External Fixation of an Ankle Fracture
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about external fixation of an ankle fracture?
External fixation of an ankle fracture is surgery to repair your broken ankle. Fixation means the bones will be held in the correct position with medical hardware, such as pins and screws.
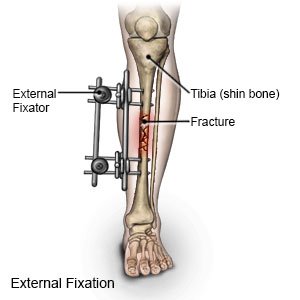 |
How do I prepare for surgery?
- Your surgeon will tell you how to prepare for surgery. He or she may tell you not to eat or drink anything after midnight on the day of your surgery. Arrange to have someone drive you home from surgery.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon about all your allergies, including allergies to medicines or anesthesia.
- You may need to have blood and urine tests before surgery. You may also need x-rays, a CT scan, or an MRI of your ankle and foot.
What will happen during surgery?
- General anesthesia will keep you asleep and free from pain during surgery. Your healthcare provider will move the broken bones back into the correct position. He or she will try to do this without making an incision on your skin. He or she may have to make small incisions for bones that are hard to reach. A fluoroscope (x-ray) may be used to help your surgeon insert pins and correctly align the bones.
- Your surgeon will use a drill to make holes in your bone above and below the fracture. Screws and long metal pins will be inserted through the holes to keep the bones in the correct position. The pins will stick out through your skin. Other rods and devices will be attached to them. An x-ray may be done to see if the bones were set in the right way. Bandages will be wrapped around the areas where pins were inserted.
What should I expect after surgery?
You will be taken to a room to rest until you are fully awake. You will be monitored closely for any problems. Do not get out of bed until your healthcare provider says it is okay. You will then be able to go home or be taken to your hospital room.
- Bandages keep the area clean and dry to prevent infection. A healthcare provider may remove the bandages soon after your surgery to check your wound.
- Medicines may be given to relieve pain or nausea, or to prevent an infection caused by bacteria.
What are the risks of external fixation surgery?
You may develop an infection. Other parts of your ankle and foot, such as nerves, blood vessels, ligaments, muscles, and bones, may be damaged. Your leg, ankle, or foot may become stiff, numb, and weak. Even after surgery, you may still have ankle pain or problems moving your leg or foot. You may have trouble going back to your usual activities, such as sports.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
