Screening for Colorectal Cancer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about colorectal cancer?
Screening means you are checked for colorectal cancer, even if you do not have signs or symptoms. Colorectal cancer is the third leading cause of death in the United States and Canada. Regular screening can find problems early and treatment can begin. Early treatment can save your life.
What types of screenings are available?
Your healthcare provider will talk to you about the benefits and risks of each type of screening. Your provider will work with you to decide which screening is best for you. Your provider will also tell you when to start getting screened.
- Fecal occult blood testing (FOBT) can be collected at home. FOBT checks for blood in your bowel movements. You will need a small sample of 2 to 3 bowel movements. Your healthcare provider will give you special cards to put the sample on. You will return the cards to your provider's office or a lab for the test to be done. If your test is positive for blood, you will need to have a colonoscopy. A flexible sigmoidoscopy or colonoscopy may help find where the blood is coming from. The blood may mean you have polyps, cancer, or other conditions, such as hemorrhoids. You may have to avoid certain medicines and food for about 3 days before you collect the sample. Your provider will tell what medicines and foods to avoid. If blood is not found, you may need to do the test next year.
- A fecal immunochemical test (FIT) is also collected at home and then sent to a lab for testing. FIT also tests for blood in your bowel movements. You do not have to avoid any medicines or foods for FIT. You collect a sample from 1 bowel movement and put it in the special container. The container is either mailed or taken to your healthcare provider's office or lab. If blood is found, you may need a flexible sigmoidoscopy or colonoscopy. If blood is not found, you may need to do the test next year.
- A sigmoidoscopy is a procedure to look inside your rectum and sigmoid colon. The sigmoid colon is the lower part of your intestines, closest to your rectum. A sigmoidoscope will be inserted into your rectum. This is a tube with a light and tiny camera on the end. Pictures of your colon appear on a monitor during the procedure. A flexible sigmoidoscopy may help diagnose colon cancer, inflammation, polyps (growths), or infections.
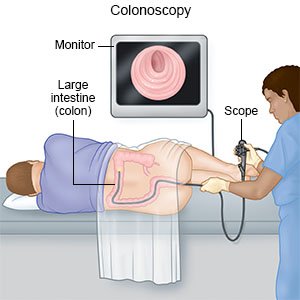
- A colonoscopy is a procedure to examine the inside of your colon (intestine) with a scope. A scope is a flexible tube with a small light and camera on the end. Polyps or tissue growths may be removed and tested for cancer during your colonoscopy.
How often will I need colorectal cancer screening?
Screening is recommended starting at age 45 and continuing to age 75 if you are at average risk. Screening may start before you are 45 or continue after you are 75 if your risk is high. Your provider will tell you how often to get screened. Timing depends on the type of screening and if polyps or other problems were found. Timing also depends on your age and if you are at increased risk for cancer. Screening may be recommended every 1, 2, 5, or 10 years.
What are the risks of colorectal cancer screening?
Any type of screening has risks. Talk with your healthcare provider about the risks of screening. Your provider may tell you the following:
- A false-negative result can happen. The result can delay treatment because it shows no cancer was found. It may cause you to not seek treatment even when you have symptoms.
- A false-positive result can happen. This result can cause you to have more tests. It can also cause you to feel anxious if you think you have cancer.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
