Pain Management in Older Adults
Medically reviewed by Drugs.com. Last updated on May 4, 2025.
What do I need to know about pain in older adults?
Pain is not a normal part of aging and may be a sign that something is wrong. Sometimes the cause of pain is not clear. Pain management is an important part of your care. It can increase your appetite, sleep, and energy. It can also improve your mood and your relationships.
What are the types of pain?
- Acute pain may be caused by an illness or injury. It comes on suddenly and lasts a short period of time. Acute pain usually goes away as your body heals but may become chronic if left untreated.
- Chronic pain describes pain that continues or gets worse over a long period of time. It may last for months or years. It may be pain that remains after you have recovered from an injury. Diseases such as cancer, arthritis, migraines, and back problems are also common causes of chronic pain.
How will healthcare providers know if I am in pain?
You may have many questions and fears about pain. Do not be ashamed to tell your providers about what you are feeling. Tell them where you hurt and how bad it is. You may try to deny that you are having pain to show courage or to escape treatment. Conditions such as dementia (memory problem), brain damage, or a stroke may make it hard to express pain. The following are common signs that may tell providers that you are in pain:
- Crying, moaning, frowning, or sighing
- Frequent feelings of sadness, depression, hopelessness, aggression, or anger
- Noisy breathing, or calling out
- Not moving, or staying in one position to decrease pain
- Poor appetite, or changes to usual sleep patterns
- Pulling away or getting upset when touched
- Restlessness or pacing
How is the cause of pain diagnosed?
Your healthcare provider will examine you and look for painful areas. Your provider may touch or press different places on your body and ask about your pain. Your provider may ask you to describe your pain. Tell your provider if your pain is sharp, dull, or achy. Tell your provider if you have constant pain or if it comes and goes. You may also need any of the following to check how much pain you have or to find its cause:
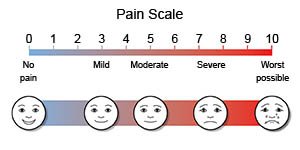
- Pain scales may help measure how much pain you feel. Pain scales may include numbers or faces. Your provider may ask you to rate the pain on a scale from 0 to 10.
- An x-ray, CT, or MRI may be used to find the cause of your pain. You may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- Stimulation tests may help find nerves or muscles affected by pain.
Drugs used to treat this and similar conditions
Hydrocodone
Hydrocodone (Hysingla ER and Zohydro ER) is used for around-the-clock treatment of severe pain ...
Cymbalta
Cymbalta (duloxetine) is used to treat major depressive disorder, general anxiety disorder and ...
Ozempic
Learn about Ozempic (semaglutide) for type 2 diabetes treatment, weight management, cardiovascular ...
Oxycodone
Oxycodone is an opioid analgesic used to treat moderate to severe pain; it has a high potential for ...
Tylenol
Tylenol is a pain reliever and a fever reducer used to treat many conditions such as headaches ...
Acetaminophen
Acetaminophen is a widely used pain reliever and fever reducer for conditions like headaches ...
Ibuprofen
Ibuprofen (Advil, Motrin) treats minor aches and pains caused by the common cold, headaches ...
Gabapentin
Gabapentin is an anti-epileptic drug, also called an anticonvulsant. It is used to treat some types ...
Acetaminophen/hydrocodone
The combination of hydrocodone and acetaminophen is used to relieve moderate to severe pain ...
Paracetamol
Paracetamol (Panadol, Calpol, Alvedon) is a widely used over-the-counter painkiller and fever ...
Which medicines are used to treat pain?
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Prescription pain medicines such as opioids, or narcotics, are only used for short-term (acute) pain. Your healthcare provider will tell you how to take your specific prescription pain medicine safely. Your provider will tell you about common and serious side effects of the medicine and what to do if they happen. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your provider.
- Steroids decrease inflammation that causes pain.
- Anesthetic medicines may be injected in or around a nerve to block pain signals from the nerves.
- Anxiety medicine decreases anxiety. High levels of anxiety make pain harder to manage.
- Antidepressants may be used to help decrease or prevent the symptoms of depression or anxiety. They are also used to treat nerve pain.
What do I need to know about prescription pain medicine safety?
Your healthcare provider will give you specific instructions based on the medicine you are taking. The following are general guidelines:
- Take your medicine as directed. Take only the amount prescribed or recommended. If you use a pain patch, remove the old patch before you place a new one. Ask your provider before you stop taking prescription pain medicine you have been taking for longer than 2 weeks. A sudden stop may cause dangerous side effects. Your provider will give you instructions for how to dispose of prescription pain medicine safely.
- Follow safety guidelines. Some medicines can cause drowsiness, slowed breathing, or concentration problems. Do not drink alcohol, drive, or operate heavy machines while you use prescription medicines. Take pain medicine 30 minutes before exercise or physical therapy, or as directed.
- Watch for side effects. Some foods, alcohol, and other medicines may cause side effects when combined with pain medicine. Ask your provider how to prevent these problems.
What can I do to manage pain without medicine?
- Keep a pain diary to help you track pain cycles. Include anything that makes your pain worse or better. Bring your pain diary when you follow up with your healthcare provider or pain specialist.
- Apply heat or ice as directed. Heat and ice relieve pain. Heat also relieves muscle spasms. Your provider may recommend only heat or ice, or you may be told to alternate. For heat, use a heat pack, heating pad set on low, or a warm washcloth. Apply heat for 20 to 30 minutes every 2 hours for as many days as directed. For ice, use an ice pack, or put crushed ice in a plastic bag. Cover the bag with a towel before you place it on your skin. Apply ice for 15 to 20 minutes every hour or as directed.
- Exercise as directed. Exercise can help improve movement and strength, and decrease pain. Your provider will help you find exercise programs that are right for your type of pain.

- Go to cognitive behavioral therapy (CBT) as directed. CBT can help you gain control over your pain and how you react to it. Your provider may have you get treatment from a therapist.
- Go to physical therapy (PT) or occupational therapy (OT) as directed. A physical therapist may teach you exercises that can help with your pain. An occupational therapist may teach new ways to do your daily activities so you have less pain.
- Use self-management programs to help you control pain. These programs give you education about pain and the effect it can have on your life. The programs also teach coping techniques, such as relaxation and communication.
- Talk to your provider about your daily activities. Some activities can cause pain to become worse or make pain management less effective. Your provider can help you find ways to reduce pain. For example, you may need to change when you take your pain medicine so it is more effective during activities.
Where can I find more information?
- American Chronic Pain Association
PO Box 850
Rocklin , CA 95677
Phone: 1- 800 - 533-3231
Web Address: https://www.theacpa.org
When should I call my doctor or pain specialist?
- Your pain gets worse or you have new pain.
- You have new symptoms, such as numbness or tingling.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
