Allergy Testing in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is allergy testing?
Allergy testing is a way to find out if your child is allergic to something, called an allergen. Common allergens include pet dander, pollen, insect bites or stings, and certain foods, such as peanuts. Your child's healthcare provider will use an allergy test to check for a reaction to the allergen. During the test, your child's provider will watch for small skin reactions that show your child is probably allergic. The provider will also watch for a rare but serious reaction called anaphylaxis that needs immediate treatment.
How do I prepare my child for an allergy test?
- Your child may be afraid that the test will hurt. Depending on your child's age, it may be helpful to explain the test before it happens. Tell your child why this test is needed and what will happen during the test. Explain that your child might be uncomfortable or feel itchy during the test. Also explain that medicine may help with any itchiness when the test is over.
- Talk to your child's healthcare provider about all medicines your child takes. Some medicines may keep the allergy test from working correctly. Your child may need to stop taking certain medicines days, weeks, or months before the test. Examples include antihistamines, topical steroids, and medicines to stop vertigo or relieve insomnia. Your child's provider will tell you if your child needs to stop any medicine, and when to stop it. The provider will also tell you when your child can start taking the medicine again after the allergy test.
What are the different kinds of allergy tests?
- A skin prick test is used to check for a reaction to an allergen applied to your child's skin. Your child's healthcare provider will place drops of solution on your child's skin. This is usually applied on the upper back in children. Each drop will contain a small amount of 1 possible allergen. Your child's provider will then prick or scratch the skin under the drops. This will help the solution get into your child's skin. If the skin becomes raised, red, and itchy within 20 minutes, your child may be allergic to that allergen.
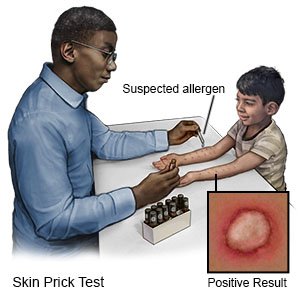
- An intradermal test is used to check for a reaction to an allergen injected under the skin of your child's upper arm. This may be used if your child's skin does not react during a skin prick test but your child may still be allergic to an allergen. The provider will inject the allergen under your child's skin and check for a reaction in about 15 minutes. Your child may be allergic to that allergen if the skin becomes raised, red, and itchy within 20 minutes.
- A patch test is used to check for a reaction to an allergen taped to your child's skin. The allergen is put onto a pad. The pad is taped to the skin. Your child will then come back in 3 days and have the area checked for a reaction. Your child will come back again at day 5 to 7 to have it checked again. Your child's provider will wait 15 to 60 minutes after removing the pad to check for a reaction. This is because your child may have some skin irritation from where the pad was taped to the skin. The irritation can be mistaken for an allergic reaction. Your child cannot get the patch test area wet during this test.
- A blood test may be used in children who have certain rashes or take medicine that make skin testing difficult to do. Blood tests may be used for children who are at risk for anaphylaxis during other kinds of allergy testing. Anaphylaxis is a life-threatening reaction to an allergen. A sample of your child's blood is tested to see if it contains antibodies to specific allergens.
What should I expect after my child's allergy test?
- You and your child's healthcare provider will talk about the results of the allergy test. A positive test result means your child's skin showed signs of an allergic reaction to an allergen. You and your child's provider can talk about other tests your child may need. The tests can find how severe the allergy is and if your child may need medicine to prevent or control a reaction. This is called an action plan.
- Rarely, after a prick or intradermal test, your child may develop signs of an allergic reaction. Depending on the kind of test your child had, you and your child will need to watch for signs of an allergic reaction. This can happen within hours of an allergy test. Your child's provider will tell you what to do if your child has a reaction. Your child may need to take an antihistamine or other medicine to stop the reaction.
Call your local emergency number (911 in the US) if:
- Your child has any of the following signs or symptoms of anaphylaxis:
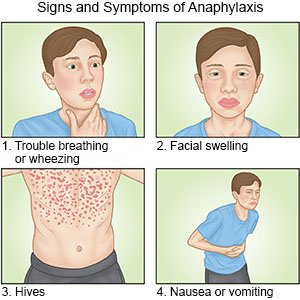
- Itching, a rash, hives that spread over the body
- Trouble breathing, swelling in the mouth or throat, or wheezing
- Feeling faint
When should I seek immediate care?
- Your child has new or worsening rashes, hives, or itching.
When should I call my child's doctor?
- Your child has an upset stomach or is vomiting.
- Your child has stomach cramps or diarrhea.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
