Pelvic Fracture
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a pelvic fracture?
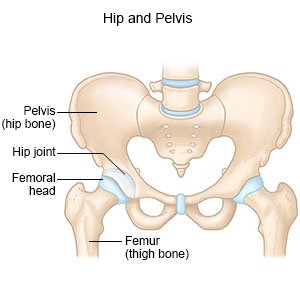
A pelvic fracture is a break in a pelvic bone or hip joint.
 |
What are the signs and symptoms of a pelvic fracture?
- Pain, tenderness, bruising, or swelling in your pelvic bone area
- Numbness or tingling in your groin or upper thighs
- Discomfort or pain when you sit, stand, walk, or have a bowel movement
- Leg or thigh bone turns outward
- Legs are not the same length
How is a pelvic fracture diagnosed?
Your healthcare provider will examine your pelvic area. He or she will also check the range of motion of your hip. An x-ray or CT scan of your pelvis may be used to check for broken bones. You may be given contrast liquid to help a fracture show up better in pictures. Tell your healthcare provider if you have ever had an allergic reaction to contrast liquid.
How is a pelvic fracture treated?
Treatment depends on the kind of fracture you have. You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Bed rest will help protect your pelvis while the fracture heals.
- Apply ice on your hip joint or pelvis for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it. Ice helps prevent tissue damage and decreases swelling and pain.
- Crutches or a walker may be needed to keep weight off the bone until it heals.
- An external fixation device may be put on your hips to hold the broken bones together while they heal. Screws or a clamp will be used to hold the device to your pelvic bones.
- Surgery may be needed for a severe pelvic fracture. Metal pins, screws, or plates may be used to hold your pelvic bone together.
Call your local emergency number (911 in the US) if:
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
When should I seek immediate care?
- Your leg feels warm, tender, and painful. It may look swollen and red.
- Your legs and feet turn blue or feel cold and numb.
When should I call my doctor?
- Your skin is itchy, swollen, or has a rash.
- Your pain or swelling increases.
- You have new symptoms.
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Pelvic Fracture
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
