Covid-19 and Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
Coronavirus disease 2019 (COVID-19) and children:
COVID-19 illness tends to be more mild in children, but anyone can develop severe illness. Babies younger than 1 year and all children with underlying conditions are at increased risk for severe illness. Even if symptoms do not develop, a baby or child can pass the virus to others.
Common symptoms include the following:
Children's symptoms usually last for about 24 hours.
- The following are the most common symptoms:
- Fever, runny nose
- Shortness of breath, cough
- Vomiting and diarrhea
- The following may also happen:
- Being more tired than usual
- Headache, body aches, or muscle aches
- Abdomen pain, or little or no appetite
- A sudden loss of taste or smell
Call your local emergency number (911 in the US) if:
- Your child is having trouble breathing.
- Your child has pain or pressure in his or her chest.
- Your child seems confused.
- You have trouble waking your child, or he or she cannot stay awake.
- Your child's lips or face look blue.
- Your child's abdominal pain becomes severe.
Call your child's doctor if:
- Your child has a fever.
- Your child has any signs or symptoms of MIS-C.
- Your child's symptoms get worse.
- You have questions or concerns about your child's condition or care.
What you need to know about multisymptom inflammatory syndrome in children (MIS-C):
- MIS-C is a condition that causes inflammation in your child's organs. MIS-C has developed in some children who were infected or were around someone who was. The cause of MIS-C is not known.
- The following are common signs and symptoms of MIS-C:
- A fever
- Abdominal pain, vomiting, or diarrhea
- Neck pain
- A skin rash or bloodshot eyes (whites of the eyes are reddish)
- Being severely tired all the time
- MIS-C usually needs to be treated in the hospital. Your child may need blood tests, a chest x-ray, or an ultrasound to check for signs of inflammation. He or she may be given extra fluid. Medicines may be given to reduce inflammation or other symptoms. Your child may need to stay in the pediatric intensive care unit (PICU) if MIS-C becomes severe.
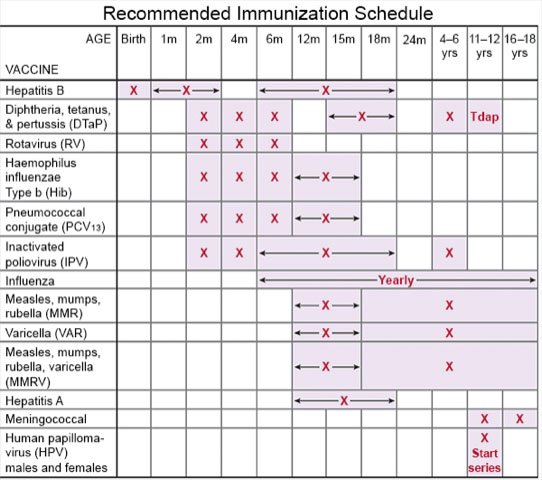
What you need to know about COVID-19 vaccines:
Healthcare providers recommend a COVID-19 vaccine, even if your child has already had COVID-19. Let your child's healthcare provider know when your child has received the final dose of the vaccine. Make a copy of the vaccination card.
- A COVID-19 vaccine is given to children as a shot in 1 to 3 doses. At least 1 dose of an updated vaccine is recommended for all children 6 months or older. COVID-19 vaccines are updated throughout the year. Your child's healthcare provider can help you schedule all needed doses as updated vaccines become available.
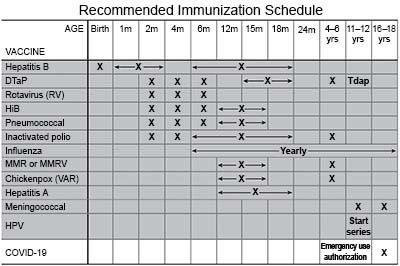
- Ask if a COVID-19 vaccine is required before your child can attend school or daycare. This may vary by state or other local area.
Help stop the spread of COVID-19 and keep your child safe:
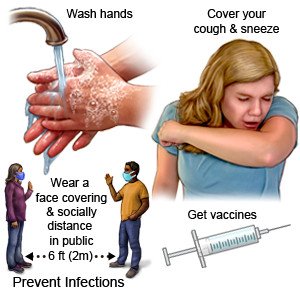 |
- Have your child wash his or her hands often. Have him or her use soap and water. Wash your child's hands for him or her if needed. Teach your child how to wash his or her hands properly. Your child should rub his or her soapy hands together and lace the fingers. Wash the front and back of each hand, and in between all fingers. Use the fingers of one hand to scrub under the fingernails of the other hand. Wash for at least 20 seconds. Teach your child a 20 second song to sing while handwashing. Rinse with warm, running water for several seconds. Then have your child dry with a clean towel or paper towel. Use hand sanitizer that contains alcohol if soap and water are not available. Tell your child not to touch his or her eyes, mouth, or face unless hands are clean. This may be more difficult for younger children.

- Teach your child to cover a sneeze or cough. Have your child turn away from others and cover his or her mouth or nose with a tissue. Throw the tissue away. Your child can use the bend of the arm if a tissue is not available. Then have your child wash his or her hands well with soap and water or use hand sanitizer. Your child should also turn and cover if someone nearby has to sneeze or cough.
- Clean and disinfect high-touch surfaces and objects often. Use disinfecting wipes or a disinfecting solution of 4 teaspoons of bleach in 1 quart (4 cups) of water.
- Ask about medical appointments. Your child may be able to have appointments without having to go into a healthcare provider's office. Some providers offer phone, video, or other types of appointments. Your child will need to go in to receive vaccines. Your child's provider can tell you which vaccines your child needs and when to get them.
What to do if your child is sick:
- Try to keep your child away from others in your home while he or she is sick. Distance may help keep others in the house from getting sick. Keep sick children away from older adults and others who have underlying conditions such as diabetes and heart disease.
- Give your child more liquids as directed. A fever makes your child sweat. This can increase his or her risk for dehydration. Liquids can help prevent dehydration.
- Help your child drink at least 6 to 8 eight-ounce cups of clear liquids each day. Give your child water, juice, or broth. Do not give sports drinks to babies or toddlers.
- Ask your child's healthcare provider if you should give your child an oral rehydration solution (ORS) to drink. An ORS has the right amounts of water, salts, and sugar your child needs to replace body fluids.
- If you are breastfeeding or feeding your child formula, continue to do so. Your baby may not feel like drinking his or her regular amounts with each feeding. If so, feed him or her smaller amounts more often.
- Give your child medicine as directed.
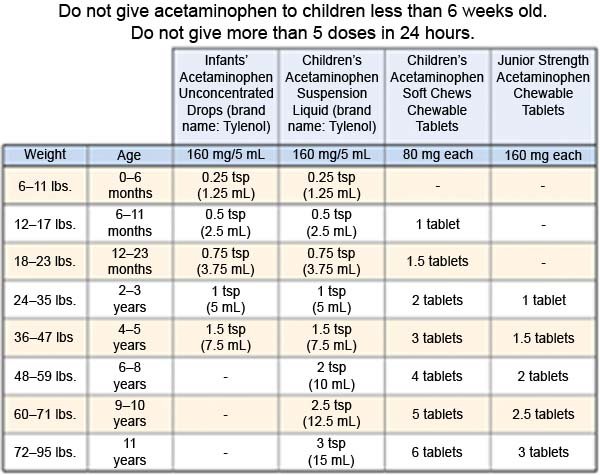
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to give your child and how often to give it. Follow directions. Read the labels of all other medicines your child uses to see if they also contain acetaminophen, or ask your child's doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
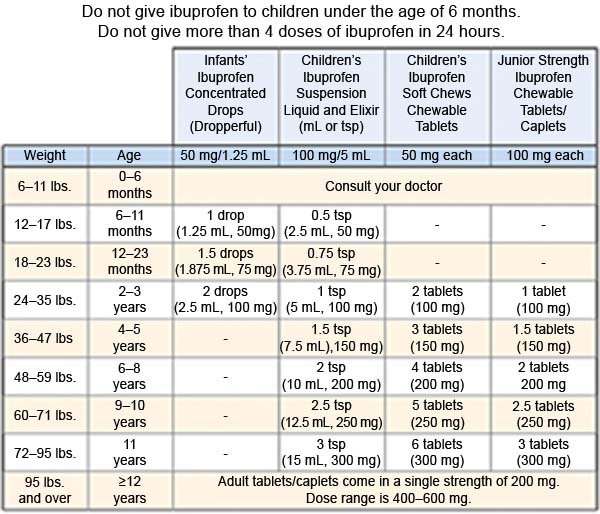
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If your child takes blood thinner medicine, always ask if NSAIDs are safe for him or her. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Follow directions for when your child can be around others after he or she recovers. Your child will need to wait at least 5 days after symptoms first appeared. Then he or she will need to have no fever for 24 hours without fever medicine, and no other symptoms. A loss of taste or smell may continue for several months. It is considered okay to be around others if this is your child's only symptom. It is not known for sure if or for how long a recovered person can pass the virus to others. Your child may need to continue social distancing or wearing a face covering around others for a time.
Follow up with your child's doctor as directed:
Write down your questions so you remember to ask them during your visits.
For more information:
- Centers for Disease Control and Prevention
1600 Clifton Road
Atlanta , GA 30333
Phone: 1- 800 - 232-4636
Web Address: http://www.cdc.gov
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
