Hypertension during Pregnancy
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
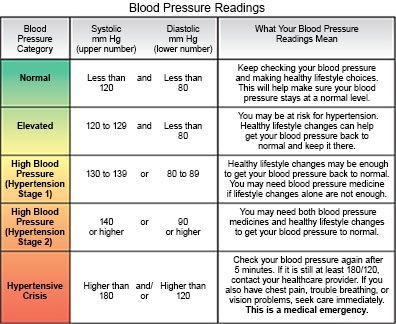
Hypertension is high blood pressure (BP). Normal BP is 119/79 or lower. Hypertension during pregnancy is a BP of 140/90 or higher. Severe hypertension is 160/110 or higher. One or both numbers of these readings may be high. Hypertension may start before you become pregnant, or develop during pregnancy. Pregnancy can cause high BP, or it may develop because of other risk factors you had before you became pregnant. It is important to get screened and treated for an elevated BP or hypertension during pregnancy. This can prevent problems for you and your baby.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US), or have someone else call if:
- You have a seizure.
- You have chest pain.
- You faint or lose consciousness.
- You have trouble breathing.
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
Seek care immediately if:
- You have a severe headache or vision loss.
- You have weakness in an arm or leg.
- You urinate less than usual or stop urinating.
- You have fluid or blood leaking from your vagina that does not stop.
- You feel a gush of fluid from your vagina.
- You have severe abdominal pain with or without nausea and vomiting.
- You feel a change in your baby's movement, or you feel fewer than 6 to 10 movements in an hour.
Call your doctor or obstetrician if:
- You have new or increased swelling in your face or hands, or sudden weight gain.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Medicine may be given to lower your BP. The dose of current BP medicine you take may be changed.
- Daily low-dose aspirin may be recommended if you are at high risk for preeclampsia. Aspirin may help prevent preeclampsia or problems it can cause. Do not take aspirin unless directed by your healthcare provider.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Manage hypertension during pregnancy:
- Go to all scheduled appointments. Your healthcare providers will check your blood pressure and may order other tests.
- Rest as directed. Your healthcare provider may tell you to rest more often if you have mild symptoms of preeclampsia.
- Check your BP as directed if you have chronic hypertension. Sit and rest for 5 minutes before you take your BP. Extend your arm and support it on a flat surface. Your arm should be at the same level as your heart. Follow the directions that came with your BP monitor. Take your BP as often as directed. Keep a record of your BP readings and bring it to your follow-up visits.

- Do not drink alcohol or smoke. Alcohol, nicotine, and other chemicals in cigarettes and cigars can increase your BP. They can also harm your baby. Ask your healthcare provider for information if you currently drink alcohol or smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Eat healthy foods. Healthy foods can help control your BP. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask if you need to be on a special diet.

- Exercise if directed. Exercise can help lower your BP. Ask your healthcare provider how much exercise you need and which exercise is right for you.
- Do kick counts as directed. You may need to keep track of how often your baby moves or kicks over a certain amount of time. Ask your obstetrician how to do kick counts and how often to do them.
- Check your weight each day. Weigh yourself every day before breakfast. Weight gain can be a sign of extra fluid in your body.
Follow up with your doctor or obstetrician as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
