Cardiac Tamponade
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is cardiac tamponade?
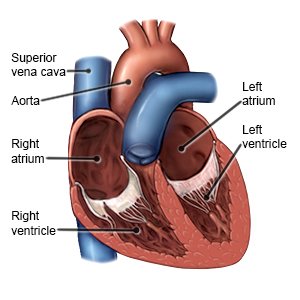
Cardiac tamponade occurs when too much fluid collects in the pericardium (the sac around your heart). The fluid puts pressure on your heart. This makes it difficult for your heart to pump. Fluid may collect slowly or quickly. Cardiac tamponade can become life-threatening.
 |
What increases my risk for cardiac tamponade?
- Infection or inflammation
- Hypothyroidism
- Lymphoma, breast cancer, or lung cancer
- Heart or abdominal surgery
- Recent heart attack or dissection (tear) in the aorta
- Kidney failure or congestive heart failure
What are the signs and symptoms of cardiac tamponade?
- Chest pain, or chest discomfort that may improve when you sit up
- Shortness of breath
- Weakness, lightheadedness, or fainting
- Pounding or racing heartbeat
- Bulging veins in your neck, head, or temples
- Nausea or abdominal pain
How is cardiac tamponade diagnosed?
- Blood tests are done to find the cause of your symptoms. They are also used to check for infection or get information about your overall health.
- An EKG test records your heart rhythm and how fast your heart beats. It is used to check the electrical activity of your heart to see if it is damaged.
- An echocardiogram is a type of ultrasound. Sound waves are used to check for fluid around your heart.
- An x-ray, CT scan, or MRI help show if there is fluid around your heart. You may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- Pulmonary artery catheterization measures the pressure in your pulmonary arteries. It shows how well your heart is working.
How is cardiac tamponade treated?
Treatment is based on how severe your symptoms are and what is causing the cardiac tamponade. You may need any of the following:
- Pericardial drainage relieves pressure on your heart so it can pump normally. A catheter is inserted into the pericardium to drain fluid.
- IV fluids may be given if your blood pressure is too low.
- Medicines help your heart pump and improve blood flow to your body.
- Surgery may be needed to relieve pressure on your heart. An incision is made into your chest and into the pericardium to drain fluid.
Call your local emergency number (911 in the US) if:
- You have sudden chest pain.
- You have sudden trouble breathing.
When should I seek immediate care?
- Your heart is pounding or racing.
When should I call my doctor?
- You have new or worsening swelling in your ankles, legs, or abdomen.
- You have bulging veins in your neck, head, or temples.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
