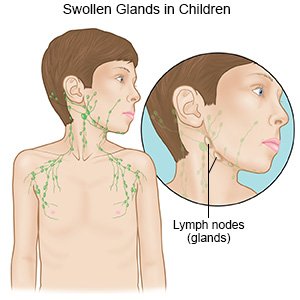
- Redness and swelling of your child's hands and feet
- Crying or fussing more than usual
How is KD diagnosed?
Your child's healthcare provider will ask about your child's symptoms and when they started. The provider will examine your child and listen to his or her heart. There is no specific test to diagnose KD. Your child may need any of the following tests:
- Blood and urine tests give information about your child's overall health, such as liver and kidney function. These tests will also show if your child has an infection.
- An EKG records your child's heart rhythm and how fast his or her heart beats. It is used to check for heart damage.
- An x-ray, echocardiogram, CT scan, or MRI may be used to help healthcare providers see your child's heart and blood vessels. Your child may be given contrast dye before these tests. Tell the healthcare provider if your child has ever had an allergic reaction to contrast dye. Do not let your child enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if your child has any metal in or on his or her body.
How is KD treated?
Your child will be hospitalized until he or she does not have a fever for 2 days. He or she may receive the following medicines:
- Aspirin helps prevent blood clots. Aspirin may cause your child to bleed or bruise more easily. If you are told to give your child aspirin, do not give him or her acetaminophen or ibuprofen instead. Give aspirin to your child exactly as directed. Aspirin may cause a serious illness called Reye syndrome. Reye syndrome may cause brain and liver damage. Ask your child's healthcare provider for more information about Reye syndrome.
- Immune globulin may be given to help your child's immune system fight infection. This medicine will be given while your child is in the hospital.
- Anticoagulants may be given if your child is at increased risk for blood clots.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to prevent the spread of germs?
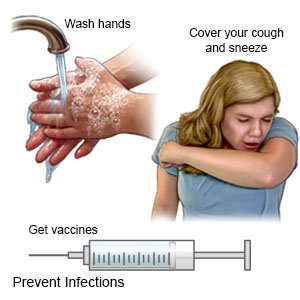 |
- Keep your child away from other people while he or she is sick. This is especially important during the first 3 to 5 days of illness. The virus is most contagious during this time.
- Have your child wash his or her hands often. He or she should wash after using the bathroom and before preparing or eating food. Have your child use soap and water. Show him or her how to rub soapy hands together, lacing the fingers. Wash the front and back of the hands, and in between the fingers. The fingers of one hand can scrub under the fingernails of the other hand. Teach your child to wash for at least 20 seconds. Use a timer, or sing a song that is at least 20 seconds. An example is the happy birthday song 2 times. Have your child rinse with warm, running water for several seconds. Then dry with a clean towel or paper towel. Your older child can use hand sanitizer with alcohol if soap and water are not available.

- Remind your child to cover a sneeze or cough. Show your child how to use a tissue to cover his or her mouth and nose. Have your child throw the tissue away in a trash can right away. Then your child should wash his or her hands well or use a hand sanitizer. Show your child how to use the bend of his or her arm if a tissue is not available.
- Tell your child not to share items. Examples include toys, drinks, and food.
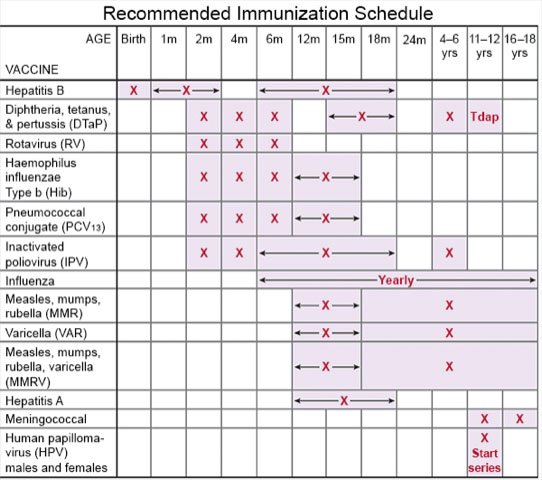
- Ask about vaccines your child needs. Vaccines help prevent some infections that cause disease. Have your child get a yearly flu vaccine as soon as recommended, usually in September or October. Your child's healthcare provider can tell you other vaccines your child should get, and when to get them.
Call your local emergency number (911 in the US) if:
- Your child has any of the following signs of a heart attack:
- Squeezing, pressure, or pain in his or her chest that lasts longer than 5 minutes or returns
- Discomfort or pain in his or her back, neck, jaw, stomach, or arm
- Trouble breathing
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat, especially with chest pain or trouble breathing
- Your child has any of the following signs of a stroke:
- Numbness or drooping on one side of his or her face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
When should I call my child's doctor?
- Your child has been around someone with chicken pox or the flu.
- Your child's symptoms return.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Kawasaki Disease
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
