Tenosynovitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is tenosynovitis?
Tenosynovitis is inflammation of a tendon and its synovium. Tendons are cords of tissue that connect muscles to bones. The synovium is the lining of the sheath around the tendon. The tendons may become thickened and not slide smoothly through the swollen lining.
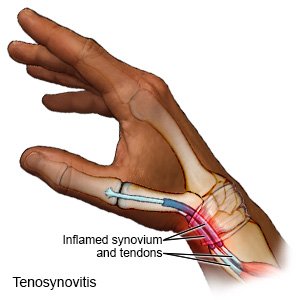 |
What increases my risk for tenosynovitis?
- Overuse
- Infection
- Pressure on the tendon
- Injury
What are the signs and symptoms of tenosynovitis?
- Pain, redness, or swelling that may get worse or be present at rest
- Fingers, toes, or ankles may click, lock, or snap
- Grating sound or feeling
- A bump on your toes or swollen fingers
- Stiffening of the fingers, ankle, or toes
- Weakness and limited movement of the affected part
How is tenosynovitis diagnosed?
Your healthcare provider will move your body part in different directions to check for pain, weakness, or movement problems. You may also need any of the following:
- Blood tests or a sample of fluid may show if your tenosynovitis is caused by infection.
- An x-ray, ultrasound, or MRI may show the cause of your tenosynovitis. You may be given contrast liquid to help the tendon show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
How is tenosynovitis treated?
- Medicines may be needed to treat or prevent pain, inflammation, or an infection.
- Surgery may be needed if other treatments do not work or your symptoms are severe. Your surgeon may need to clean the area around your tendon so it can heal properly.
How can I manage my symptoms?
- Rest the inflamed area as directed.
- Apply ice on your inflamed area for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel. Ice helps prevent tissue damage and decreases swelling and pain.
- Elevate the inflamed area above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your inflamed area on pillows or blankets to keep it elevated comfortably.
- Use your assistive device as directed. You may need a brace, splint, walking boot, or cast. You may also need to use crutches or orthotics. These devices prevent movement, decrease pain, and help your tendon heal.
- Go to physical or occupational therapy as directed. A physical therapist teaches you exercises to help improve movement and strength and decrease pain. An occupational therapist teaches you skills to help with your daily activities.
Call your local emergency number (911 in the US) if:
- You have sudden trouble breathing or chest pain.
When should I seek immediate care?
- Your arm, leg, fingers, or toes are numb, tingle, or are pale.
- You hear or feel a pop in a joint.
- You have severe pain.
When should I call my doctor?
- You have a fever.
- A joint near your inflamed area is red and swollen.
- Your symptoms do not go away or they get worse, even after treatment.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
