Photorefractive Keratectomy
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
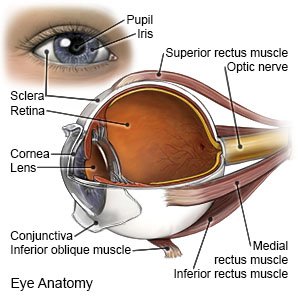
Photorefractive keratectomy (PRK)
is laser surgery to correct refractive errors of the eye. Refractive errors are common eye disorders that cause blurred vision. These errors happen when there is a problem in the refraction (bending) of light in the eye. They are often caused by an abnormal shape and texture of the cornea. The cornea is the clear outer layer of your eye. PRK uses a laser to reshape your cornea or make it smoother. This helps light to focus better in the eye, which leads to clearer vision.
 |
How to prepare for PRK:
- Arrange to have someone drive you home after surgery and stay with you for a few hours. You may be groggy or sleepy for several hours after surgery. It is important to have someone available to help you and watch for problems that need immediate care.
- You may need to stop wearing your soft contact lenses at least 1 week before surgery. You may need to stop wearing your gas-permeable contact lenses at least 3 weeks before surgery.
- Do not wear makeup or lotion on your face on the day of surgery.
- Your healthcare provider may give you medicine to help you stay calm and relaxed during surgery. Tell the provider if you have ever had an allergic reaction to anesthesia or numbing medicine.
What will happen during PRK:
- Your healthcare provider will place eyedrops into your eyes. These include antibiotic eyedrops to help prevent infection and numbing drops to prevent pain. Your eyelashes and the area around your eyes will be cleaned. A speculum (eyelid holder) will gently hold your eyelids open to keep you from blinking. The laser will be programmed to correct your refraction error.
- Your healthcare provider will remove the epithelium of your cornea with the laser. The epithelium is a thin layer of tissue that covers and protects the cornea. He or she will tell you to focus on a target light while he reshapes your cornea. It is important to keep your gaze focused on the light so the laser can work correctly. A soft bandage contact lens may be placed into each of your eyes to help the corneas heal.
What will happen after PRK:
- A lens will be put in your eye to protect it while you heal. You will keep it in for about a week after surgery. Your provider will remove it when you have healed.
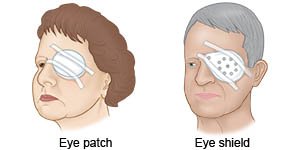
- A bandage and protective clear plastic eye shield may be used to cover your eye. This will help remind you to not rub or touch your eye.
- Medicines will be given as eyedrops to prevent a bacterial infection and reduce inflammation. You may also be given pain medicine.
- You will need to see your eye specialist soon after surgery and then regularly for the first 6 months. This is to make sure your eye is healing properly and your vision is stable. After 6 months, you should not notice any more changes in your vision. You may need to have another procedure if your vision changes after 6 months.
- Your provider will tell you when it is okay to start driving again. This is usually in about 1 to 3 weeks after surgery.
Risks of PRK:
You may get an infection. Nerves or blood vessels may be damaged during surgery. You may need another eye surgery. It may take longer than expected for your cornea to heal. You may have increased pain. Your vision may be worse than before surgery. You may develop glaucoma (increased pressure), cataracts (clouding of the lens), or long-term inflammation. You may lose your vision. You may have dry eyes. Scars may form on your corneas. You may have other eye problems, such as permanent glare, haze, or halos around lights at night.
Seek care immediately if:
- You feel sudden, sharp eye pain.
- You suddenly lose your vision.
- Your eye problems, such as blurred vision, become worse.
Contact your eye specialist if:
- You accidently rub or touch your eye.
- You see flashing lights.
- Your eyes are red or drain pus.
- You have any questions or concerns about your surgery, condition, or care.
Medicines:
It is very important that you use the following eyedrops as directed. You may need to continue using them daily for up to 4 months.
- Antibiotic eyedrops help prevent an infection caused by bacteria.
- Steroid eyedrops help decrease eye inflammation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Follow up with your eye specialist as directed:
You will need to return to have your eyes checked and the soft bandage contact lens removed. Write down your questions so you remember to ask them during your visits.
Eye care:
- Do not rub your eyes for at least 3 months. Rubbing your eyes can move or damage the flaps.
- Rest your eyes. Use your eye shield, eye patch, or corrective lenses as directed. Get plenty of sleep. Limit activities that strain your eyes, such as reading.
- Use lubricating eyedrops as directed. You will need to use drops that do not contain preservatives at first. Your eye specialist will tell you how long to use preservative-free drops. Talk to your provider if dry eye continues for longer than the first week after surgery.
- Ask about activity. You may need to avoid exercise and contact sports. Do not swim, sit in a hot tub, fly, or scuba dive until your healthcare provider says it is okay. These activities increase the pressure in your eyes. Ask when you can start to wear makeup.
- Use proper lighting. This will help you see more clearly. Use lights that decrease glare in your home or workplace.
- Wear sunglasses outside. This will help protect your eyes and decrease sensitivity to light.
Follow up with your doctor as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
