Patent Ductus Arteriosus in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is patent ductus arteriosus (PDA)?
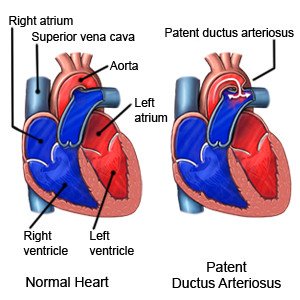
PDA is an abnormal opening between the aorta and the pulmonary artery of your child's heart. In the womb, your baby's blood goes around his or her lungs through a normal opening called a ductus arteriosus (DA). The DA allows your baby to get oxygen from his or her mother's blood. Shortly after birth, the DA closes on its own because blood needs to go to the lungs to get oxygen. When the DA does not close as it should, it is called a patent (open) ductus arteriosus.
 |
What health problems can PDA cause?
A PDA causes some of the blood from the aorta to flow back into the pulmonary artery. This extra blood flow causes the heart to pump harder than normal to send enough blood and oxygen through the body. The increased blood flow could lead to heart failure. It can also increase pressure in your child's lungs.
What causes a PDA?
The cause of PDA is usually not known. PDAs happen more often in premature babies. It also happens more in babies born at high altitudes. Babies born to a mother who had rubella during pregnancy are also more likely to have a PDA.
What are the signs and symptoms of a PDA?
A small PDA may not cause any signs or symptoms. A larger PDA may cause any of the following:
- Heart murmur (abnormal sound heard through stethoscope)
- Shortness of breath after crying, eating, or being active
- Trouble breathing at rest
- Blue lips and fingernails after crying, eating, or being active
- Problems eating and gaining weight
- Colds and lung problems that happen often
How is a PDA diagnosed?
- A chest x-ray of your child's lungs and heart may be taken. Healthcare providers use it to see if the heart chambers are larger than they should be. A chest x-ray can also show if the aorta and the pulmonary arteries have become larger.
- An EKG test records the electrical activity of your child's heart. It is used to check for problems caused by the size of your child's heart.
- An echocardiogram uses sound waves to show pictures of your child's heart on a monitor. This test can show how well your child's heart is pumping. It may also show problems such as fluid around the heart or problems with the heart valves.
How is a PDA treated?
Your child's PDA may not need treatment if it is small and is not causing symptoms. Your child's healthcare provider may wait to see if the PDA will close on its own. The provider may close the PDA even if your child has no symptoms. This helps decrease the risk for infection. Your child may need any of the following:
- Medicine, such as heart medicine or diuretics, may be given if your infant or older child has heart failure.
- Transcatheter duct occlusion may be used to close your child's PDA if it is small. One or more tiny coils are put into the PDA to close it. This treatment is usually used for older infants and children.
- Surgery may be needed for infants and older children. Surgery will be done if the PDA is large and your child is having heart or lung problems.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When should I seek immediate care?
- Your child has shortness of breath after crying, eating, or being active.
- Your child's lips and fingernails turn blue after being active.
When should I call my child's doctor?
- Your child has problems eating and gaining weight.
- Your child has a fever.
- Your child has chills, a cough, or feels weak and achy.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Patent Ductus Arteriosus
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
