Sinusitis in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is sinusitis?
Sinusitis is inflammation or infection of your child's sinuses. Sinusitis is most often caused by a virus. Acute sinusitis may last up to 30 days. Chronic sinusitis lasts longer than 90 days. Recurrent sinusitis means your child has sinusitis 3 times in 6 months or 4 times in 1 year.
What increases my child's risk for sinusitis?
- Allergies
- Upper respiratory infection caused by a virus
- Dental infections or procedures
- Group daycare or child care
- Certain medical conditions such as immune system disorder, cystic fibrosis, or asthma
- Smoking or exposure to secondhand smoke
- Large or extra tissue in the mouth or throat or cleft palate
What are the signs and symptoms of sinusitis?
- Fever
- Pain, pressure, redness, or swelling around the forehead, cheeks, or eyes
- Thick yellow or green discharge from your child's nose
- Tenderness when you touch your child's face over his or her sinuses
- Dry cough that happens mostly at night or when your child lies down
- Sore throat or bad breath
- Headache and face pain that is worse when your child leans forward
- Tooth pain or pain when your child chews
How is sinusitis diagnosed?
Your child's healthcare provider will examine your child and ask about his or her symptoms. The provider will check inside your child's nose using a nasal speculum. This is a small tool used to open the nostrils. A sample of the mucus from your child's nose may show what germ is causing his or her infection.
How is sinusitis treated?
Your child's symptoms may go away on their own. Your child's healthcare provider may recommend watchful waiting for 3 days before starting antibiotics. Your child may need any of the following:
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to give your child and how often to give it. Follow directions. Read the labels of all other medicines your child uses to see if they also contain acetaminophen, or ask your child's doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If your child takes blood thinner medicine, always ask if NSAIDs are safe for him or her. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Nasal steroid sprays may help decrease inflammation in your child's nose and sinuses.
- Antibiotics help treat or prevent a bacterial infection.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my child's symptoms?
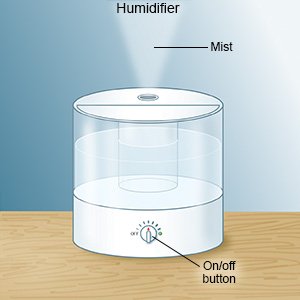
- Use a humidifier to increase air moisture in your home. This may make it easier for your child to breathe and help decrease his or her cough.
- Help your child rinse his or her sinuses. Use a sinus rinse device to rinse your child's nasal passages with a saline (salt water) solution or distilled water. Do not use tap water. A sinus rinse will help thin the mucus in your child's nose and rinse away pollen and dirt. It will also help reduce swelling so your child can breathe normally. Ask your child's healthcare provider how often to do this.
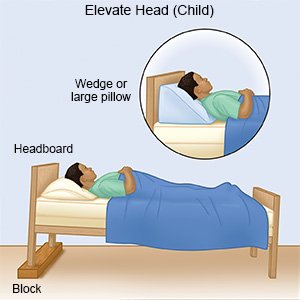
- Have your older child sleep with his or her head elevated. Place an extra pillow under your child's head before he or she goes to sleep to help the sinuses drain. Ask if your child is old enough to sleep with an extra pillow under his or her head.
- Give your child liquids as directed. Liquids will thin the mucus in your child's nose and help it drain. Ask your child's healthcare provider how much liquid to give your child and which liquids are best for him or her. Avoid drinks that contain caffeine.
How can I help prevent the spread of germs?
- Help your child avoid others when he or she is sick. Some germs spread easily and quickly through contact. Have your child stay home from school or daycare. Ask when it is okay for your child to return.
- Wash your and your child's hands often with soap and water. Encourage your child to wash his or her hands after using the bathroom, coughing, or sneezing.

When should I seek immediate care?
- Your child's eye and eyelid are red, swollen, and painful.
- Your child cannot open his or her eye.
- Your child has vision changes, such as double vision.
- Your child's eyeball bulges out or your child cannot move his or her eye.
- Your child is more sleepy than normal, or you notice changes in his or her ability to think, move, or talk.
- Your child has a stiff neck, a fever, or a bad headache.
- Your child's forehead or scalp is swollen.
When should I call my child's doctor?
- Your child's symptoms get worse after 5 to 7 days.
- Your child's symptoms do not go away after 10 days.
- Your child has nausea and is vomiting.
- Your child's nose is bleeding.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Sinusitis
Treatment options
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
