Cervicitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is cervicitis?
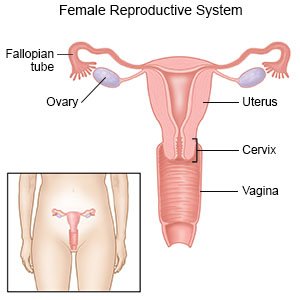
Cervicitis is inflammation of your cervix. Your cervix is at the bottom of your uterus where it opens into your vagina.
 |
What causes or increases my risk for cervicitis?
In some cases, the exact cause of cervicitis may not be clear. Most cases are caused by the following:
- Douching, which causes normal vaginal bacteria to be out of balance
- An infection in your vagina or reproductive organs, or a sexually transmitted infection (STI)
- Chemicals, such as spermicides used to kill sperm, latex in condoms
- Items placed in your vagina, such as a tampon, diaphragm, or cervical cap
- Cancer, or radiation used to treat cancer
- Older age, which causes your estrogen levels decrease
- Multiple sex partners or unprotected sex
What are the signs and symptoms of cervicitis?
You may have no signs and symptoms, or you may have any of the following:
- Vaginal itching
- Vaginal bleeding or spotting in between your monthly periods or during or after sex
- Green or yellow vaginal discharge that may smell foul
- Pain during or after sex
- Pain with urination
- Abdominal pain
- Fever
How is cervicitis diagnosed?
Your healthcare provider may ask about your health and sex history. Tell your provider about your symptoms and when they started. Tell him or her about any STIs that you or your partner have or have had. Your provider will do a pelvic exam to check your vagina and cervix. You may also need any of the following:
- Blood or urine tests may be done to check for an infection. The tests may show which germ is causing the infection.
- A vaginal fluid culture is a sample of discharge from your vagina or cervix. The sample is sent to a lab to be tested.
How is cervicitis treated?
- Antibiotics helps kill bacteria causing cervicitis. Take them as directed.
- An ablation may be used to treat cervicitis that continues or comes back after treatment. Your healthcare provider may freeze, burn, or scrape the top layer of skin from your cervix.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I prevent cervicitis?
- Get treatment before you continue having sex. Your risk for an STI is lower if you have fewer sex partners. If you have an STI, tell all recent sex partners. Tell them to see a healthcare provider for testing and treatment to help stop the spread of infection. Do not have sex with someone who has or is being treated for an STI.
- Use a condom during sex. Use a latex condom every time you have sex. If you are allergic to latex, use a nonlatex condom.
- Do not use products that can cause irritation. Do not douche unless healthcare providers tell you to. Do not use spermicides if they caused symptoms in the past. Use sanitary napkins instead of tampons.
Where can I find more information?
- Centers for Disease Control and Prevention
1600 Clifton Road
Atlanta , GA 30333
Phone: 1- 800 - 232-4636
Web Address: http://www.cdc.gov
When should I seek immediate care?
- You have bleeding from your vagina that does not stop and it is not time for your period.
When should I call my doctor or gynecologist?
- You are spotting blood from your vagina and it is not time for your period.
- You have yellow or green discharge from your vagina.
- You have abdominal pain.
- You have a fever.
- You think or know you are pregnant.
- Your symptoms do not go away 2 to 4 weeks after you start treatment.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Cervicitis
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
