Testicular Cancer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is testicular cancer?
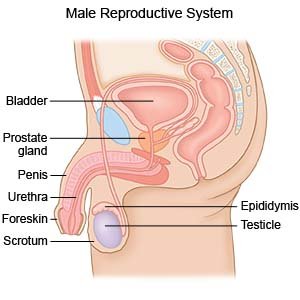
Most testicular cancer starts in the sperm-making cells of the testicles. Testicular cancer occurs most commonly in males aged 15 to 39 years.
 |
What increases my risk for testicular cancer?
- One or both testicles did not descend (drop) into your scrotum
- A genetic disorder, such as Klinefelter syndrome
- A family history of testicular cancer
- Smoking cigarettes
What are the signs and symptoms of testicular cancer?
- A painless lump or change in how your testicle feels
- Your testicle becomes larger or smaller
- Swelling of your scrotum
- A feeling of heaviness in the scrotum
- A dull ache in the lower abdomen or in the groin
- Pain or discomfort in your testicle or scrotum
- Breast swelling or tenderness
How is testicular cancer diagnosed?
Your healthcare provider may shine a small flashlight on your scrotum. This may show a lump in or on your testicle. You may need one or more of the following tests:
- Blood tests may be used to check for cancer markers.
- An ultrasound or CT may show if the cancer has spread. You may be given contrast liquid to help the cancer show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- A biopsy may be used to take tissue from the testicle to be tested for the type of testicular cancer.
- Lymphangiography is a procedure that uses dye to see if the cancer has spread to your lymph nodes.
Will testicular cancer affect my ability to have sex?
A male with 1 normal healthy testicle can still have sex and make sperm. Before treatment, ask your healthcare provider how your ability to have sex may change. Treatment can affect these abilities. You may have your sperm removed and frozen so that you can father a child at a later time.
How is testicular cancer treated?
- Surgery may be needed to remove your testicle. Lymph nodes that contain cancer may also be removed.
- Radiation therapy kills cancer cells and may stop the cancer from spreading with x-rays or gamma rays.
- Chemotherapy medicine is used to treat cancer by killing cancer cells. Chemotherapy may also be used to shrink lymph nodes that have cancer in them.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to manage my testicular cancer?
- Do not smoke. Nicotine can damage blood vessels and make it more difficult to manage your testicular cancer. Smoking also increases your risk for new or returning cancer and delays healing after treatment. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your healthcare provider for information if you currently smoke and need help quitting.
- Drink liquids as directed. Drink extra liquids to prevent dehydration. You will also need to replace fluid if you are vomiting or have diarrhea from cancer treatments. Ask your healthcare provider which liquids to drink and how much you need each day.
- Limit or do not drink alcohol as directed. Limit alcohol to 2 drinks per day. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Eat healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask if you need to be on a special diet.

- Be physically active as directed. Physical activity can help increase your energy level. Ask your healthcare provider about the best activity plan for you.

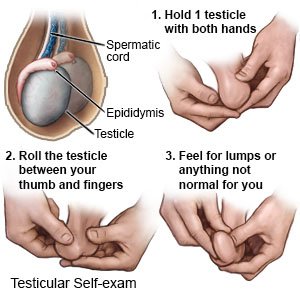
How should I do a testicular self-exam?
A testicular self-exam (TSE) can help you learn how your testicles normally look and feel. Ask your healthcare provider or oncologist for more information about a TSE and how often to do one.
- Stand in front of a mirror and look at your scrotum. Look for changes in its shape, size, and color. It may be normal for one side of your scrotum to be larger or to hang lower than the other.
- Examine one testicle at a time. Put the thumbs of both hands in front of the testicle. Put the second (pointer) fingers behind the testicle. Gently roll each testicle between the thumbs and fingers of both hands. Feel for any lumps or changes in the testicle. It may be normal for one of your testicles to feel slightly larger than the other. Find a long, cord-like tube on top and in back of each testicle. This is the epididymis. Feel for any changes in the epididymis.
 |
When should I seek immediate care?
- Your leg feels warm, tender, and painful. It may look swollen and red.
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
- You are confused or cannot think clearly.
When should I call my doctor?
- You have a fever.
- You are vomiting and cannot keep any food or liquids down.
- You feel lumps or other changes in your testicle.
- You are depressed and feel you cannot cope with your illness.
- You have pain that does not decrease or go away after you take your pain medicine.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Testicular Cancer
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
