Aortic Regurgitation
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is aortic regurgitation?
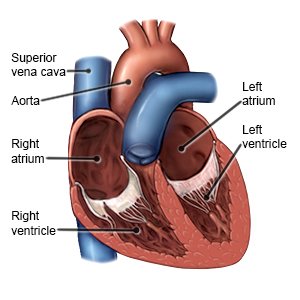
Aortic regurgitation is a condition that causes blood to flow through the aortic valve to your left ventricle. This happens because the aortic valve does not close properly. The aortic valve is between the left ventricle and the aorta. The aorta is a blood vessel that pumps blood to your body. The aortic valve opens and closes to direct blood from your left ventricle to your aorta.
 |
What increases my risk for aortic regurgitation?
Aortic regurgitation is caused by damage to or weakness of the aortic valve. Any of the following may increase your risk for these problems:
- Older age
- Being born with heart problems
- Rheumatic fever or infection of the aortic valve
- High blood pressure or heart attack
- Injury to the aortic valve from trauma, a heart procedure, or radiation
- A medical condition such as Marfan syndrome
- Certain medicines, such as pills that help you lose weight
What are the signs and symptoms of aortic regurgitation?
You may not have symptoms, or you may have any of the following:
- Weakness or fatigue
- Shortness of breath that gets worse during activity or when you lie down
- Chest pain or tightness
- Dizziness or feeling faint
- A fast heartbeat or feeling your heart flutter
- Swollen feet or ankles
How is aortic regurgitation diagnosed?
Your healthcare provider will examine you and listen to your heart. He or she will ask if you have had strep throat or rheumatic fever. Tell your provider if you have a family history of heart disease. You may need any of the following tests:
- Blood tests may be used to check for an infection or other cause of your aortic regurgitation.
- An echocardiogram is a type of ultrasound. It is used to show problems with your aortic valve and how blood flows through your heart. It may also show how well your heart is pumping. You may need a transthoracic or transesophageal echocardiogram. Ask your healthcare provider about these types of echocardiogram.
- X-ray, CT, or MRI pictures show the size of your heart and look for fluid around your heart or lungs. They also look for problems with your valve or aorta. You may be given contrast liquid to help the heart and lungs show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- An EKG test records the electrical activity of your heart. It is used to check for an abnormal heart rhythm.
- A stress test helps healthcare providers see how well your aortic valve works under stress. Healthcare providers may place stress on your aortic valve with exercise or medicine.
- Cardiac catheterization is a procedure to check how well your heart is pumping blood. It is also used to measure pressure in different parts of your heart. A catheter (long thin tube) is inserted into your arm, neck, or groin and moved into your heart. An x-ray may be used to guide the tube to the right place. Contrast liquid may be used to help your heart show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
How is aortic regurgitation treated?
Treatment may not be needed if your condition does not cause symptoms.
- Medicine may be given to lower your blood pressure, decrease stress on your heart, or remove extra fluid.
- Surgery may be used to repair or replace your aortic valve if you have severe symptoms.
How can I manage aortic regurgitation?
- Maintain a healthy weight. Being overweight can increase your risk for high blood pressure and coronary artery disease. These conditions can make your heart work harder. Ask your healthcare provider what a healthy weight is for you. Ask him or her to help you create a weight loss plan if you are overweight.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung and heart damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Limit or do not drink alcohol. Ask your healthcare provider if it is okay for you to drink alcohol. Alcohol can increase your risk for high blood pressure and coronary artery disease. Your provider can tell you how many drinks are okay to have within 24 hours or within 1 week. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
- Eat heart-healthy foods. Heart-healthy foods include salmon, tuna, walnuts, whole-grain breads, low-fat dairy products, beans, and oils such as olive or canola oil. A dietitian or your provider can give you more information on meal plans such as the DASH (Dietary Approaches to Stop Hypertension) eating plan. The DASH plan is low in sodium, processed sugar, unhealthy fats, and total fat. It is high in potassium, calcium, and fiber. These can be found in vegetables, fruit, and whole-grain foods.

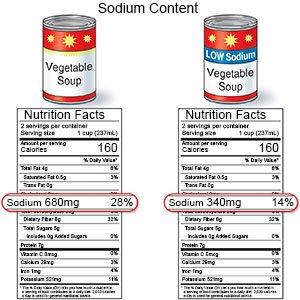
- Limit sodium (salt) as directed. Too much sodium can affect your fluid balance. Check labels to find low-sodium or no-salt-added foods. You can also make small changes to get less salt. For example, if you add salt while you cook, do not add more salt at the table. Ask your healthcare provider or dietitian for more ways to cut down on salt.
- Exercise as directed. Exercise can help keep your heart healthy. Ask your healthcare provider what activities are safe for you to do. The amount and type of exercise that is safe may depend on how severe your condition is.
- Talk to your healthcare provider about pregnancy. If you are a woman and want to get pregnant, talk to your healthcare provider. You and your baby may need to be monitored by specialists during your pregnancy.
- Ask your healthcare provider if you should take antibiotics before certain procedures. Some procedures may allow bacteria to get into your blood and travel to your heart. This can make your condition worse.
- Ask about vaccines you may need. Certain diseases are dangerous for a person who has aortic regurgitation. Vaccines help prevent infections that can cause some diseases. Get a flu vaccine as soon as recommended each year, usually in September or October. Your healthcare provider can tell you if you also need other vaccines, and when to get them.
What can I do to prevent aortic regurgitation?
- Manage other health conditions. High blood pressure and high cholesterol levels increase your risk for aortic regurgitation. Ask your healthcare provider for more information on managing these conditions.
- Get treatment for strep throat. If strep throat is not treated, it can cause rheumatic fever.
- Talk to your healthcare provider before you take any new medicine. Some medicines can cause aortic regurgitation.
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
When should I seek immediate care?
- Your heart is beating faster than usual and you feel fluttering in your chest.
- You have new or worse swelling in your abdomen, legs, ankles, or feet.
When should I call my doctor?
- You have a fever.
- You feel more tired than usual.
- You are more short of breath than usual when you exercise or lie down.
- You cough more than usual, especially when you lie down.
- You are pregnant or think you are pregnant.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Aortic Regurgitation
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
