Cleft Lip and Cleft Palate Repair
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about cleft lip or cleft palate repair:
Cleft lip and cleft palate repair is surgery to close the openings in your child's lip or mouth. Your child may have a cleft lip repair, a cleft palate repair, or both.
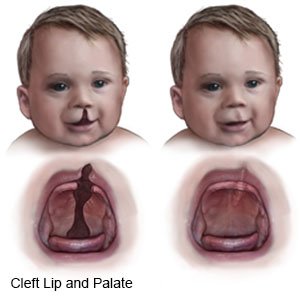 |
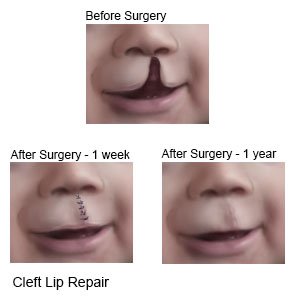 |
What you can do to help your child before surgery:
- Show your child the padded arm boards that will be used after surgery. Explain that they are to keep him or her from touching his or her mouth by accident. Put the padded arm boards on your child for a short time. This will help your child be less afraid if the boards are put on after surgery.
- Teach your child to drink from a cup, the side of a spoon, or a syringe. This may help prepare your child for new ways to drink after surgery.
- Practice cleaning your child's mouth. Sit your child up with his or her head forward. Gently spray water or salt water on the roof of your child's mouth with a spray bottle as directed. Let your child hold the spray bottle so he or she will not be afraid.
How to prepare your child for surgery:
- Your child's healthcare provider will tell you how to prepare your child for surgery. The provider may tell you not to let your child have anything to eat or drink the night before surgery.
- Ask your child's healthcare provider before you give your child any medicine on the day of surgery. These medicines include insulin, antibiotics, over-the-counter medicines, vitamins, or prescription medicines.
- Your child may be given antibiotics to prevent an infection. Medicine may be given in your child's IV to help him or her feel relaxed or drowsy. Your child will also be given general anesthesia to keep him or her asleep during surgery. Tell the healthcare provider if your child has ever had an allergic reaction to antibiotics or anesthesia.
What will happen during surgery:
The surgeon will cut along each side of the cleft. Tissue from both sides of the cleft will be brought together to close the hole. The edges are sewn together with stitches. These will help the wound stay closed as the cleft heals. If your child's cleft involves his or her nose, the nostril may be reshaped at this time or in a later surgery.
What to expect after surgery:
- Your child may have some pain or discomfort when he or she swallows. He or she may be given pain medicine.
- You will be shown how to clean the stitches. You will need to clean the stitches as directed when your child goes home from the hospital. Padded arm bands will be placed on your child. They keep your child from bending his or her elbows. This will prevent your child from touching the stitches. The arm bands will stay on for about 10 days after surgery.
- Your child will stay in the hospital overnight or until he or she can drink liquids again.
Risks of surgery:
Your child may bleed more than usual or get an infection after surgery. He or she may have trouble breathing or get blood clots. Your child can damage the incision by putting his or her hands or an object into his or her mouth. If your child's skin separates from the stitches, surgery may have to be done again. This may also cause more scarring. The most common problem with cleft lip repair is when the side of the repaired lip does not line up with the other side. The most common problem with cleft palate repair is poor healing. It is common for children with clefts to need repair surgery more than 1 time.
Seek care immediately if:
- Your child's stitches come apart.
- Your child's stitches are red, swollen, or draining pus.
- Your child has severe pain.
- Your child will not eat or drink.
- Your child cries without tears.
- Your child's lips, mouth, and tongue are very dry.
- Your child's eyes look sunken in.
- Your baby's fontanelle (soft spot on the top of the head) is sunken.
- Your child urinates very little or none at all.
Call your child's doctor or surgeon if:
- Your child has a fever.
- Your child has chills, a cough, or sounds congested.
- You feel overwhelmed and need help to feed your child.
- Your child does not eat as well as he or she usually does.
- Your child acts tired, sleepy, restless, or fussy.
- Your child has a fever, ear pain, and trouble hearing.
- You have questions or concerns about your child's condition or care.
Medicines:
Your child may need any of the following:
- Antibiotics may be given to fight an infection caused by bacteria.
- Prescription pain medicine may be given. Ask your child's healthcare provider how to give this medicine safely. Some prescription pain medicines contain acetaminophen. Do not give your child other medicines that contain acetaminophen without talking to a healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your child's healthcare provider how to prevent or treat constipation.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Give your child's medicine as directed. Contact your child's healthcare provider if you think the medicine is not working as expected. Tell the provider if your child is allergic to any medicine. Keep a current list of the medicines, vitamins, and herbs your child takes. Include the amounts, and when, how, and why they are taken. Bring the list or the medicines in their containers to follow-up visits. Carry your child's medicine list with you in case of an emergency.
How to feed your child:
Feeding your child can be difficult. Try to be calm and patient. This will help your child relax as he or she eats. Teach others how to feed your child. This will give you support and help you manage stress. The following tips will help you feed your child:
- Breastfeeding helps your child suck better because your breast fills the cleft. Breastfeeding also decreases your child's risk of ear infections and helps strengthen the muscles he or she uses to eat.
- Your child may need to use a bottle if he or she cannot breastfeed. Healthcare providers will work with you to find the best bottles, nipples, and other supplies to feed your child. Ask providers about bottles and nipples made for children who have a cleft. If you cannot find these supplies, look for nipples with wide openings or a cross cut into the nipple. These nipples will help your child get more milk with each suck. You can also use squeeze bottles to help get the milk into your child's mouth. These supplies may help decrease your child's risk of choking.
- Feed your child in an upright position. His or her head should be higher than the stomach. This will help prevent choking. It will also help keep liquids from coming out of your child's nose or going into his or her ears.
- Feed your child slowly over 18 to 30 minutes. Burp him or her after every 1 to 2 ounces of liquid to decrease the amount of air swallowed.
- Do not overfeed your baby. Your baby will give you clues of when he or she is done. Your baby may look around instead of watching you. He or she may chew on the nipple rather than sucking on it. He or she may also cry and try to wriggle away.
- Do not lay your child down with a bottle. This may increase the risk of choking, ear infections, and cavities.
Speech and nutrition therapy:
Your child may need therapy to help with his or her speech. You may also need to meet with a dietitian to learn the best foods for your child.
Protect your child's incisions:
Your child's mouth needs to be protected for 6 weeks after surgery. It may take this long for your child's mouth to heal. If the stitches are not protected, they could pull or break. This may cause more bleeding, pain, or scarring for your child. Your child may need another surgery if the stitches separate. It is important to watch your child at all times to prevent this from happening.
- Do not let your child put his or her hands or objects into his or her mouth. Padded arm boards can be used to keep your child's elbows straight. This will help keep your child from rubbing his or her face with his or her hands or upper arms. Long sleeves should be worn under the arm boards to keep them from rubbing on your child's skin. Remove the arm boards 3 to 4 times a day so your child's arms can get exercise. Do not leave your child alone when the arm boards are off.
- Do not let your child sleep on his or her stomach. Your child should sleep on his or her back or side. This will help prevent your child from rubbing his or her face on the sheets. Dress your child in clothes that snap or button in the front.
Help prevent infection:
- Keep your child away from people with colds, the flu, or other infections until his or her mouth is healed.
- Keep the inside of your child's mouth wet. This will help keep the surgery area clean. Sit your child up with his or her head forward to prevent choking. Gently spray water or salt water on the roof of his or her mouth with a spray bottle as directed. Do this after each feeding and at bedtime.
Follow up with your child's healthcare provider or specialist as directed:
Your child may need to return for more tests. He or she may also need to have his or her weight measured. Write down your questions so you remember to ask them during your visits.
For support and more information:
- Cleft Palate Foundation
1504 E. Franklin St, Ste. 102
Chapel Hill , North Carolina 27514-2820
Phone: 1- 919 - 933-9044
Web Address: http://www.cleftline.org
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
