Primary Ciliary Dyskinesia in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Primary ciliary dyskinesia (PCD) is a disorder that affects the cilia in your child's body. Cilia are hair-like structures around cells that normally move like waves. Cilia in the lungs, ears, and sinuses normally carry mucus out. When mucus cannot be carried out, it sits in your child's airway. Bacteria in the mucus increase, leading to lung infections or respiratory failure. Your child may have fertility problems (trouble having children) later in life. PCD can keep certain parts of the reproductive system from working correctly. PCD is a genetic disorder (passed from both parents to the child).
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- Your child has sudden chest pain.
- Your child has sudden or more severe trouble breathing.
- Your child is confused or feels faint.
Call your child's pediatrician if:
- Your child's lips or fingernails turn gray or blue.
- Your child coughs up blood.
- Your child has a fever.
- Your child coughs more than usual or wheezes.
- Your child's medicines do not relieve his or her symptoms.
- You have questions or concerns about your child's condition or care.
Medicines:
Do not give your child cough suppressants (medicine to prevent coughing). It is important that your child cough out mucus and irritants to prevent respiratory infections.
- Antibiotics may be given to prevent or fight an infection caused by bacteria.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Give your child's medicine as directed. Contact your child's healthcare provider if you think the medicine is not working as expected. Tell the provider if your child is allergic to any medicine. Keep a current list of the medicines, vitamins, and herbs your child takes. Include the amounts, and when, how, and why they are taken. Bring the list or the medicines in their containers to follow-up visits. Carry your child's medicine list with you in case of an emergency.
Manage your child's PCD:
Tell your child's healthcare provider right away when he or she has signs of a respiratory infection. Early treatment may help control the infection so it does not become severe. The following can help you and your child manage PCD and protect his or her airway:
- Take your child to pulmonary rehabilitation (rehab) as directed. Pulmonary rehab is a program that can help your child learn how to prevent breathing problems. The rehab team includes lung and ear, nose, and throat specialists, and respiratory therapists. The team will help your child create an aerobic exercise plan. Aerobic exercise is one of the best ways to manage PCD. Exercises such as walking, swimming, or riding a bicycle help strengthen your child's heart and lungs. The rehab program will change as your child gets older and becomes responsible for his or her own care.
- Keep your child's airway clear and open. Have your child do airway clearance techniques as needed. Healthcare providers will show your child how to do these in pulmonary rehab. Help thin mucus by having your child drink more liquids or use a cool mist humidifier.
- Prevent infections. Keep your child away from people who are sick. Have your child wash his or her hands often. Use soap and water, or a gel hand sanitizer if soap and water are not available.

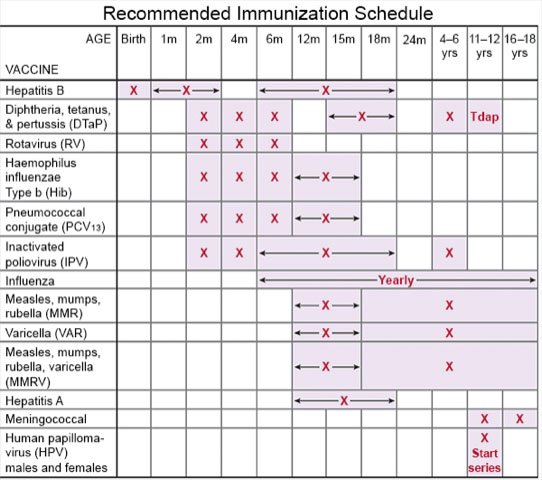
- Talk to your child's healthcare provider about vaccines. Children get vaccines on a regular schedule. Your child's provider can help you schedule catch-up doses if your child has not received all the recommended vaccines. Take your child to get a flu vaccine every year as soon as it becomes available. Your child may also need a vaccine to help prevent pneumonia.
- Do not smoke around your child or let others smoke around him or her. Do not let your adolescent smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage and make breathing problems worse. Ask your adolescent's healthcare provider for information if he or she currently smokes and needs help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to healthcare providers before he or she uses these products.
Follow up with your child's pediatrician or specialist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
