Pediatric Comfort Measures
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What are comfort measures?
Comfort measures are ways your child's suffering can be eased during end-of-life care. Care can be provided at home or in a hospital. It can also be provided in a hospice or long-term care facility. Comfort measures are sometimes called palliative measures, but they are different. Palliative care can be given for any disease or illness, even if the person recovers. Comfort measures are only given when treatment will no longer be effective.
Who provides comfort measures?
Your child's comfort care team may include any of the following:
- Doctors, nurses, and dietitians
- Pain specialists and pharmacists
- Chaplains, social workers, and counselors
How will my child's symptoms be managed?
It may be difficult to see your child in pain or having any discomfort. Talk to your child's care team if you have any questions or concerns. They will work with you to make sure your child is as comfortable as possible.
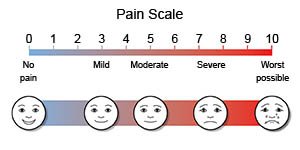
- Pain may be relieved with medicine. Your child may instead choose other methods, such as massage, music, or aromatherapy. Your child's team will ask how the pain is affecting his or her quality of life. Your child may be asked to describe the pain by choosing a face on a pain scale picture.
- Shortness of breath may be relieved with extra oxygen or breathing treatments. Your child may feel short of breath all the time, or only with activity. He or she may feel a little winded, or struggling to breathe. Comfort care will depend on what is causing your child's shortness of breath.
- Physical symptoms can be relieved or treated to improve your child's comfort. Examples include nausea, fatigue, and sleep problems. Your child's skin can be treated or soothed if it is irritated or he or she develops a pressure injury from lying in bed. Some treatment may help relieve your child's symptoms even though it will not cure the disease. An example is radiation. Radiation will not cure the cancer, but it can make the tumor smaller. This may help relieve pain or other symptoms caused by the tumor.
- Emotional symptoms such as anxiety, sadness, or depression may affect your child's quality of life. These symptoms may be treated with medicines. Other methods include deep breathing and meditation. Your child may also want to talk to a counselor or spiritual advisor.
What support services may be offered?
- Care support is given to help your child and his or her family. Your child's team can answer any questions your child or his or her family members have.
- Emotional and psychological support is provided to help your child and those close to him or her. Team members will meet with your child and his or her family regularly about your child's condition. Your child and those close to him or her may also join support groups or meet others receiving comfort measures.
- Spiritual and cultural support helps your child and his or her family evaluate religious values and cultural beliefs. This may make it easier to understand and accept your child's condition.
Where can I find more information?
- National Hospice & Palliative Care Organization (NHPCO)
1731 King Street, Suite 100
Alexandria , VA 22314
Phone: 1- 800 - 658-8898
Web Address: https://www.nhpco.org/
- Children's Project on Palliative/Hospice Services (ChiPPS)
National Hospice and Palliative Care Organization
1731 King Street, Suite 100
Alexandria , VA 22314
Phone: 1- 800 - 658-8898
Web Address: https://www.nhpco.org/pediatric
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
