Lorvatus Pharmapak: Package Insert / Prescribing Info
Package insert / product label
Generic name: diclofenac sodium, metaxalone, and isopropyl alcohol
Dosage form: kit
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Overdosage
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- How Supplied/Storage and Handling
- Storage and Handling
- Patient Counseling Information
- Warnings
- Precautions
Highlights of Prescribing Information
DICLOFENAC Sodium Topical Solution 1.5% w/w is for topical use only.
Initial U.S. Approval: 1988
WARNING: CARDIOVASCULAR AND GASTROINTESTINAL RISK
See full prescribing information for complete boxed warning
Cardiovascular Risk
- Nonsteroidal anti-inflammatory drugs (NSAIDS) may cause an increased risk of serious cardiovascular thrombotic events, myocardial infarction, and stroke, which can be fatal. Patients with cardiovascular disease or risk factors for cardiovascular disease may be at greater risk. (5.1)
- Diclofenac sodium topical solution is contraindicated for the treatment of perioperative pain in the setting of coronary artery bypass graft (CABG) surgery. (4 )
Gastrointestinal Risk
- NSAIDs, including diclofenac sodium topical solution cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal events. (5.2)
Recent Major Changes
| Dosage and Administration (2) | 10/2013 |
Indications and Usage for Lorvatus Pharmapak
Diclofenac sodium topical solution is a nonsteroidal anti-inflammatory drug (NSAID) indicated for the treatment of signs and symptoms of osteoarthritis of the knee(s). (1)
Lorvatus Pharmapak Dosage and Administration
For the relief of the signs and symptoms of osteoarthritis of the knee(s), the recommended dose is 40 drops on each painful knee, 4 times a day. (2)
- Apply diclofenac sodium topical solution to clean, dry skin. (2.1)
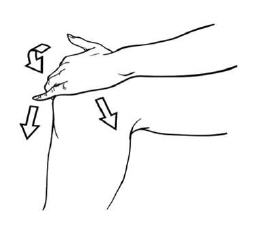
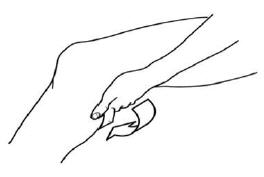
- Dispense diclofenac sodium topical solution 10 drops at a time either directly onto the knee or first into the hand and then onto the knee. Spread diclofenac sodium topical solution evenly around front, back and sides of the knee. Repeat this procedure until 40 drops have been applied and the knee is completely covered with solution. (2.1)
- Wash hands completely after administering the product.
- Wait until the area is completely dry before covering with clothing or applying sunscreen, insect repellent, cosmetics, topical medications, or other substances.
- Do not get diclofenac sodium topical solution in your eyes, nose or mouth.
Dosage Forms and Strengths
- 1.5% w/w topical solution (3)
Contraindications
Warnings and Precautions
- Serious and potentially fatal cardiovascular thrombotic events, myocardial infarction, and stroke can occur with NSAID treatment. Use the lowest effective dose of diclofenac sodium topical solution in patients with known CV disease or risk factors for CV disease. (5.1)
- NSAIDs can cause gastrointestinal (GI) adverse events including inflammation, bleeding, ulceration, and perforation. Prescribe diclofenac sodium topical solution with caution in those with a prior history of ulcer disease or gastrointestinal bleeding. (5.2)
- Elevation of one or more liver tests may occur during therapy with NSAIDs. Discontinue diclofenac sodium topical solution immediately if abnormal liver tests persist or worsen. (5.3)
- Hypertension can occur with NSAID treatment. Monitor blood pressure closely with diclofenac sodium topical solution treatment. (5.4)
- Use diclofenac sodium topical solution with caution in patients with fluid retention or heart failure. (5.5)
- Long-term administration of NSAIDs can result in renal papillary necrosis and other renal injury. Use diclofenac sodium topical solution with caution in patients at greatest risk of this reaction, including the elderly, those with impaired renal function, heart failure, liver dysfunction, and those taking diuretics and ACE-inhibitors. (5.6)
- Anaphylactoid reactions may occur in patients with the aspirin triad or in patients without prior exposure to diclofenac sodium topical solution. (5.7)
- NSAIDs can cause serious skin adverse events such as exfoliative dermatitis, Stevens-Johnson syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. (5.8)
- Not for use during pregnancy. (5.9)
- Do not administer to patients with aspirin sensitive asthma and use with caution in patients with preexisting asthma. (5.10)
- Avoid exposure of treated knee(s) to natural or artificial sunlight. (5.11)
- Avoid contact of diclofenac sodium topical solution with eyes and mucosa. (5.12)
Avoid concurrent use with oral NSAIDs. (5.13)
Adverse Reactions/Side Effects
The most common adverse events with diclofenac sodium topical solution are application site reactions. (6.1)
To report SUSPECTED ADVERSE REACTIONS, contact IGI Laboratories, Inc. at 1-856 -697-1441, or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
- Concomitant administration of diclofenac and aspirin is not generally recommended because of the potential of increased adverse effects including increased GAI bleeding. (7.1)
- Concomitant use of anticoagulants and diclofenac have a risk of serious GI bleeding higher than users of either drug alone. (7.2)
Use In Specific Populations
See 17 for PATIENT COUNSELING INFORMATION.
Revised: 7/2015
Full Prescribing Information
WARNING: CARDIOVASCULAR AND GASTROINTESTINAL RISK
Cardiovascular Risk
- Nonsteroidal anti-inflammatory drugs (NSAIDs) may cause an increased risk of serious cardiovascular thrombotic events, myocardial infarction, and stroke, which can be fatal. This risk may increase with duration of use. Patients with cardiovascular disease or risk factors for cardiovascular disease may be at greater risk [see Warnings and Precautions (5.1)].
- Diclofenac sodium topical solution is contraindicated in the perioperative setting of coronary artery bypass graft (CABG) surgery [see Contraindications (4)].
Gastrointestinal Risk
- NSAIDs cause an increased risk of serious gastrointestinal adverse events including bleeding, ulceration, and perforation of the stomach or intestines, which can be fatal. These events can occur at any time during use and without warning symptoms. Elderly patients are at greater risk for serious gastrointestinal events [see Warnings and Precautions (5.2)].
1. Indications and Usage for Lorvatus Pharmapak
Diclofenac sodium topical solution is a nonsteroidal anti-inflammatory drug (NSAID) indicated for the treatment of signs and symptoms of osteoarthritis of the knee(s).
2. Lorvatus Pharmapak Dosage and Administration
2.1 General Instructions
For the relief of the signs and symptoms of osteoarthritis of the knee(s), the recommended dose is 40 drops per knee, 4 times a day.
Apply diclofenac sodium topical solution to clean, dry skin.
To avoid spillage, dispense diclofenac sodium topical solution 10 drops at a time either directly onto the knee or first into the hand and then onto the knee. Spread diclofenac sodium topical solution evenly around front, back and sides of the knee. Repeat this procedure until 40 drops have been applied and the knee is completely covered with solution.
To treat the other knee, if symptomatic, repeat the procedure.
Application of diclofenac sodium topical solution in an amount exceeding or less than the recommended dose has not been studied and is therefore not recommended.
2.2 Special Precautions
- Avoid showering/bathing for at least 30 minutes after the application of diclofenac sodium topical solution to the treated knee.
- Wash and dry hands after use.
- Do not apply diclofenac sodium topical solution to open wounds.
- Avoid contact of diclofenac sodium topical solution with eyes and mucous membranes. Do not apply external heat and/or occlusive dressings to treated knees.
- Avoid wearing clothing over the diclofenac sodium topical solution-treated knee(s) until the treated knee is dry.
- Protect the treated knee(s) from sunlight.
- Wait until the treated area is dry before applying sunscreen, insect repellant, lotion, moisturizer, cosmetics, or other topical medication to the same knee you have just treated with diclofenac sodium topical solution.
- Until the treated knee(s) is completely dry, avoid skin-to-skin contact between other people and the treated knee(s).
4. Contraindications
Diclofenac sodium topical solution is contraindicated in patients with a known hypersensitivity to diclofenac sodium or any other component of diclofenac sodium topical solution.
Diclofenac sodium topical solution is contraindicated in patients who have experienced asthma, urticaria, or allergic-type reactions after taking aspirin or other NSAIDs. Severe, rarely fatal, anaphylactic-like reactions to NSAIDs have been reported in such patients [see Warnings and Precautions (5.7, 5.10)].
Diclofenac sodium topical solution is contraindicated in the setting of coronary artery bypass graft (CABG) surgery [see Warnings and Precautions (5.1)].
5. Warnings and Precautions
5.1 Cardiovascular Thrombotic Events
Clinical trials of several oral COX-2 selective and nonselective NSAIDs of up to three years duration have shown an increased risk of serious cardiovascular (CV) thrombotic events, myocardial infarction (MI), and stroke, which can be fatal. All NSAIDs, including diclofenac sodium topical solution and COX-2 selective and nonselective orally administered NSAIDs, may have a similar risk. Patients with known CV disease or risk factors for CV disease may be at greater risk. To minimize the potential risk for an adverse CV event in patients treated with an NSAID, use the lowest effective dose for the shortest duration possible. Physicians and patients should remain alert for the development of such events, even in the absence of previous CV symptoms. Inform patients about the signs and/or symptoms of serious CV events and the steps to take if they occur.
Two large, controlled, clinical trials of an orally administered COX-2 selective NSAID for the treatment of pain in the first 10 to 14 days following CABG surgery found an increased incidence of myocardial infarction and stroke [see Contraindications (4)].
There is no consistent evidence that concurrent use of aspirin mitigates the increased risk of serious CV thrombotic events associated with NSAID use.
The concurrent use of aspirin and NSAIDS, such as diclofenac, does increase the risk of serious GI events [see Warnings and Precautions (5.2)]
5.2 Gastrointestinal Effects – Risk of GI Ulceration, Bleeding, and Perforation
NSAIDs, including diclofenac, can cause serious gastrointestinal (GI) adverse events including bleeding, ulceration, and perforation of the stomach, small intestine, or large intestine, which can be fatal. These serious adverse events can occur at any time, with or without warning symptoms, in patients treated with NSAIDs. Only one in five patients who develop a serious upper GI adverse event on NSAID therapy is symptomatic. Upper GI ulcers, gross bleeding, or perforation caused by NSAIDs occur in approximately 1% of patients treated for 3 to 6 months, and in about 2 to 4% of patients treated for one year. These trends continue with longer duration of use, increasing the likelihood of developing a serious GI event at some time during the course of therapy. However, even short-term therapy is not without risk.
Prescribe NSAIDs, including diclofenac sodium topical solution, with extreme caution in those with a prior history of ulcer disease or gastrointestinal bleeding. Patients with a prior history of peptic ulcer disease and/or gastrointestinal bleeding who use NSAIDs have a greater than 10-fold increased risk for developing a GI bleed compared to patients with neither of these risk factors. Other factors that increase the risk of GI bleeding in patients treated with NSAIDs include concomitant use of oral corticosteroids or anticoagulants, longer duration of NSAID therapy, smoking, use of alcohol, older age, and poor general health status. Most spontaneous reports of fatal GI events are in elderly or debilitated patients and therefore, use special care when treating this population.
To minimize the potential risk for an adverse GI event, use the lowest effective dose for the shortest possible duration. Remain alert for signs and symptoms of GI ulceration and bleeding during diclofenac therapy and promptly initiate additional evaluation and treatment if a serious GI adverse event is suspected. For high-risk patients, consider alternate therapies that do not involve NSAIDs.
5.3 Hepatic Effects
Borderline elevations (less than 3 times the upper limit of the normal [ULN] range) or greater elevations of transaminases occurred in about 15% of oral diclofenac-treated patients in clinical trials of indications other than acute pain. Of the markers of hepatic function, ALT (SGPT) is recommended for the monitoring of liver injury.
In clinical trials of an oral diclofenac – misoprostol combination product, meaningful elevations (i.e., more than 3 times the ULN) of AST (SGOT) occurred in about 2% of approximately 5,700 patients at some time during diclofenac treatment (ALT was not measured in all studies).
In an open-label, controlled trial of 3,700 patients treated for 2 to 6 months, patients with oral diclofenac were monitored first at 8 weeks and 1,200 patients were monitored again at 24 weeks. Meaningful elevations of ALT and/or AST occurred in about 4% of the 3,700 patients and included marked elevations (>8 times the ULN) in about 1% of the 3,700 patients. In this open-label study, a higher incidence of borderline (less than 3 times the ULN), moderate (3 to 8 times the ULN), and marked (>8 times the ULN) elevations of ALT or AST was observed in patients receiving diclofenac when compared to other NSAIDs. Elevations in transaminases were seen more frequently in patients with osteoarthritis than in those with rheumatoid arthritis. Almost all meaningful elevations in transaminases were detected before patients became symptomatic.
Abnormal test occurred during the first 2 months of therapy with oral diclofenac in 42 of the 51 patients in all trials who developed marked transaminase elevations. In post marketing reports, cases of drug- induced hepatotoxicity have been reported in the first month, and in some cases, the first 2 months of NSAID therapy.
Post marketing surveillance has reported cases of sever hepatic reactions, including liver necrosis, jaundice, fulminant hepatitis with and without jaundice, and liver failure. Some of these reported cases resulted in fatalities or liver transplantation.
In a European retrospective population-based, case-controlled study, 10 cases of oral diclofenac associated drug-induced liver injury with current use compared with non-use of diclofenac were associated with a statistically significant 4-fold adjusted odds ratio of liver injury. In this particular study, based on an overall number of 10 cases of liver injury associated with diclofenac, the adjusted odds ratio increased further with female gender, doses of 150 mg or more, and duration of use for more than 90 days.
Measure transaminases (ALT and AST) periodically in patients receiving long-term therapy with diclofenac, because severe hepatotoxicity may develop without a prodrome of distinguishing symptoms. The optimum times for making the first and subsequent transaminase measurements are not known. Based on clinical trial data and post marketing experiences, monitor transaminases within 4 to 8 weeks after initiating treatment with diclofenac. However, severe hepatic reactions can occur at any time during treatment with diclofenac. If abnormal liver tests persist or worsen, if clinical signs and/or symptoms consistent with liver disease develop, or if systemic manifestations occur (e.g. eosinophilia, rash, abdominal pain, diarrhea, dark urine, etc.), discontinue diclofenac sodium topical solution immediately.
To minimize the possibility that hepatic injury will become severe between transaminase measurements, inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, diarrhea, pruritus, jaundice, right upper quadrant tenderness, and "flulike" symptoms), and the appropriate action to take if these signs and symptoms appear.
To minimize the potential risk for an adverse liver-related event in patients treated with diclofenac sodium topical solution, use the lowest effective dose for the shortest duration possible. Exercise caution when prescribing diclofenac sodium topical solution with concomitant drugs that are known to be potentially hepatotoxic (e.g., acetaminophen, certain antibiotics, antiepileptics). Caution patients to avoid taking unprescribed acetaminophen while using diclofenac sodium topical solution.
5.4 Hypertension
NSAIDs, including diclofenac, can lead to new onset or worsening of preexisting hypertension, either of which may contribute to the increased incidence of CV events. Use NSAIDs, including diclofenac sodium topical solution, with caution in patients with hypertension. Monitor blood pressure (BP) closely during the initiation of NSAID treatment and throughout the course of therapy.
Patients taking ACE-inhibitors, thiazides or loop diuretics may have impaired response to these therapies when taking NSAIDs.
5.5 Congestive Heart Failure and Edema
Fluid retention and edema have been observed in some patients treated with NSAIDs, including diclofenac sodium topical solution. Use diclofenac sodium topical solution with caution in patients with fluid retention or heart failure.
5.6 Renal Effects
Use caution when initiating treatment with diclofenac sodium topical solution in patients with considerable dehydration.
Long-term administration of NSAIDs has resulted in renal papillary necrosis and other renal injury. Renal toxicity has also been seen in patients in whom renal prostaglandins have a compensatory role in the maintenance of renal perfusion. In these patients, administration of an NSAID may cause a dose- dependent reduction in prostaglandin formation and, secondarily, in renal blood flow, which may precipitate overt renal decompensation. Patients at greatest risk of this reaction are those with impaired renal function, heart failure, liver dysfunction, those taking diuretics and ACE-inhibitors, and the elderly. Discontinuation of NSAID therapy is usually followed by recovery to the pretreatment state.
No information is available from controlled clinical studies regarding the use of diclofenac sodium topical solution in patients with advanced renal disease. Therefore, treatment with diclofenac sodium topical solution is not recommended in patients with advanced renal disease. If diclofenac sodium topical solution therapy is initiated, close monitoring of the patient's renal function is advisable.
5.7 Anaphylactoid Reactions
As with other NSAIDs, anaphylactoid reactions may occur in patients without prior exposure to diclofenac sodium topical solution. Do not prescribe diclofenac sodium topical solution to patients with the aspirin triad. This symptom complex typically occurs in asthmatic patients who experience rhinitis with or without nasal polyps, or who exhibit severe, potentially fatal bronchospasm after taking aspirin or other NSAIDs [see Contraindications (4) and Warnings and Precautions (5.10)]. Seek emergency help in cases where an anaphylactoid reaction occurs.
5.8 Skin Reactions
Do not apply diclofenac sodium topical solution to open skin wounds, infections, inflammations, or exfoliative dermatitis, as it may affect absorption and tolerability of the drug.
NSAIDs, including diclofenac sodium topical solution, can cause serious skin adverse events such as exfoliative dermatitis, Stevens-Johnson syndrome (SJS), and toxic epidermal necrolysis (TEN), which can be fatal. These serious events may occur without warning. Inform patients about the signs and symptoms of serious skin manifestations, and discontinue use of the drug at the first appearance of skin rash or any other signs of hypersensitivity.
5.9 Pregnancy
Diclofenac sodium topical solution should not be used by pregnant or nursing women or those intending to become pregnant.
5.10 Preexisting Asthma
Patients with asthma may have aspirin-sensitive asthma. The use of aspirin in patients with aspirin- sensitive asthma has been associated with severe bronchospasm, which can be fatal. Since cross- reactivity, including bronchospasm, between aspirin and other nonsteroidal anti-inflammatory drugs has been reported in such aspirin-sensitive patients, do not administer diclofenac sodium topical solution to patients with this form of aspirin sensitivity and use with caution in patients with preexisting asthma.
5.11 Sun Exposure
Instruct patients to avoid exposure to natural or artificial sunlight on treated knee(s) because studies in animals indicated topical diclofenac treatment resulted in an earlier onset of ultraviolet light-induced skin tumors. The potential effects of diclofenac sodium topical solution on skin response to ultraviolet damage in humans are not known.
5.12 Eye Exposure
Avoid contact of diclofenac sodium topical solution with eyes and mucosa. Advise patients that if eye contact occurs, immediately wash out the eye with water or saline and consult a physician if irritation persists for more than an hour.
5.13 Oral Nonsteroidal Anti-Inflammatory Drugs
Concomitant use of oral NSAIDs with diclofenac sodium topical solution resulted in a higher rate of rectal hemorrhage, more frequent abnormal creatinine, urea and hemoglobin. Therefore, do not use combination therapy with diclofenac sodium topical solution and an oral NSAID unless the benefit outweighs the risk and conduct periodic laboratory evaluations.
5.14 Corticosteroid Treatment
Diclofenac sodium topical solution cannot be expected to substitute for corticosteroids or to treat corticosteroid insufficiency. Abrupt discontinuation of corticosteroids may lead to exacerbation of corticosteroid-response illness. For patients on prolonged corticosteroid therapy, taper slowly if a decision is made to discontinue corticosteroids.
5.15 Inflammation
The pharmacological activity of diclofenac sodium topical solution in reducing inflammation, and possibly fever, may diminish the utility of these diagnostic signs in detecting complications of presumed noninfectious, painful conditions. Hematological Effects
The effects of diclofenac sodium topical solution on platelet function were studied in 10 healthy subjects administered 80 drops four times a day for 7 days. There was no significant change in platelet aggregation following one week of treatment [see Clinical Pharmacology (12.4)].
Anemia is sometimes seen in patients receiving NSAIDs. This may be due to fluid retention, occult or gross GI blood loss, or an incompletely described effect upon erythropoiesis. Check hemoglobin or hematocrit of patients on diclofenac sodium topical solution if they exhibit any signs or symptoms of anemia or blood loss.
NSAIDs inhibit platelet aggregation and have been shown to prolong bleeding time in some patients. Unlike aspirin, their effect on platelet function is quantitatively less, of shorter duration and reversible. Carefully monitor patients receiving diclofenac sodium topical solution who may be adversely affected by alteration in platelet function, such as those with coagulation disorders or patients receiving anticoagulants.
5.16 Monitoring
Because serious GI tract ulcerations and bleeding can occur without warning symptoms in patients taking NSAIDs, monitor patients for signs or symptoms of GI bleeding. Check CBC and a chemistry profile periodically in patients on long-term treatment with NSAIDs. Discontinue diclofenac sodium topical solution if abnormal liver tests or renal tests persist or worsen.
6. Adverse Reactions/Side Effects
6.1 Clinical Studies Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of another drug cannot be directly compared to rates in the clinical trial of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to diclofenac sodium topical solution of 911 patients treated between 4 and 12 weeks (mean duration of 49 days) in seven Phase 3 controlled trials, as well as exposure of 793 patients treated in an open-label study, including 463 patients treated for at least 6 months, and 144 patients treated for at least 12 months. The population mean age was approximately 60 years, 89% of patients were Caucasians, 64% were females, and all patients had primary osteoarthritis. The most common adverse events with diclofenac sodium topical solution were application site skin reactions. These events were the most common reason for withdrawing from the studies.
Application site reactions:
In controlled trials, the most common treatment related adverse events in patients receiving diclofenac sodium topical solution were application site skin reactions. Application site reactions were characterized by one or more of the following: dryness, erythema, induration, vesicles, paresthesia, pruritus, vasodilation, acne, and urticaria. The most frequent of these reactions were dry skin (32%), contact dermatitis characterized by skin erythema and induration (9%), contact dermatitis with vescicles (2%) and pruritus (4%). In one controlled trial, a higher rate of contact dermatitis with vesicles (4%) was observed after treatment of 152 subjects with the combination of diclofenac sodium topical solution and oral diclofenac. In the open label uncontrolled long-term safety study, contact dermatitis occurred in 13% and contact dermatitis with vesicles in 10% of patients, generally within the first 6 months of exposure, leading to a withdrawal rate for an application site event of 14%.
Adverse events common to the NSAID class:
In controlled trials, subjects treated with diclofenac sodium topical solution experienced some adverse events associated with the NSAID class more frequently than subjects using placebo (constipation, diarrhea, dyspepsia, nausea, flatulence, abdominal pain, edema; see Table 1). The combination of diclofenac sodium topical solution and oral diclofenac, compared to oral diclofenac alone, resulted in a higher rate of rectal hemorrhage (3% vs. less than 1%), and more frequent abnormal creatinine (12% vs. 7%), urea (20% vs. 12%), and hemoglobin (13% vs. 9%), but no difference in elevation of liver transaminases.
Table 1: lists all adverse reactions occurring in ≥1% of patients receiving diclofenac sodium topical solution, where the rate in the diclofenac sodium topical solution group exceeded placebo, from seven controlled studies conducted in patients with osteoarthritis. Since these trials were of different durations, these percentages do not capture cumulative rates of occurrence.
| Treatment Group: | Diclofenac Sodium Topical Solution N=911 | Topical Placebo N= 332 |
|---|---|---|
| Adverse Reaction* | N(%) | N(%) |
|
||
| Dry Skin (Application Site) | 292 (32) | 17 (5) |
| Contact Dermatitis (Application Site) | 83 (9) | 6 (2) |
| Dyspepsia | 72 (8) | 13 (4) |
| Abdominal Pain | 54 (6) | 10 (3) |
| Flatulence | 35 (4) | 1 (<1) |
| Pruritus (Application Site) | 34 (4) | 7 (2) |
| Diarrhea | 33 (4) | 7 (2) |
| Nausea | 33 (4) | 3 (1) |
| Pharyngitis | 40 (4) | 13 (4) |
| Constipation | 29 (3) | 1 (<1) |
| Edema | 26 (3) | 0 |
| Rash (Non-Application Site) | 25 (3) | 5 (2) |
| Infection | 25 (3) | 8 (2) |
| Ecchymosis | 19 (2) | 1 (<1) |
| Dry Skin (Non-Application Site) | 19 (2) | 1 (<1) |
| Contact Dermatitis, vesicles (Application Site) | 18 (2) | 0 |
| Paresthesia (Non-Application Site) | 14 (2) | 3 (<1) |
| Accidental Injury | 22 (2) | 7 (2) |
| Pruritus (Non-Application Site) | 15 (2) | 2 (<1) |
| Sinusitis | 10 (1) | 2 (<1) |
| Halitosis | 11 (1) | 1 (<1) |
| Application Site Reaction (not otherwise specified) | 11 (1) | 3 (<1) |
6.2 Post marketing Experience
In non – U.S. post marketing surveillance, the following adverse reactions have been reported during post-approval use of diclofenac sodium topical solution. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Body as a Whole: abdominal pain, accidental injury, allergic reaction, asthenia, back pain, body odor, chest pain, edema, face edema, halitosis, headache, lack of drug effect, neck rigidity, pain
Cardiovascular: palpitation, cardiovascular disorder
Digestive: diarrhea, dry mouth, dyspepsia, gastroenteritis, decreased appetite, mouth ulceration, nausea, rectal hemorrhage, ulcerative stomatitis
Metabolic and Nutritional: creatinine increased
Musculoskeletal: leg cramps, myalgia
Nervous: depression, dizziness, drowsiness, lethargy, paresthesia, paresthesia at application site
Respiratory: asthma, dyspnea, laryngismus, laryngitis, pharyngitis
Skin and Appendages: At the Application Site: contact dermatitis, contact dermatitis with vesicles, dry skin, pruritus, rash;
Other Skin and Appendages Adverse Reactions: eczema, rash, pruritus, skin discoloration, urticaria
Special senses: abnormal vision, blurred vision, cataract, ear pain, eye disorder, eye pain, taste perversion
7. Drug Interactions
Drug interactions with the use of diclofenac sodium topical solution have not been studied. The following drug interactions [sections 7.1 to 7.7] are noted for oral diclofenac sodium.
7.1 Aspirin
When diclofenac is administered with aspirin, the binding of diclofenac to protein is reduced, although the clearance of free diclofenac is not altered. The clinical significance of this interaction is not known; however, as with other NSAIDs, concomitant administration of diclofenac and aspirin is not generally recommended because of the potential of increased adverse effects.
7.2 Anticoagulants
The effects of anticoagulants such as warfarin and NSAIDs on GI bleeding are synergistic, such that users of both drugs together have a risk of serious GI bleeding higher than users of either drug alone.
7.3 ACE-Inhibitors
NSAIDs may diminish the antihypertensive effect of angiotensin converting enzyme (ACE) inhibitors. Consider this interaction in patients taking NSAIDs concomitantly with ACE-inhibitors.
7.4 Diuretics
Clinical studies, as well as post marketing observations, have shown that NSAIDs can reduce the natriuretic effect of furosemide and thiazides in some patients. The response has been attributed to inhibition of renal prostaglandin synthesis. During concomitant therapy with NSAIDs, observe the patient closely for signs of renal failure [see Warnings and Precautions (5.6)], as well as to assure diuretic efficacy.
7.5 Lithium
NSAIDs have produced an elevation of plasma lithium levels and a reduction in renal lithium clearance. The mean minimum lithium concentration increased 15% and the renal clearance was decreased by approximately 20%. These effects have been attributed to inhibition of renal prostaglandin synthesis by the NSAID. Thus, when NSAIDs, including diclofenac, and lithium are administered concurrently, observe patients carefully for signs of lithium toxicity.
7.6 Methotrexate
NSAIDs have been reported to competitively inhibit methotrexate accumulation in rabbit kidney slices. This may indicate that they could enhance the toxicity of methotrexate. Use caution when NSAIDs, including diclofenac, are administered concomitantly with methotrexate.
7.7 Cyclosporine
Diclofenac, like other NSAIDs, may affect renal prostaglandins and increase the toxicity of certain drugs. Therefore, concomitant therapy with diclofenac may increase cyclosporine's nephrotoxicity. Use caution when diclofenac is administered concomitantly with cyclosporine.
7.8 Oral Nonsteroidal Anti-Inflammatory Drugs
Concomitant use of oral NSAIDs with diclofenac sodium topical solution has been evaluated in one Phase 3 controlled trial and in combination with oral diclofenac, compared to oral diclofenac alone, resulted in a higher rate of rectal hemorrhage (3% vs. less than 1%), and more frequent abnormal creatinine (12% vs. 7%), urea (20% vs. 12) and hemoglobin (13% vs. 9%). Therefore, do not use combination therapy with diclofenac sodium topical solution and an oral NSAID unless the benefit outweighs the risk and conduct periodic laboratory evaluations.
8. Use In Specific Populations
8.1 Pregnancy
Pregnancy Category C prior to 30 weeks gestation; Category D starting 30 weeks gestation.
Teratogenic Effects:
There are no adequate and well-controlled studies of diclofenac sodium topical solution in pregnant women. Diclofenac sodium topical solution should not be used by pregnant women as its safe use has not been adequately determined and starting at 30 weeks gestation, diclofenac and other NSAIDs should be avoided by pregnant women as premature closure of the ductus arteriosus in the fetus may occur.
Developmental studies in animals demonstrated that diclofenac sodium administration did not produce teratogenicity despite the induction of maternal toxicity and fetal toxicity in mice at doses up to 20 mg/kg/day (0.6-fold the maximum recommended human dose [MRHD] of 154 mg/day based on body surface area comparison), and in rats and rabbits at doses up to 10 mg/kg/day (approximately 0.6-fold and 1.3-fold the MRHD, respectively). Published reproductive and developmental studies of dimethyl sulfoxide (DMSO, the solvent used in diclofenac sodium topical solution) are equivocal as to potential teratogenicity.
8.2 Labor and Delivery
The effects of diclofenac sodium topical solution on labor and delivery in pregnant women are unknown. In rat studies maternal exposure to diclofenac, as with other NSAID drugs, known to inhibit prostaglandin synthesis, increased the incidence of dystocia, delayed parturition, and decreased offspring survival.
8.3 Nursing Mothers
It is not known whether this drug is excreted in human milk; however, there is a case report in the literature indicating that diclofenac can be detected at low levels in breast milk. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from diclofenac sodium topical solution, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.5 Geriatric Use
Of the 911 patients treated with diclofenac sodium topical solution in seven controlled Phase 3 clinical trials, 444 subjects were 65 years of age and over. There was no age-related difference in the incidence of adverse events. Of the 793 patients treated with diclofenac sodium topical solution in one open-labeled safety trial, 334 subjects were 65 years of age and over including 107 subjects 75 and over. There was no difference in the incidence of adverse events with long-term exposure to diclofenac sodium topical solution for this elderly population. As with any NSAID, use caution in treating the elderly (65 years and older) and it may be useful to monitor renal function since they are more likely to have decreased baseline renal function.
10. Overdosage
There have been no known experiences of overdose with diclofenac sodium topical solution.
Symptoms following acute NSAID overdose are usually limited to lethargy, drowsiness, nausea, vomiting, and epigastric pain, which are generally reversible with supportive care. Gastrointestinal bleeding can occur. Hypertension, acute renal failure, respiratory depression and coma may occur, but are rare. Anaphylactoid reactions have been reported with therapeutic ingestion of NSAIDs, and may occur following an overdose.
Manage patients using symptomatic and supportive care following an NSAID overdose. There are no specific antidotes. Emesis is not recommended due to a possibility of aspiration and subsequent respiratory irritation by DMSO contained in diclofenac sodium topical solution. Activated charcoal (60 to 100 g in adults, 1 to 2 g/kg in children) and/or osmotic cathartic may be indicated in patients seen within 4 hours of ingestion with symptoms or following a large overdose (5 to 10 times the usual dose). Forced diureses, alkalinization of urine, hemodialysis, or hemoperfusion may not be useful due to high protein binding.
For additional information about overdose treatment, call a poison control center (1-800-222-1222).
11. Lorvatus Pharmapak Description
Diclofenac sodium topical solution is a clear, colorless to faintly pink-orange solution for topical application.
Diclofenac sodium topical solution contains 1.5% w/w diclofenac sodium, a benzeneacetic acid derivative that is a nonsteroidal anti-inflammatory drug (NSAID), designated chemically as 2-[(2,6- dichlorophenyl)amino]-benzeneacetic acid, monosodium salt. The molecular weight is 318.14. Its molecular formula is C14H10Cl2NNaO2 and it has the following structural formula:
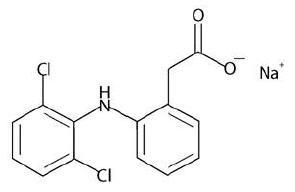
Each 1 mL of solution contains 16.05 mg of diclofenac sodium. In addition diclofenac sodium topical solution contains the following inactive ingredients: dimethyl sulfoxide USP (DMSO, 45.5% w/w), propylene glycol, alcohol, glycerin and purified water.
12. Lorvatus Pharmapak - Clinical Pharmacology
12.1 Lorvatus Pharmapak Mechanism of Action
The mechanism of action of diclofenac is similar to that of other nonsteroidal anti-inflammatory drugs. Diclofenac inhibits the enzyme, cyclooxygenase (COX), an early component of the arachidonic acid cascade, resulting in the reduced formation of prostaglandins, thromboxanes and prostacylin. It is not completely understood how reduced synthesis of these compounds results in therapeutic efficacy.
12.2 Pharmacodynamics
Diclofenac, the active component of diclofenac sodium topical solution has anti-inflammatory, anti-nociception, and antipyretic effects.
12.3 Pharmacokinetics
After topical administration to healthy human volunteers of single and multiple maximum doses of diclofenac sodium topical solution, 40 drops (approximately 1.2 mL) to each knee (80 drops total dose), the following diclofenac pharmacokinetic parameters were obtained: (see Table 2).
| Pharmacokinetic Parameters | Diclofenac sodium | |
|---|---|---|
| Normal Adults [N=18] (Age: 18-55 years) | Normal Adults [N=19] (Age: 18-55 years) |
|
| Single Dose | Multiple Dose Four times daily for 7 days |
|
|
||
| AUC0-t | 177.5 ± 72.6 ng.h/mL | 695.4 ± 348.9 ng.h/mL |
| AUC0-inf | 196.3 ± 68.5 ng.h/mL | 745.2 ± 374.7 ng.h/mL |
| Plasma Cmax | 8.1 ± 5.9 ng/mL | 19.4 ± 9.3 ng/mL |
| Plasma Tmax (h) | 11.0 ± 6.4 | 4.0 ± 6.5 |
| Plasma t1/2 (h) | 36.7 ± 20.8 | 79.0 ± 38.1 |
| Kel (h-1) | 0.024 ± 0.010 | 0.011 ± 0.004 |
| CL/F (L/h) | 244.7 ± 84.7* | - |
Absorption
Diclofenac systemic exposure from diclofenac sodium topical solution application (4 times daily for 1 week) was approximately 1/3 of the diclofenac systemic exposure from the Solaraze (diclofenac topical gel) application (twice daily for 4 weeks).
Distribution
Diclofenac is more than 99% bound to human serum proteins, primarily to albumin.
Diclofenac diffuses into and out of the synovial fluid. Diffusion into the joint occurs when plasma levels are higher than those in the synovial fluid, after which the process reverses and synovial fluid levels are higher than plasma levels. It is not known whether diffusion into the joint plays a role in the effectiveness of diclofenac.
Metabolism
Five diclofenac metabolites have been identified in human plasma and urine. The metabolites include 4'- hydroxy-, 5-hydroxy-, 3'-hydroxy-, 4',5-dihydroxy- and 3'-hydroxy-4'-methoxy diclofenac. The major diclofenac metabolite, 4'-hydroxy-diclofenac, has very weak pharmacologic activity. The formation of 4'-hydroxy diclofenac is primarily mediated by CPY2C9. Both diclofenac and its oxidative metabolites undergo glucuronidation or sulfation followed by bilIary excretion. Acylglucuronidation mediated by UGT2B7 and oxidation mediated by CPY2C8 may also play a role in diclofenac metabolism. CYP3A4 is responsible for the formation of minor metabolites, 5-hydroxy and 3'-hydroxy-diclofenac.
12.4 Platelets
The effect of diclofenac sodium topical solution on platelet function was evaluated in 10 healthy human volunteers as a sub-study of a multiple-dose pharmacokinetic study [see Pharmacokinetics (12.3)].
Average (range) platelet aggregation time following stimulation with adenosine diphosphate, collagen, epinephrine and arachidonic acid was 101.3% (73.3 to 128.1), 99.8% (69.6 to 112.9), 109.9% (66.2 to 178.1) and 99.0% (15.5 to 126.6) of baseline value, respectively. These results indicate that there was no effect on platelet aggregation after application of the maximum clinical dose for 7 days [see Pharmacokinetics (12.3)].
13. Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies in mice and rats administered diclofenac sodium, as a dietary constituent for 2 years resulted in no significant increases in tumor incidence at doses up to 2 mg/kg/day corresponding to approximately 0.35-and 0.7-fold (mouse and rat, respectively) of the maximum recommended human topical dose (MRHD) of diclofenac sodium topical solution (based on apparent bioavailability and body surface area comparison).
In a dermal carcinogenicity study conducted in albino mice, daily topical applications of diclofenac sodium for two years at concentrations up to 0.035% diclofenac sodium (a 43-fold lower diclofenac sodium concentration than present in diclofenac sodium topical solution) did not increase neoplasm incidence.
In a photococarcinogenicity study conducted in hairless mice, topical application of diclofenac sodium at doses up to 0.035% diclofenac sodium (a 43-fold lower diclofenac sodium concentration than present in diclofenac sodium topical solution) resulted in an earlier median time of onset of tumors.
Mutagenesis: Diclofenac was not mutagenic or clastogenic in a battery of genotoxicity tests that included the bacterial reverse mutation assay, in vitro mouse lymphoma point mutation assay, chromosomal aberration studies in Chinese hamster ovarian cells in vitro, and in vivo rat chromosomal aberration assay of bone marrow cells.
Impairment of Fertility: Fertility studies have not been conducted with diclofenac sodium topical solution. Diclofenac sodium administered to male and female rats at doses up to 4 mg/kg/day (1.4-fold of the MRHD of diclofenac sodium topical solution based on apparent bioavailability and body surface area comparison) did not affect fertility. Studies have not been conducted to determine the safety of DMSO on fertility.
13.2 Animal Toxicology and/or Pharmacology
Ocular Effects
No adverse effects were observed using indirect ophthalmoscopy after multiple-daily dermal application to rats for 26 weeks and minipigs for 52 weeks of DMSO at twice the concentration found in diclofenac sodium topical solution. Published studies of dermal or oral administration of DMSO to rabbits, dogs and pigs described refractive changes of lens curvature and cortical fibers indicative of myopic changes and/or incidences of lens opacity or discoloration when evaluated using slit-lamp biomicroscopy examination, although no ocular abnormalities were observed in rhesus monkeys during daily oral or dermal treatment with DMSO for 9 to 18 months.
14. Clinical Studies
14.1 Pivotal Studies in Osteoarthritis of the Knee
The use of diclofenac sodium topical solution for the treatment of the signs and symptoms of osteoarthritis of the knee was evaluated in two double-blind controlled trials conducted in the U.S. and Canada, involving patients treated with diclofenac sodium topical solution at a dose of 40 drops four times a day for 12 weeks. Diclofenac sodium topical solution was compared to topical placebo (2.3% DMSO with other excipients) and/or topical vehicle solution (45.5% w/w DMSO with other excipients), applied directly to the study knee. In both trials, diclofenac sodium topical solution treatment resulted in statistically significant clinical improvement compared to placebo and/or vehicle, in all three primary efficacy variables – pain, physical function (Western Ontario and McMaster Universities LK3.1 OA Index (WOMAC) pain and physical function dimensions) and Patient Overall Health Assessment (POHA)/Patient Global Assessment (PGA). Numerical results are summarized in Tables 3 and 4.
| Efficacy Variable | Study I | |||
|---|---|---|---|---|
| Mean baseline score and mean change in efficacy variables after 12 weeks of treatment | ||||
| Mean Baseline score | Diclofenac sodium N=154 | Topical placebo*
N=155 | Topical vehicle†
N=161 |
|
| WOMAC pain score | 13 | -6.0 | -4.7 | -4.7 |
| (Likert 3.1, 0-20) | ||||
| WOMAC physical function (Likert 3.1, 0-68) | 42 | -15.7 | -12.3 | -12.1 |
| POHA (0-4) | 2.3 | -1.0 | -0.4 | -0.6 |
| Efficacy Variable | Study II | ||
|---|---|---|---|
| Mean baseline score and mean change in efficacy variables after 12 weeks of treatment | |||
| Mean Baseline score | Diclofenac sodium N=164 | Topical vehicle*
N=162 |
|
|
|||
| WOMAC pain score (Likert 3.1, 0-20) | 13 | -5.9 | -4.4 |
| WOMAC physical function (Likert 3.1, 0-68) | 42 | -15.3 | -10.3 |
| PGA (0-4) | 3.1 | -1.3 | -1.0 |
16. How is Lorvatus Pharmapak supplied
Diclofenac Sodium Topical Solution is supplied as a clear, colorless to faintly pink-orange solution containing 16.05 mg of diclofenac sodium per mL of solution, in a white high density polyethylene bottle with a white low-density dropper cap.
| NDC Number & Size | |
|---|---|
| NDC # 51021-150-05 | 150 mL bottle |
17. Patient Counseling Information
See FDA-Approved Patient Labeling (Medication Guide and Instructions for Use).
17.1 Patient/Caregiver Instructions
Inform patients of the following information before initiating therapy with an NSAID and periodically during the course of ongoing therapy. Encourage patients to read the NSAID Medication Guide that accompanies each prescription dispensed prior to using diclofenac sodium topical solution [see Medication Guide and Instructions for Use].
17.2 Cardiovascular Effects
Diclofenac sodium topical solution, like other NSAIDs, may cause serious DV side effects, such as MI or stroke, which may result in hospitalization and even death. Although serious CV events can occur without warning symptoms, instruct patients to be alert for the signs and symptoms of chest pain, shortness of breath weakness, slurring of speech, and to ask for medical advice when observing any indicative sign or symptoms. Inform patients of the importance of this follow-up [see Warnings and Precautions (5.1)].
17.3 Gastrointestinal Effects
Diclofenac sodium topical solution, like other NSAIDs, may cause GI discomfort and, rarely, serious GI side effects, such as ulcers and bleeding, which may result in hospitalization and even death.
Although serious GI tract ulcerations and bleeding can occur without warning symptoms, inform patients to be alert for the signs and symptoms of ulceration and bleeding, and to ask for medical advice when observing any indicative sign or symptoms including epigastric pain, dyspepsia, melena, and hematemesis. Instruct patients of the importance of this follow-up [see Warnings and Precautions (5.2)].
17.4 Hepatotoxicity
Inform patients of the warning signs and symptoms of hepatotoxicity (e.g., nausea, fatigue, lethargy, pruritus, jaundice, right upper quadrant tenderness, and "flu-like" symptoms). If these occur, instruct patients to stop therapy with diclofenac sodium topical solution and seek immediate medical therapy [see Warnings and Precautions (5.3)].
17.5 Adverse Skin Reactions
Diclofenac sodium topical solution, like other NSAIDs, can cause serious systemic skin side effects such as exfoliative dermatitis, SJS, and TEN, which may result in hospitalizations and even death.
Although serious systemic skin reactions may occur without warning, instruct patients to be alert for the signs and symptoms of skin rash and blisters, fever, or other signs of hypersensitivity such as itching, and to ask for medical advice when observing any indicative signs or symptoms [see Warnings and Precautions (5.8)].
Advise patients to stop diclofenac sodium topical solution immediately if they develop any type of generalized rash and contact their physicians as soon as possible.
Diclofenac sodium topical solution can cause a localized skin reaction at the application site. Advise patients to contact their physicians as soon as possible of they develop any type of localized application site rash.
Instruct patients not to apply diclofenac sodium topical solution to open skin wounds, infections, inflammations, or exfoliative dermatitis, as it may affect absorption and reduce tolerability of the drug.
Instruct patients to wait until the area treated with diclofenac sodium topical solution is completely dry before applying sunscreen, insect repellant, lotion, moisturizer, cosmetics, or other topical medication.
Instruct patients to minimize or avoid exposure of treated knee(s) to natural or artificial sunlight.
17.6 Weight Gain and Edema
Instruct patients to promptly report to their physician signs or symptoms of unexplained weight gain or edema following treatment with diclofenac sodium topical solution [see Warnings and Precautions (5.5)].
17.7 Anaphylactoid Reactions
Inform patients of the signs of an anaphylactoid reaction (e.g. difficulty breathing, swelling of the face or throat). If these occur, instruct patients to seek immediate emergency help [see Warnings and Precautions (5.7)].
17.8 Effects During Pregnancy
Instruct patients who are pregnant or intending to become pregnant not to use diclofenac sodium topical solution [see Use in Specific Populations (8.1) and Impairment of Fertility (13.1)].
17.9 Eye Exposure
Instruct patients to avoid contact of diclofenac sodium topical solution with the eyes and mucosa. Advise patients that if eye contact occurs, immediately wash out the eye with water or saline and consult a physician if irritation persists for more than an hour.
17.10 Prevention of Secondary Exposure
Instruct patients to avoid skin-to-skin contact between other people and the knee(s) to which diclofenac sodium topical solution was applied until the knee(s) is completely dry.
Medication Guide for Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
(See the end of this Medication Guide for a list of prescription NSAID medicines.)
What is the most important information I should know about medicines called Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)?
NSAID medicines may increase the chance of a heart attack or stroke that can lead to death.
This chance increases:
- with longer use of NSAID medicines in people who have heart disease
NSAID medicines should never be used right before or after a heart surgery called a "coronary artery bypass graft (CABG)."
NSAID medicines can cause ulcers and bleeding in the stomach and intestines at any time during treatment. Ulcers and bleeding:
- can happen without warning symptoms may cause death
The chance of a person getting an ulcer or bleeding increases with:
- taking medicines called "corticosteroids" and "anticoagulants"
- longer use
- smoking
- drinking alcohol
- older age
- having poor health NSAID medicines should only be used:
- exactly as prescribed at the lowest dose possible for your treatment for the shortest time needed
What are Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)?
NSAID medicines are used to treat pain and redness, swelling, and heat (inflammation) from medical conditions such as:
- different types of arthritis, menstrual cramps and other types of short-term pain
Who should not take a Non-Steroidal Anti-Inflammatory Drug (NSAID)?
Do not take an NSAID medicine: if you had an asthma attack, hives, or other allergic reaction with aspirin or any other NSAID medicine or pain right before or after heart bypass surgery
Tell your healthcare provider:
- about all of your medical conditions.
- about all of the medicines you take. NSAIDs and some other medicines can interact with each other and cause serious side effects. Keep a list of your medicines to show to your healthcare provider and pharmacist.
- if you are pregnant, NSAID medicines should not be used by pregnant women late in their pregnancy.
- if you are breastfeeding. Talk to your doctor.
What are the possible side effects of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)?
Serious side effects include:
| Other side effects include:
|
Get emergency help right away if you have any of the following symptoms:
- shortness of breath or trouble breathing chest pain
- slurred speech
- weakness in one part or side of your body swelling of the face or throat
Stop your NSAID medicine and call your healthcare provider right away if you have any of the following symptoms:
- nausea
- more tired or weaker than usual itching
- your skin or eyes look yellow
- stomach pain
- flu-like symptoms
- vomit
- blood
- there is blood in your bowel movement or it is black and sticky like tar
- unusual weight gain
- skin rash or blisters with fever
- swelling of the arms and legs, hands and feet
These are not all the side effects with NSAID medicines. Talk to your healthcare provider or pharmacist for more information about NSAID medicines.
Call your doctor for medical advice about s ide effects. You may report s ide effects to FDA at 1- 800-FDA-1088.
Other information about Non-Steroidal Anti-Inflammatory Drugs (NSAIDs):
- Aspirin is an NSAID medicine but it does not increase the chance of a heart attack. Aspirin can cause bleeding in the brain, stomach, and intestines. Aspirin can also cause ulcers in the stomach and intestines.
- Some of these NSAID medicines are sold in lower doses without a prescription (over-the-counter). Talk to your healthcare provider before using over-the-counter NSAIDs for more than 10 days.
NSAID medicines that need a prescription
| Generic Name | Trade name |
|---|---|
|
|
| Celecoxib | Celebrex® |
| Diclofenac | Flector, Cataflam®, Voltaren®, Arthrotec™(combined with misoprostol), PENNSAID® (Diclofenac Sodium Topical Solution) |
| Diflunisal | Dolobid® |
| Etodolac | Lodine®, Lodine® XL |
| Fenoprofen | Nalfon®, Nalfon® 200 |
| Flurbiprofen | Ansaid® |
| Ibuprofen | Motrin®, Tab-Profen®, Vicoprofen®* (combined with hydrocodone), Combunox™ (combined with oxycodone) |
| Indomethacin | Indocin®, Indocin® SR, Indo-Lemmon™, Indomethagan™ |
| Ketoprofen | Oruvail® |
| Ketorolac | Toradol® |
| Mefenamic Acid | Ponstel® |
| Meloxicam | Mobic® |
| Nabumetone | Relafen® |
| Naproxen | Naprosyn®, Anaprox®, Anaprox® DS, EC- Naproxyn®, Naprelan®, Naprapac® (copackaged with lansoprazole) |
| Oxaprozin | Daypro® |
| Piroxicam | Feldene® |
| Sulindac | Clinoril® |
| Tolmetin | Tolectin®, Tolectin® DS, Tolectin® 600 |
This Medication Guide has been approved by the U.S. Food and Drug Administration.
17.11 Patient Instructions for Use
Diclofenac Sodium Topical Solution
Read the Medication Guide that comes with diclofenac sodium topical solution first. Be sure that you read, understand, and follow these Instructions for Use before you use diclofenac sodium topical solution for the first time.
Important: For use on the skin only (topical). Do not get diclofenac sodium topical solution in your eyes, nose or mouth.
Before you use diclofenac sodium topical solution:
- Apply diclofenac sodium topical solution exactly as your healthcare provider tells you. Talk with your healthcare provider or pharmacist if you are not sure.
- Only use diclofenac sodium topical solution to treat pain from osteoarthritis in your knee or knees. Apply diclofenac sodium topical solution on clean dry skin that does not have any cuts, infections or rashes.
- Use diclofenac sodium topical solution 4 times each day on your knee or knees as prescribed. Your total dose for each knee is 40 drops of diclofenac topical solution, each time you use it.
- If you get diclofenac sodium topical solution in your eyes, rinse your eyes right away with water or saline. Call your healthcare provider if your eyes are irritated for more than one hour.
Steps for using diclofenac sodium topical solution:
Step 1. Wash your hands with soap and water before and after applying diclofenac sodium topical solution.
Step 2. Put 10 drops of diclofenac sodium topical solution either on your hand or directly on your knee (See Figure A).
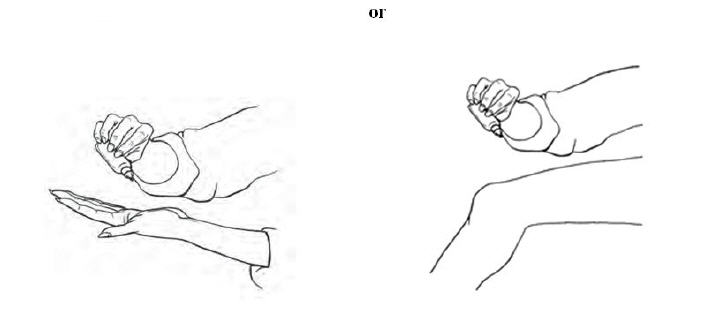
Step 3. Spread diclofenac sodium topical solution evenly on the front, back and sides of your knee (see Figures B and C). Repeat steps 2 and 3, three times so that your knee is completely covered with a total of 40 drops of diclofenac sodium topical solution.
Figure B
Figure C
Step 4. If your healthcare provider has prescribed diclofenac sodium topical solution for both knees, repeat steps 2 and 3 for the other knee.
After you use diclofenac sodium topical solution:
Wash your hands with soap and water right away after applying diclofenac sodium topical solution.
Do not
- touch the treated knee or allow another person to touch the knee treated with diclofenac sodium topical solution until your knee is completely dry.
- cover your knee with clothing until your knee is completely dry.
- put sunscreen, insect repellant, lotion, moisturizer, cosmetics, or other topical medicines on your knee until it is completely dry.
- take a shower or a bath for at least 30 minutes after you put diclofenac sodium topical solution on your knee(s).
- use heating pads or apply bandages to the skin where you have applied diclofenac sodium topical solution.
- use sunlamps and tanning beds. Protect your treated knee from sunlight. Wear clothes that cover your skin if you have to be in sunlight.
How should I store diclofenac sodium topical solution?
- Store diclofenac sodium topical solution between 68° F to 77°F (20°C to 25°C).
Keep diclofenac sodium topical solution and all medicines out of the reach of children.
This Instructions for Use has been approved by the U.S. Food and Drug Administration.
Brands mentioned are trademarks of their respective owners.
Manufactured for:
Sircle Laboratories, LLC
Madison, MS 39110
Lorvatus Pharmapak Description
Metaxalone is available as an 800 mg, light pink to pink, capsule shaped, scored uncoated tablet.
Chemically, metaxalone is 5-[(3,5- dimethylphenoxy) methyl]-2-oxazolidinone. The empirical formula is C12H15NO3, which corresponds to a molecular weight of 221.25. The structural formula is:
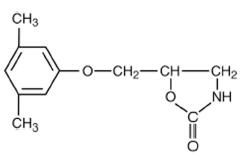
Metaxalone is a white to almost white, odorless crystalline powder freely soluble in chloroform, soluble in methanol and in 96% ethanol, but practically insoluble in ether or water.
Each tablet contains 800 mg metaxalone and the following inactive ingredients: calcium carbonate, FD& C Red # 40, hypromellose, lactose monohydrate, microcrystalline cellulose, povidone, silicone dioxide, sodium starch glycol ate and sodium stearyl fumarate.
Lorvatus Pharmapak - Clinical Pharmacology
Lorvatus Pharmapak Mechanism of Action
The mechanism of action of metaxalone in humans has not been established, but may be due to general central nervous system depression. Metaxalone has no direct action on the contractile mechanism of striated muscle, the motor end plate or the nerve fiber.
Pharmacokinetics
The pharmacokinetics of metaxalone have been evaluated in healthy adult volunteers after single dose administration of metaxalone under fasted and fed conditions at doses ranging from 400 mg to 800 mg.
Absorption
Peak plasma concentrations of metaxalone occur approximately 3 hours after a 400 mg oral dose under fasted conditions. Thereafter, metaxalone concentrations decline log-linearly with a terminal half-life of 9.0 ± 4.8 hours. Doubling the dose of metaxalone from 400 mg to 800 mg results in a roughly proportional increase in metaxalone exposure as indicated by peak plasma concentrations (Cmax) and area under the curve (AUC). Dose proportionality at doses above 800 mg has not been studied. The absolute bioavailability of metaxalone is not known.
The single-dose pharmacokinetic parameters of metaxalone in two groups of healthy volunteers are shown in Table 1.
Food Effects
A randomized, two-way, crossover study was conducted in 42 healthy volunteers (31 males, 11 females) administered one 400 mg metaxalone tablet under fasted conditions and following a standard high-fat breakfast. Subjects ranged in age from 18 to 48 years (mean age = 23.5 ± 5.7 years). Compared to fasted conditions, the presence of a high fat meal at the time of drug administration increased Cmax by 177.5% and increased AUC (AUC0-t, AUC∞) by 123.5% and 115.4%, respectively. Time-to-peak concentration (Tmax) was also delayed (4.3 h versus 3.3 h) and terminal half-life was decreased (2.4 h versus 9.0 h) under fed conditions compared to fasted.
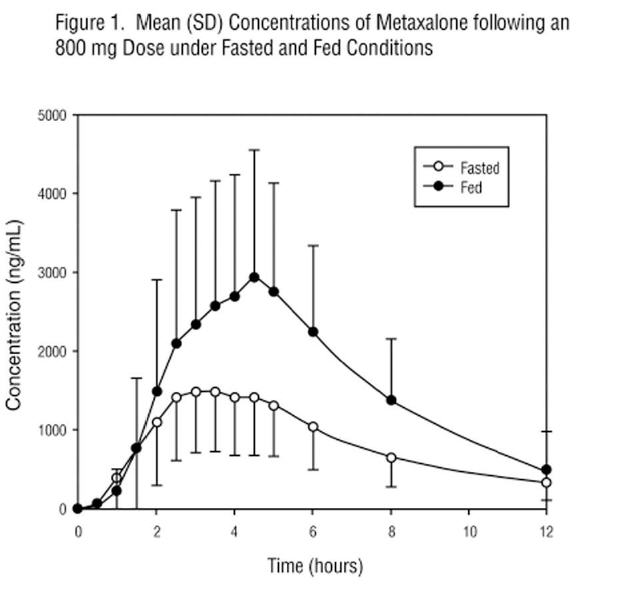
In a second food effect study of similar design, two 400 mg metaxalone tablets (800 mg) were administered to healthy volunteers (N=59, 37 males, 22 females), ranging in age from 18 to 50 years (mean age = 25.6± 8.7 years). Compared to fasted conditions, the presence of a high fat meal at the time of drug administration increased Cmax by 193.6% and increased AUC (AUC0-t, AUC∞) by 146.4% and 142.2%, respectively. Time-to-peak concentration (Tmax) was also delayed (4.9 h versus 3.0 h) and terminal half-life was decreased (4.2 h versus 8.0 h) under fed conditions compared to fasted conditions. Similar food effect results were observed in the above study when one metaxalone 800 mg tablet was administered in place of two metaxalone 400 mg tablets. The increase in metaxalone exposure coinciding with a reduction in half-life may be attributed to more complete absorption of metaxalone in the presence of a high fat meal (Figure 1 ).
Distribution, Metabolism, and Excretion
Although plasma protein binding and absolute bioavailability of metaxalone are not known, the apparent volume of distribution (V/F ~ 800 L) and lipophilicity (log P = 2.42) of metaxalone suggest that the drug is extensively distributed in the tissues. Metaxalone is metabolized by the liver and excreted in the urine as unidentified metabolites. Hepatic Cytochrome P450 enzymes play a role in the metabolism of metaxalone. Specifically, CYP1A2, CYP2D6, CYP2E1, and CYP3A4 and, to a lesser extent, CYP2C8, CYP2C9, and CYP2C19 appear to metabolize metaxalone.
Metaxalone does not significantly inhibit major CYP enzymes such as CYP1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, CYP2E1, and CYP3A4. Metaxalone does not significantly induce major CYP enzymes such as CYP1A2, CYP2B6, and CYP3A4 in vitro.
Pharmacokinetics in Special Populations
Age
The effects of age on the pharmacokinetics of metaxalone were determined following single administration of two 400 mg tablets (800 mg) under fasted and fed conditions. The results were analyzed separately, as well as in combination with the results from three other studies. Using the combined data, the results indicate that the pharmacokinetics of metaxalone are significantly more affected by age under fasted conditions than under fed conditions, with bioavailability under fasted conditions increasing with age.
The bioavailability of metaxalone under fasted and fed conditions in three groups of healthy volunteers of varying age is shown in Table 2.
| Younger Volunteers | Older Volunteers | |||||
|---|---|---|---|---|---|---|
| Age (years) | 25.6 ± 8.7 | 39.3 ± 10.8 | 71.5 ± 5.0 | |||
| N | 59 | 21 | 23 | |||
| Food | Fasted | Fed | Fasted | Fed | Fasted | Fed |
| Cmax (ng/mL) | 1816 (43) | 3510 (41) | 2719 (46) | 2915 (55) | 3168 (43) | 3680 (59) |
| Tmax (h) | 3.0 (39) | 4.9 (48) | 3.0 (40) | 8.7 (91) | 2.6 (30) | 6.5 (67) |
| AUC0 -t (ng∙h/mL) | 14531 (47) | 20683 (41) | 19836 (40) | 20482 (37) | 23797 (45) | 24340 (48) |
| AUC∞ (ng∙h/mL) | 15045 (46) | 20833 (41) | 20490 (39) | 20815 (37) | 24194 (44) | 24704 (47) |
Gender
The effect of gender on the pharmacokinetics of metaxalone was assessed in an open label study, in which 48 healthy adult volunteers (24 males, 24 females) were administered two metaxalone 400 mg tablets (800 mg) under fasted conditions. The bioavailability of metaxalone was significantly higher in females compared to males as evidenced by Cmax (2115 ng/mL versus 1335 ng/mL) and AUC∞ (17884 ng∙h/mL versus 10328 ng∙h/mL). The mean half-life was 11.1 hours in females and 7.6 hours in males. The apparent volume of distribution of metaxalone was approximately 22% higher in males than in females, but not significantly different when adjusted for body weight. Similar findings were also seen when the previously described combined dataset was used in the analysis.
Indications and Usage for Lorvatus Pharmapak
Metaxalone is indicated as an adjunct to rest, physical therapy, and other measures for the relief of discomforts associated with acute, painful musculoskeletal conditions. The mode of action of this drug has not been clearly identified, but may be related to its sedative properties. Metaxalone does not directly relax tense skeletal muscles in man.
Contraindications
Known hypersensitivity to any components of this product. Known tendency to drug induced, hemolytic, or other anemias. Significantly impaired renal or hepatic function.
Precautions
Metaxalone should be administered with great care to patients with pre-existing liver damage. Serial liver function studies should be performed in these patients.
False-positive Benedict's tests, due to an unknown reducing substance, have been noted. A glucose- specific test will differentiate findings.
Taking metaxalone with food may enhance general CNS depression; elderly patients may be especially susceptible to this CNS effect. (See CLINICAL PHARMACOLOGY: Pharmacokinetics and PRECAUTIONS: Information for Patients section).
Information for Patients
Metaxalone may impair mental and/or physical abilities required for performance of hazardous tasks, such as operating machinery or driving a motor vehicle, especially when used with alcohol or other CNS depressants.
Drug Interactions
The sedative effects of metaxalone and other CNS depressants (e.g., alcohol, alcohol, benzodiazepines, opioids, tricyclic antidepressants) may be additive. Therefore, caution should be exercised with patients who take more than one of these CNS depressants simultaneously.
Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of metaxalone has not been determined.
Pregnancy
Reproduction studies in rats have not revealed evidence of impaired fertility or harm to the fetus due to metaxalone. Post marketing experience has not revealed evidence of fetal injury, but such experience cannot exclude the possibility of infrequent or subtle damage to the human fetus. Safe use of metaxalone has not been established with regard to possible adverse effects upon fetal development. Therefore, metaxalone tablets should not be used in women who are or may become pregnant and particularly during early pregnancy unless, in the judgement of the physician, the potential benefits outweigh the possible hazards.
Adverse Reactions/Side Effects
The most frequent reactions to metaxalone include:
CNS: drowsiness, dizziness, headache, and nervousness or "irritability". Digestive: nausea, vomiting, gastrointestinal upset.
Other adverse reactions are:
Immune System: hypersensitivity reaction, rash with or without pruritus; Hematologic: leukopenia; hemolytic anemia;
Hepatobiliary: jaundice.
Though rare, anaphylactoid reactions have been reported with metaxalone.
Overdosage
Deaths by deliberate or accidental overdose have occurred with metaxalone, particularly in combination with antidepressants, and have been reported with this class of drug in combination with alcohol.
When determining the LD50 in rats and mice, progressive sedation, hypnosis and finally respiratory failure were noted as the dosage increased. In dogs, no LD50 could be determined as the higher doses produced an emetic action in 15 to 30 minutes.
Lorvatus Pharmapak Dosage and Administration
The recommended dose for adults and children over 12 years of age is one 800 mg tablet three to four times a day.
How is Lorvatus Pharmapak supplied
Metaxalone is available as an 800 mg, light pink to pink, capsule shaped, scored uncoated tablet with debossing 'AN' on the left side of the scoring and '553' on the right side of the scoring. Other side of the tablet is plain.
They are available as follows:
Bottles of 30: NDC 51021-333-30
Bottles of 60: NDC 51021-333-60
For Questions or Comments, please call 1-888-452-9975 or fax to 1-888-452-9975
Rx Only
Distributed By:
Sircle Laboratories, LLC
Madison, MS 39110
Indications and Usage for Lorvatus Pharmapak
- Antiseptic cleanser
- Kills harmful bacteria and germs
- First aid to help prevent infection
Warnings
- For External Use Only
- Avoid contact with the eyes. If contact occurs, flush eyes with water.
- Flammable, keep away from fire or flame.
Lorvatus Pharmapak Dosage and Administration
- Use as part of your daily cleansing routine
- May be covered with a steril bandage
Use with Kit
Open one wipe, apply topically as needed and let dry before applying Diclofenac Solution.
- Discard after single use
- Sterile unless pouch is opened or damaged
- Latex Free
NDC 67777-121-14
Manufactured for: Dynarex Corporation, Orangeburg, NY 10962
PRINCIPAL DISPLAY PANEL - Kit Carton
NDC 51021-274-01
Rx Only
Lorvatus™ PharmaPak
metaxalone tablets & diclofenac sodium topical solution
800mg tablets / 1.5% topical solution w/w
Kit Contents:
Metaxalone 800mg tablets: Each tablet contains 800 mg metaxalone and the following inactive ingredients: calcium carbonate,
FD&C Red #40, hypromellose, lactose monohydrate, microcrystalline cellulose, povidone, silicone dioxide, sodium starch glycolate
and sodium stearyl fumarate.
Diclofenac Sodium 1.5% Topical Solution: Each 1 mL of solution contains 16.05 mg of diclofenac sodium. In addition diclofenac sodium topical
solution contains the following inactive ingredients: dimethyl sulfoxide USP (DMSO, 45.5% w/w), propylene glycol, alcohol, glycerin and purified water.
Sterile Alcohol Prep Pads: Each pad contains Isopropyl Alcohol, 70% v/v and the following inactive ingredient: water.
*Sterile as long as the package remains unopened and undamaged

| LORVATUS PHARMAPAK
diclofenac sodium, metaxalone, and isopropyl alcohol kit |
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
|
||||||||||||||||||||||
| Labeler - Sircle Laboratories, LLC (962175621) |